Planting before the rain: in Cameroon, a grieving woman reconsiders vaccination
Victorine’s sister died of cervical cancer. Her children will be safer because of the loss.
- 12 March 2026
- 5 min read
- by Delphine Fri Chifor
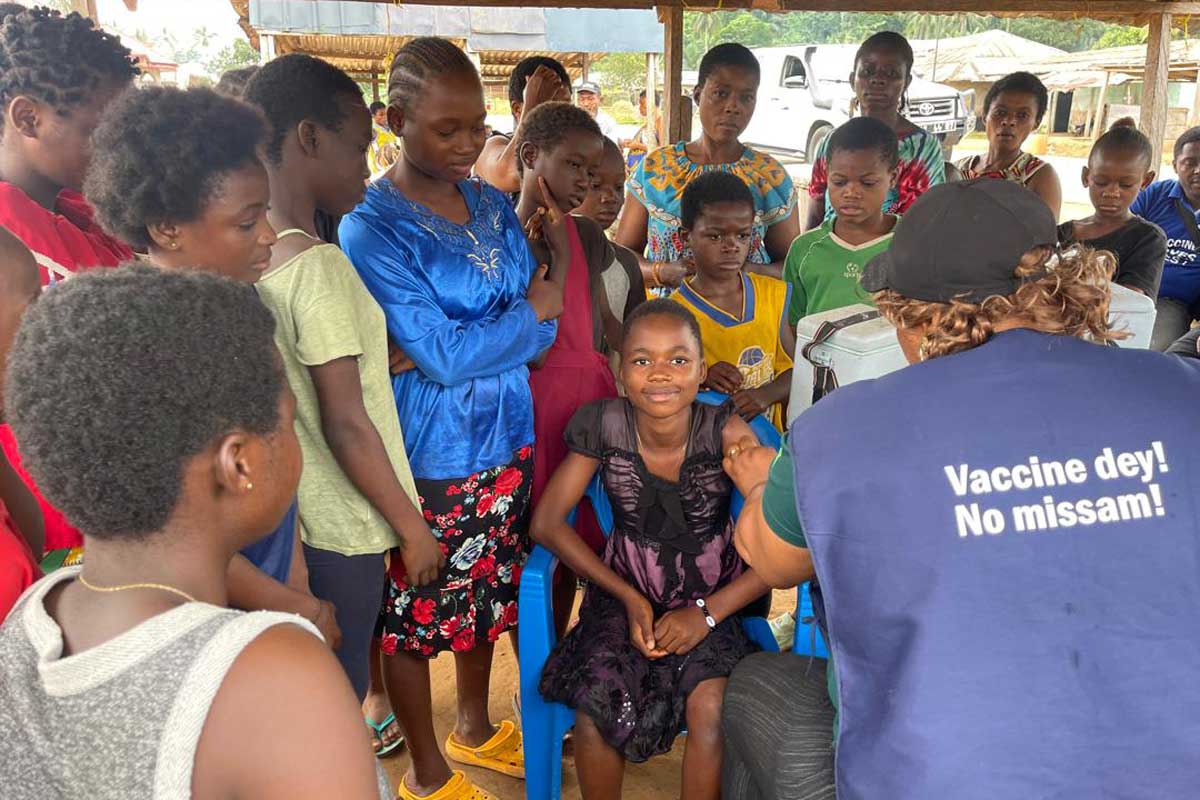
The rain had done its work.
After weeks bent in half over the red soil, labouring to get the crops planted before the heavy clouds broke over her village in Nguti, Southwest Region of Cameroon, Victorine finally allowed herself to rest.
Now the first downpour had washed the dust from the leaves and pressed the seeds deep into the earth. The crops will be plentiful because I did the needful, she thought to herself.
That morning, she intended to sleep in, but just as the first cock crowed, a town crier’s voice cut through the damp air, announcing the coming of a vaccination team into her community that morning. “Children will receive routine antigens and vaccines for those over five years old, including HPV,” he announced.
Victorine pulled the blanket tighter around her shoulders. She was exhausted. But a promise she had made to herself tugged at her conscience, preventing her from slipping back into sleep.
