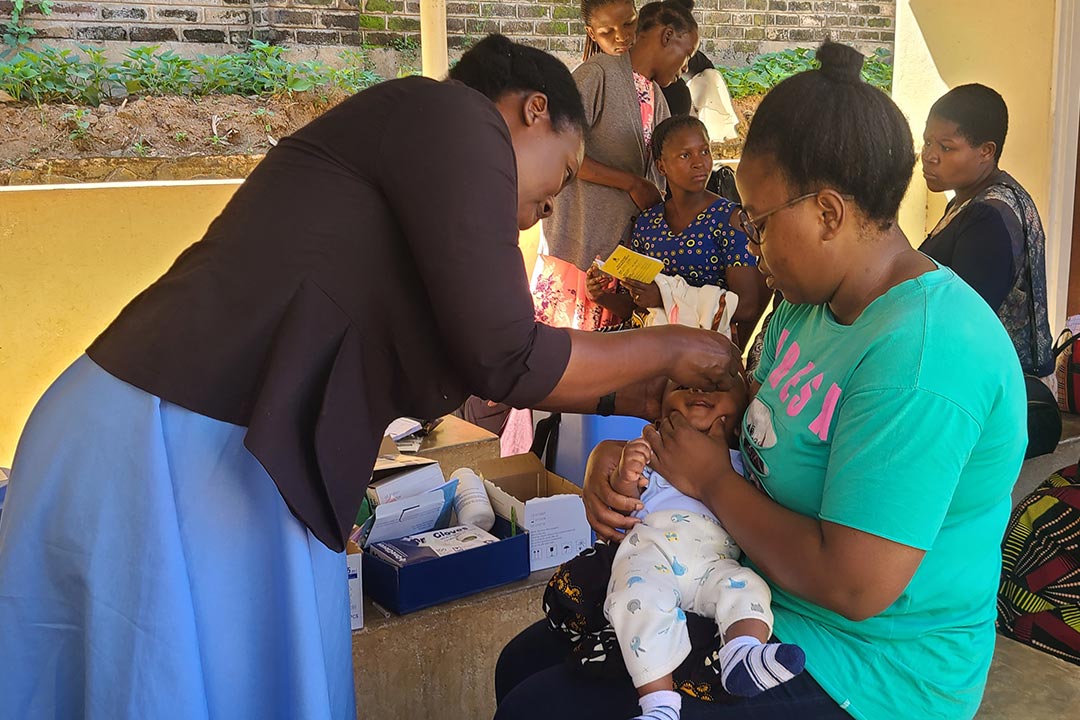
My malaria story: living in hope
Growing up in malaria-endemic Ghana, Ernest’s childhood was riddled with regular battles to survive infection, leaving him with traumatic memories of experiences he still struggles to recall. Now working at Gavi, Ernest shares how the roll-out of the first malaria vaccine in Ghana has given him renewed hope for the health and prosperity of the next generation – if it’s funded properly.
- 31 October 2022
- 5 min read
- by Ernest Aboagye

Before turning 16 years old, I had malaria fever at least 30 times.
It was a challenge, both mentally and financially for my parents each time my brother and I were sick, given the frequency with which we were both suffering from malaria. I remember the nationwide campaign promoting mosquito coils to try and keep this national threat at bay.
The disease was so widespread within my community that being sick with malaria was not an excuse for absenteeism. My teachers claimed, “Everyone gets it, it’s normal,” and as long as I could walk and eat, I was expected to come to school.
The disease was so widespread within my community that being sick with malaria was not an excuse for absenteeism. My teachers claimed, “Everyone gets it, it’s normal,” and as long as I could walk and eat, I was expected to come to school, irrespective of the other symptoms.
At home, it was a battle to survive each time I was sick, but my friends and I would find the sense of humour to laugh about it, counting how many times each of us had been infected and how long it took to recover – mocking those who took longer.
These are not the best of my childhood memories, and not experiences I like to recall, but they were triggered again by the ground-breaking discovery of the malaria vaccine. In October last year, I read the World Health Organization (WHO) news release recommending the widespread use of the RTS,S/AS01 (RTS,S) malaria vaccine for children in sub-Saharan Africa, and immediately shared it with friends and family.
Hopefully, this historic achievement can erase some of my childhood traumas triggered by malaria. I am thankful there is now a vaccine that can help reduce the prevalence of malaria, which typically affects households and communities with fewer financial resources.
Foremost among the challenges that lead to the spread of malaria in sub-Saharan Africa (SSA) are poverty and climate suitability. Poverty is both a source and a result of the disease. It thrives in locations with poor living circumstances that favour mosquito breeding, and among people with low socio-economic status who often cannot access quality health care.1
This historic achievement can erase some of my childhood traumas triggered by malaria. I am thankful there is now a vaccine that can help reduce the prevalence of malaria.
Numerous vector-borne diseases have been dubbed “diseases of poverty” due to their strong association with socially vulnerable communities. In addition, research demonstrates that the socioeconomic status of the family has a substantial effect on the number of hospitalised children with malaria: children from lower socio-economic status homes had a significantly higher likelihood of developing malaria compared to those from high economic status homes.
The climate (high temperature and abundant rainfall) in SSA is suitable for the reproduction and propagation of the female anopheles mosquito. The region’s climatic characteristics are conducive to seasonal and endemic malaria transmissions. The mosquitoes are immune to the pyrethroid pesticides used in ITNs, and are resistant to antimalarial drugs, making it challenging to control the disease in the SSA region.
Have you read?
The result? More than 260,000 children in Africa under the age of five die from malaria annually. The 2021 World Malaria Report states that in the nations where the disease is most common, efforts to combat malaria have slowed or stagnated in recent years.
But the promising findings of the pilot roll-out of the GSK Mosquirix vaccinations in Ghana, Malawi and Kenya, which prompted the WHO to advocate wider use among children in SSA and other regions, are evidence of progress. Even though my generation did not have access to the vaccine, the ongoing pilot programme has already reached more than a million children.
However vaccine introduction does not equal vaccine accessibility. That's why Gavi has made an initial investment of US$ 155.7 million for 2022-2025 to initiate the implementation of the vaccine. As iterated by Dr Seth Berkley, CEO of Gavi, the Vaccine Alliance, “The vaccine is an important additional tool to control malaria in Africa, alongside other interventions such as routine use of insecticide-treated bed nets, indoor spraying with insecticides, malaria chemoprevention, and timely testing and treatment.”
Continued financing is required for dissemination and research innovation. The expected yearly investment in R&D for malaria-related research for the period 2021-2030 is US$ 851 million, underscoring the necessity to continue investing in strategies to combat the disease. In addition, the WHO and its partners welcome new methods and technologies for malaria vector control, antimalarial medicines, and drug resistance.
I am happy to express my gratitude for the creation of the malaria vaccine and am grateful for having survived so many cases of the disease. Malaria is a fatal yet curable disease and its eradication requires cooperation from many sectors. Without a doubt, WHO’s collaboration with Gavi, the Vaccine Alliance, and other partners to prevent diseases and deaths by providing vaccines is a significant step that should be encouraged and applauded. It contributes to putting smiles on people’s faces while preventing tens of thousands of illnesses and deaths.
Even though the pandemic and current conflicts have had a substantial influence on global immunisation coverage, there is an ongoing need for programmatic support to regain lost ground and preserve lives.
1. Gallup JL, Sachs JD. The economic burden of malaria. In: The intolerable burden of malaria: a new look at the numbers: Supplement to Volume 64(1) of the American Journal of Tropical Medicine and Hygiene. 2001. https://www.ncbi.nlm.nih.gov/books/NBK2624/