10 reasons why pandemic fatigue could threaten global health in 2021
Being in a constant state of high alert and uncertainty is exhausting yet health officials warn that we can’t let our guard down yet and resisting living with the ‘new normal’ could threaten our health.
- 23 September 2020
- 6 min read
- by Priya Joi

The COVID-19 pandemic has meant that as a species we have collectively gone into a form of flight-or-fight mode, an evolutionary self-defence mechanism that can kick in when faced with a crisis. But what happens when that crisis lasts for months with no end in sight? For many, this protracted emergency is resulting in pandemic fatigue. But what does that mean exactly, and could it breed a form of complacency that could spell trouble for the fight against COVID-19 in 2021?
1. Pandemic fatigue should not be confused with post-COVID-fatigue
Many people who have had even mild cases of COVID-19 can have post-viral fatigue that can last for months or even years. This can include feeling constantly tired, with aching muscles and brain fog. Instead, pandemic fatigue refers to feeling overwhelmed with still having to maintain a state of constant vigilance, in this case six months after the pandemic started, and a weariness to abide by restrictions.
2. Collateral damage from the pandemic
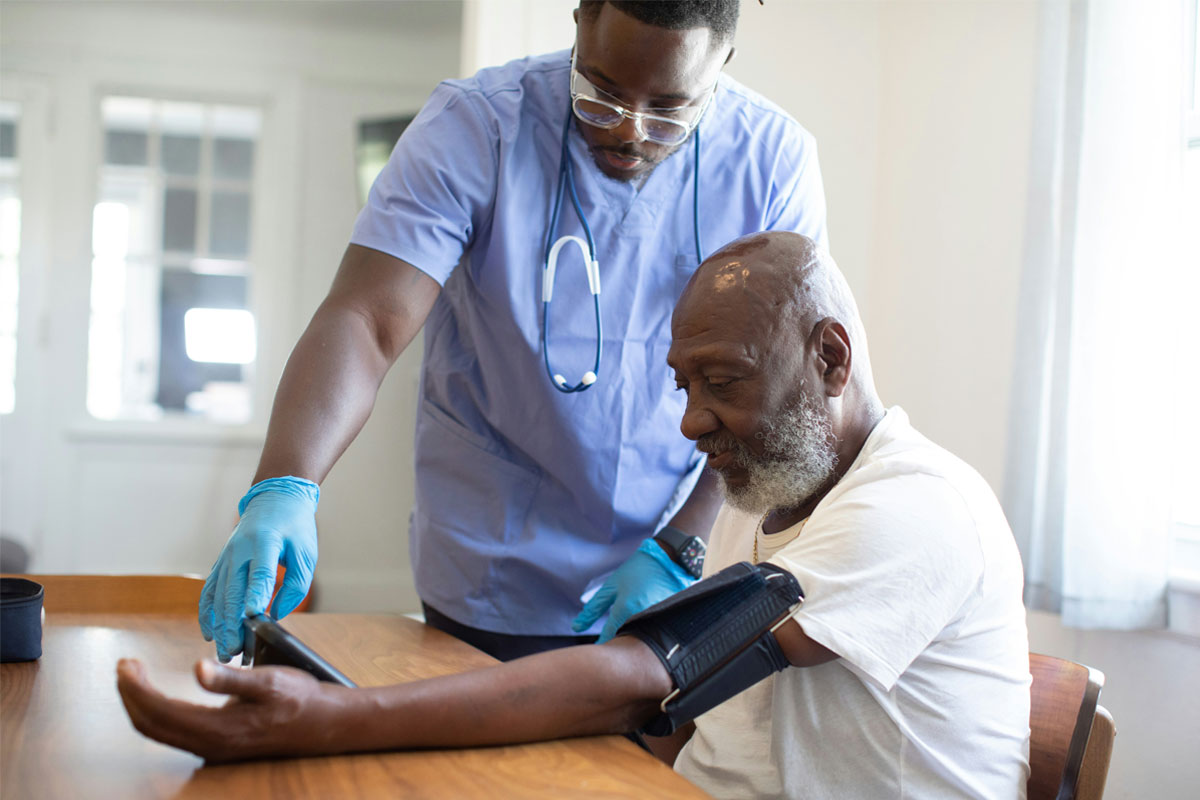
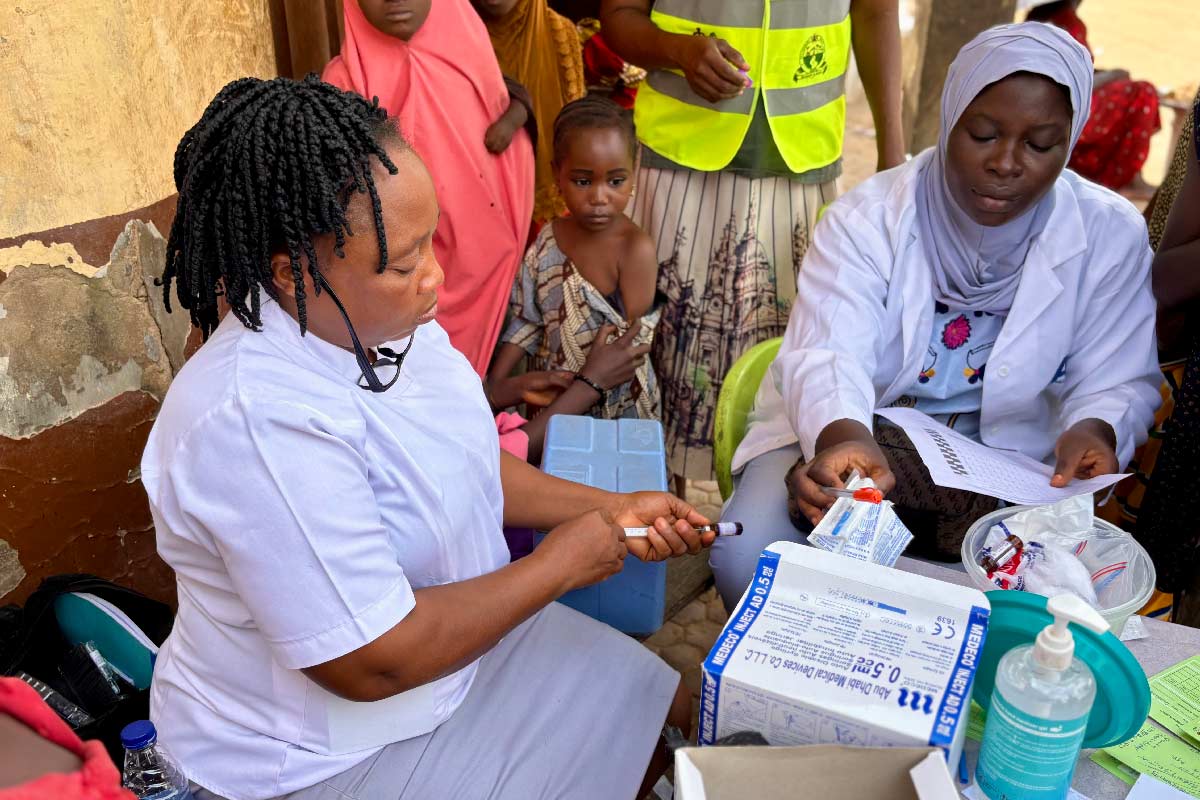
COVID-19 has infected more than 30 million people and killed nearly one million. These numbers seemed unthinkable at the start of the pandemic, but we are now having to accept that the numbers are likely to continue to rise especially as some countries start to enter their second wave of infections. This alone will exert a huge toll on human health. But the collateral damage is devastating too; the loss of incomes, the closure of entire swathes of community services and a lack of access to non-COVID-19 health services, including routine immunisation, is causing widespread insecurity and uncertainty about both the present and the future.
3. Mental health challenges
This emotional overwhelm can understandably lead to or exacerbate mental health problems, such as depression and anxiety. Health experts around the world have warned of a rise in the need for mental health services, which in the UK has been estimated at a 20% increase. A study in April this year looking at mental distress in more than 2,000 Americans indicated that 28% showed signs of serious mental illness compared with 3.4 in a similar survey in 2018. Young adults (18-44 years) showed the biggest downward change, and they were ten times more likely to have mental health issues.
4. The lingering effects of lockdown
Even for people who have not developed mental health problems, the weeks of lockdown and restrictions that millions went through brought emotional and psychological challenges that few had ever experienced. For many, those stresses may have lifted when lockdown eased, with schools and offices re-opening along with restaurants and gyms. Yet countries, such as Spain and the UK, are potentially facing new restrictions that might include another lockdown. Israel just went back into its second lockdown as it has one of the highest COVID-19 infection rates in the world. It’s unclear how people will cope with a second lockdown. In many low- and middle-income countries lockdown has proven disastrous. In India, 400 million workers in the informal sector - 80% of India’s non-agricultural workforce - are now at risk of falling into poverty as a result of the crisis.
Have you read?