A few months before, Victorine had buried her sister. She had lost her to cervical cancer. In the long days that followed the funeral, Victorine had slowly stitched together fragments of information that had somehow, previously, refused to make sense.
It was a difficult fact to process that cervical cancer had killed her sister, despite being largely preventable. Regular screening could have caught it early enough to cure. What resonated even more was the fact that a vaccine that protected against the virus responsible for almost all cervical cancers was available for free for young adolescents.
She had once dismissed the human papillomavirus (HPV) vaccine after hearing about it on the radio. Many in her community had done the same. But grief changed everything for her. “I could not afford it for myself,” she said quietly, referring to the steep cost of the vaccine on the private market. “But I knew from that day that I needed to do something for my children.”
When facts are not enough
In Cameroon, the HPV vaccine was introduced into the Expanded Programme on Immunization in October 2020, for girls aged 9 to 14. In 2022, it was extended to boys of the same age group to prevent cancers linked to HPV, including cervical, anal, oropharyngeal, penile, vaginal and vulvar cancers, as well as genital warts.
Cervical cancer alone remains a serious burden in Cameroon, with around 2,770 women being diagnosed each year and approximately 1,787 dying from it, and it remains one of the leading cancers among women aged 15 to 44.
Unfortunately, factual data is often insufficient to change behaviour in the community, whose health-seeking behaviours are shaped by diverse factors.

In many under-served communities in the Northwest and Southwest regions, HPV vaccine hesitancy seemed to take root at the moment of introduction. Some myths falsely framed the vaccine as a population control strategy. For many parents, the vaccine itself seemed like an abstract solution to a distant or even foreign ailment.
Victorine’s experience made her realise that the risk lived closer to home than she could have imagined. She had searched for the vaccine for her eligible children at her local primary health care unit, but it was unavailable. Then another mother told her that the Cameroon Baptist Convention Health Services (CBCHS) vaccination team sometimes brought HPV vaccines during their outreach sessions.
“Next time I hear they are coming, I will go,” she had promised herself.
Have you read?
An integrated approach that ensures the well-being of everyone
The CBCHS immunisation programme does not focus only on children under five. Its integrated approach bundles routine childhood vaccines, HPV vaccination, and other antigens and supplements, as well as humanitarian services, into a single outreach package.
This strategy, initially designed to reach zero-dose children, has broadened its scope, reaching more families through its integrated strategy.
That morning, Victorine did not wait; she rose at the first light and walked with her children to the vaccination site. They were the first family to arrive.
“I did not want to take chances,” she said. “I already feel bad that I cannot afford the vaccine [privately] for my 18-year-old daughter. But at least the three others will receive this life-saving protection. If my sister had taken it, she might still be alive. We could not help her, but we can help the next generation.”
While not every family has experienced the personal loss that transformed Victorine’s perspective, the combination of community education and consistent vaccine availability is changing minds.
Through its integrated outreach, the CBCHS immunisation programme has administered HPV vaccines to more than 9,000 children in under-served communities across the two regions. What began as an effort to reach zero-dose children is now also protecting adolescents from future cancers.
Meanwhile, Victorine says that watching her crops sprout after she took care to sow the seeds before the storms, puts her in mind of the immune shield she’s made sure to extend to her children before the virus can take hold. Both choices contain the promise of a better, safer future.
How is Gavi helping?
Gavi is supporting CBCHS in Cameroon through three funding streams.
One stream provides direct funding to CBCHS through the ZIP Humanitarian Partnership to expand efforts to reach zero-dose and under-immunised children in 12 fragile districts of the Northwest and Southwest regions, which find themselves in humanitarian crisis.
A second stream provides support through Gavi CSO Fund Manager MannionDaniels, to strengthen delivery and community engagement strategies in 22 priority districts countrywide.
A third stream comes through the Full Portfolio Planning (FPP) process led by the Expanded Programme on Immunization, which aligns partner efforts and resources to strengthen routine CSO involvement in immunisation in Cameroon.
Together, these three streams enable CBCHS to conduct targeted outreach, strengthen community engagement, and reach children in 22 vulnerable districts across five regions.








