COVID vaccines don’t just benefit physical health – they improve mental health too
The mental wellbeing benefits associated with COVID vaccination were substantial among older and clinically vulnerable people, but negligible for younger adults.
- 4 November 2022
- 4 min read
- by The Conversation
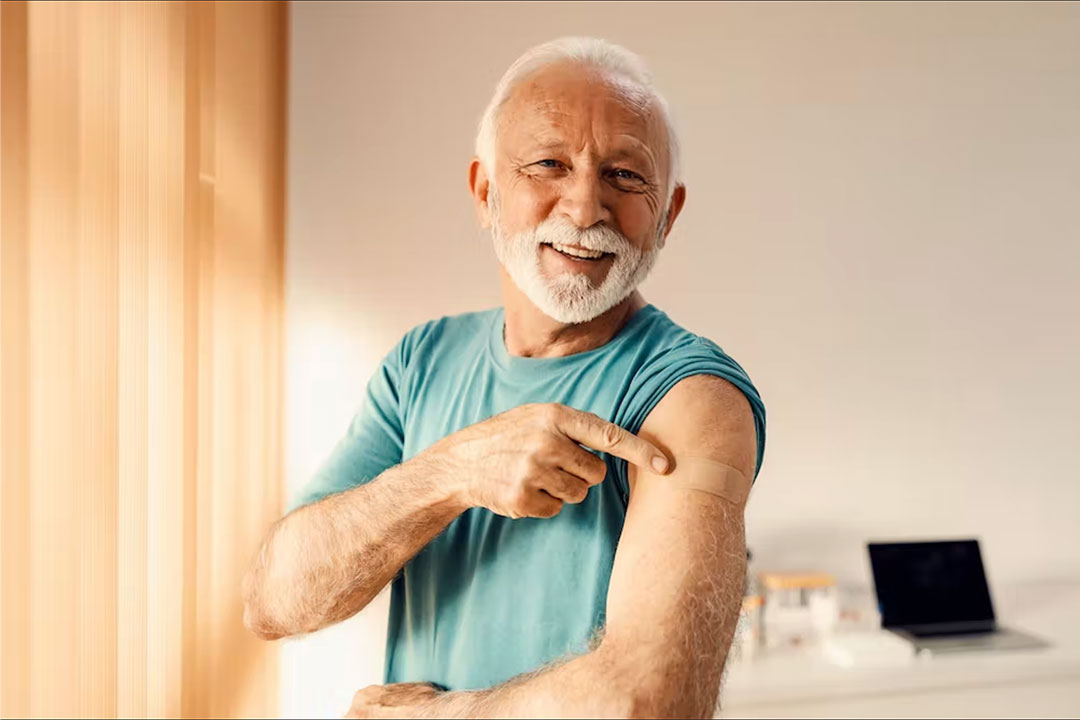
The considerable physical health benefits of COVID vaccines, in particular, the significantly reduced risk of serious illness, hospitalisation and death from the virus, are well known.
But what about the benefits of vaccination for mental health? Does vaccination help to lessen the psychological distress associated with COVID? And if so, how substantial are the positive effects?
We speculated that COVID vaccination would be beneficial for people’s mental wellbeing as it may reduce the anxiety surrounding COVID (at least, regarding a person’s own health).
In a new study, using data from thousands of UK adults, we’ve shown that vaccination is linked to a significant easing in the psychological distress associated with COVID.
To understand the benefits of vaccination on mental health, we compared the mental wellbeing of people who had received the vaccine (one or two doses) with those who had not. We used data from the UK Household Longitudinal Study, a large annual household survey that captures a wide range of information from adults living in the UK. We looked specifically at data collected between January and March 2021.
The measure of mental wellbeing used in this study was the General Health Questionnaire. It consists of a 12-item scale designed to assess stress, anxiety and happiness.
One issue with simply comparing the mental wellbeing of both groups (those who had been vaccinated, and those who had not) is that there may be important differences between them. This may mean that we could mistake differences between the mental wellbeing of the groups as being due to vaccination when they could be a result of other factors.
Our approach to this potential problem was to match both groups carefully, so that the people who were vaccinated were very similar to those who were not, for example, in characteristics like age.
We also had a variable in the survey capturing whether people were willing to take a vaccine, which meant that we could match both groups based on their willingness to be vaccinated. This could be important as people who refuse a vaccine, for example, due to a lower trust in the government, may have lower wellbeing in the first place.
Our results suggest that for the group of people who were vaccinated, vaccination led to a large reduction in their psychological distress.
To understand how large this estimated effect was, we compared it with the estimated effect of other major life events on mental wellbeing (taken from other studies). The benefit for wellbeing in the vaccinated group was equivalent to about half to two-thirds of the mental wellbeing benefits associated with moving from unemployment to full employment.
Have you read?
Differences across age groups
We must note that while just under half of the respondents in our sample were vaccinated, owing to the phased rollout of COVID vaccines, this was also the half that was most likely to be at risk from a COVID infection.
That said, we had significant numbers of people across all age groups who were vaccinated.
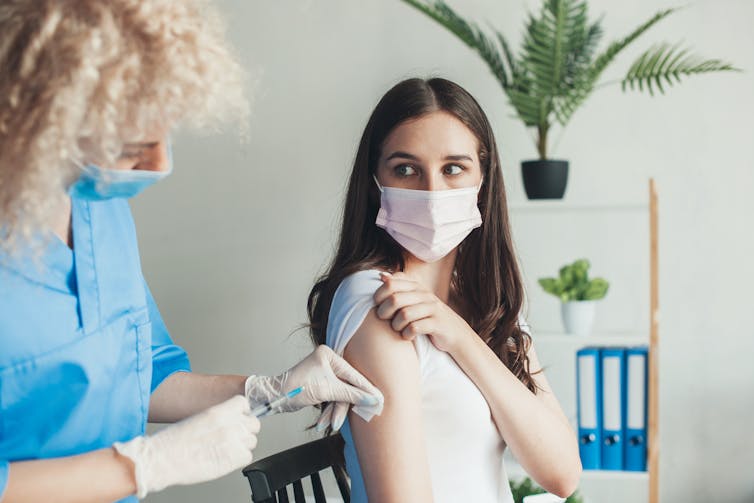
We looked to see if there was any difference in the benefits of vaccination for mental wellbeing across different groups. Specifically, we compared the estimated mental wellbeing benefits of vaccination for people under the average (median) age (56) in our sample with those above this age. We also compared people who were classified as “clinically vulnerable” (people at greater risk of harm from an infection) with those who were not.
We found that the mental wellbeing benefits associated with vaccination were heavily concentrated on the older and clinically vulnerable groups. Our proposed explanation is that in the absence of vaccination, anxiety about contracting COVID would be particularly strong for this group.
On the other hand, when looking at younger groups who were not clinically vulnerable, we found little evidence to suggest that vaccination led to a substantial improvement in their mental wellbeing.
It’s perhaps worth noting here that despite a successful COVID vaccination drive in the UK overall, younger groups are most likely to express vaccine hesitancy.
Our findings may help to explain this. For young people, not taking up the vaccine may be primarily due to a lack of perceived benefits for their own wellbeing (weighed up alongside any perceived costs), as opposed to vaccine hesitancy in all cases.![]()
Authors
Kausik Chaudhuri, Senior Lecturer in Economics, University of Leeds
Peter Howley, Professor of Economics and Behavioural Science, University of Leeds

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
The authors do not work for, consult, own shares in or receive funding from any company or organisation that would benefit from this article, and have disclosed no relevant affiliations beyond their academic appointment.
Partners
University of Leeds provides funding as a founding partner of The Conversation UK.