5. Complacency about wearing masks and physical distancing
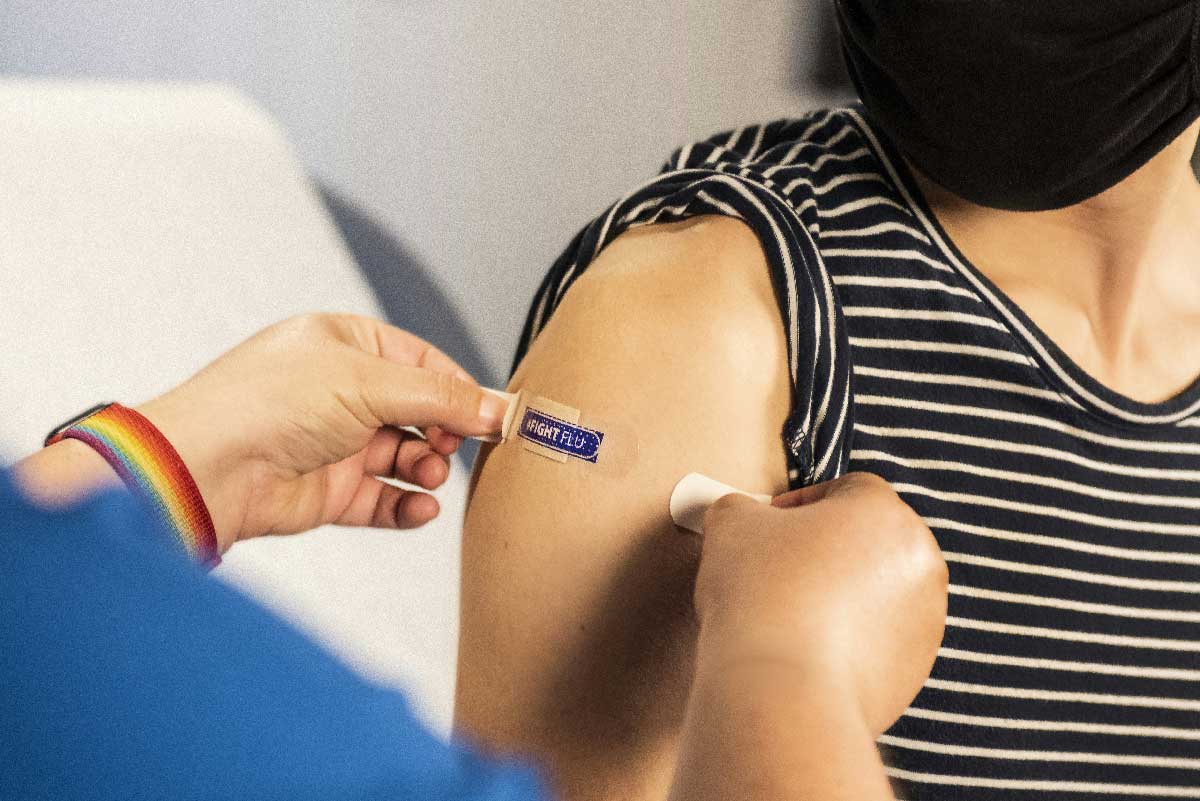
Although face-coverings and physical distancing is still mandatory in public spaces in most countries, there are many reports of people either not wearing masks or wearing them ineffectively. Equally, despite pavements and floors in shops and airports painted to indicate the distance that people should keep apart, often they are not heeded. Yet masks are unlikely to go away as a disease prevention tool for COVID-19, and moreover there is evidence that countries that introduced masks early on had milder epidemics. People in countries where the pandemic has yet to fully take-off, may also be complacent in continuing to comply with restrictions, in the believe that the threat is over.
6. The risk of re-infection in people who have had COVID-19
People who have had COVID-19 and have antibodies may feel that they are fairly well protected as they may have natural immunity to further infections. Yet natural immunity may not last long and there are documented cases of re-infection, sometimes leading to asymptomatic disease, but occasionally sending the person into intensive care. Some scientists believe that when a person is re-infected, they are protected by their antibodies from severe disease. But so far, it’s not clear how long antibodies last for, which also has implications for vaccine development.
7. Confusion over COVID-19 restrictions
Some pandemic fatigue seems to be caused by conflicting public health messaging in many countries. During lockdown, the rules in some countries were so strict that they were fairly unambiguous. Now, after the easing of lockdowns in many places, some countries are reintroducing restrictions of varying levels following rising numbers of cases. These constantly changing measures can cause confusion over what people should and shouldn’t do, for example, how schools should respond to students testing positive for COVID-19 or differences in messaging between local and national governments.
8. Misinformation and why people still don’t believe COVID-19 is a threat
An infodemic of misinformation about COVID-19 has threatened the COVID-19 response since the start of the pandemic. This includes false claims that it would be better to get the virus (in the belief that antibodies would then protect against further infection), that the disease is not as bad as people have been led to believe or even whether or not the virus is real. All of this can not only put people at risk by not following guidance such as wearing masks, but it can also put more vulnerable people in society at risk, as well as encouraging the spread of non-scientific information.
9. Failing to learn lessons can be disastrous for the future
Even when we are past the acute phase of this COVID-19 crisis, pandemic fatigue could threaten future disease prevention. Just three years after the H1N1 flu pandemic, World Health Organization (WHO) officials noted that health experts were unwilling to analyse it anymore to influence future pandemic planning, and were keen to move on. Yet such guidance based on lessons learned can be especially important for low- and middle-income countries that lack the resources to develop their own plans. A failure to plan also tends to mean a waste of resources – global health experts estimate it costs around US$ 4.5 billion a year globally to properly prepare for pandemics. By contrast, responding to the pandemic is costing low-and middle-income countries on average a staggering US$ 52·45 billion every four weeks.
10. Life in 2021 will require as much vigilance
Many people are understandably keen to see the end of 2020, but public health experts are keen to point out that nothing will materially change on 1 January 2021. Comprehensive testing and contact tracing programmes are yet to be successfully rolled out anywhere in the world, even in high-income countries. Scientists have modelled future scenarios of how the pandemic may evolve, none of which include a scenario in which the virus disappears. By the end of 2020, we are unlikely to have a treatment or a vaccine, and when we do get a vaccine, the logistics of manufacturing and distribution are not insignificant.