Progress has slowed on universal health coverage: Here's what needs to happen
One of the targets of Sustainable Development Goal 3 is universal health coverage, but progress has been slowing since 2015. Here’s what you need to know.
- 18 October 2023
- 5 min read
- by World Economic Forum
Since the Sustainable Development Goals were set in 2015, progress towards achieving universal health coverage (UHC), one of the targets set in Goal 3: Good Health and Well-being, has stagnated.
UHC means "all people – no matter who they are or where they live – can receive quality health services, when and where they are needed, without incurring financial hardship", according to a new report from the World Health Organization (WHO) and the World Bank.
But around 4.5 billion people – half the world's population – were not covered by essential health services in 2021, finds the Tracking Universal Health Coverage: 2023 Global Monitoring Report.
Since 2015, most countries (108 out of 194) experienced "worsening or no significant change in service coverage", says the report.
And, even before the pandemic, 2 billion faced financial hardship due to spending on health in 2019, and of those, 344 million were living in extreme poverty.
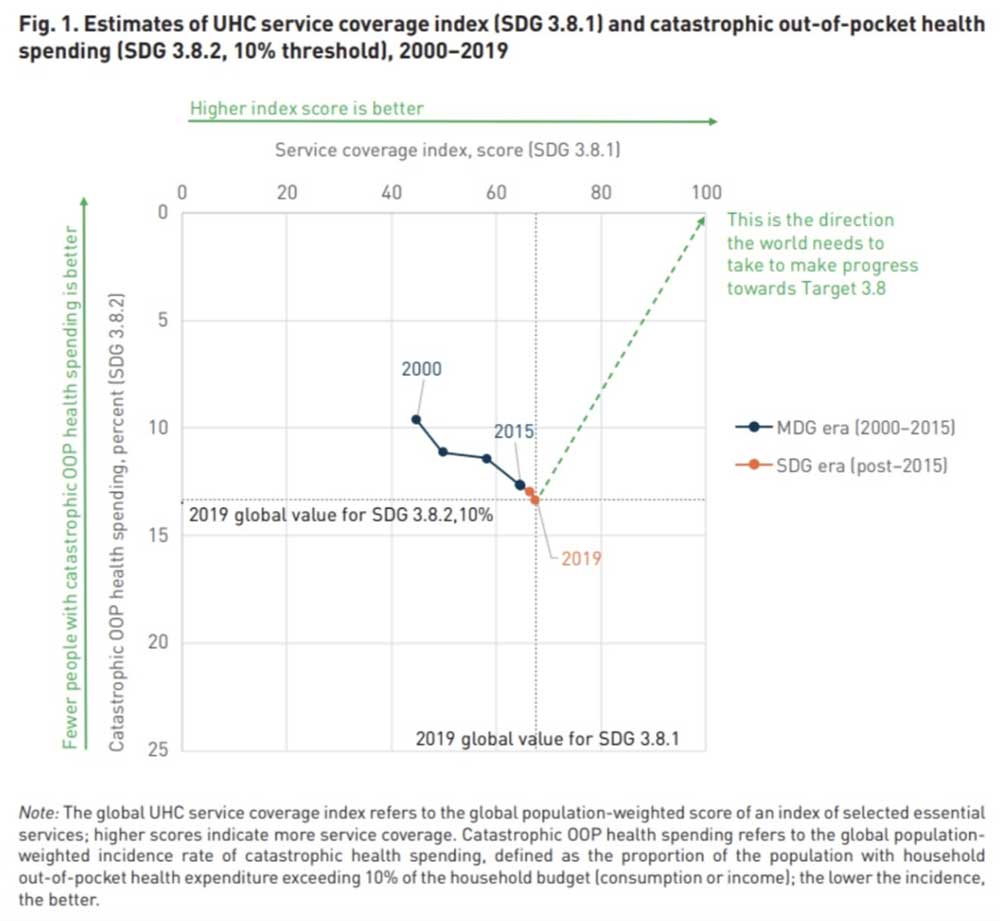
Image: WHO/World Bank
The report looks at two indicators – the UHC service coverage index (SCI) and catastrophic out-of-pocket (OOP) health spending. Here are some of the report's main findings:
A snapshot of the state of UHC
Only a few countries have managed to improve service coverage and reduce catastrophic OOP health spending.
In the two decades since 2000, only 42 of the 138 countries with data available have improved in both UHC – expanding health coverage and reducing OOP spending.
Substantial progress in expanding UHC was made in those 20 years – with the global UHC SCI score increasing from 45 to 68 out of 100 between 2000 and 2021. But, across the globe, progress has slowed in recent years.
The biggest improvements in the UHC service coverage index were in low-income countries and lower-middle-income countries, but they also saw the largest increases in catastrophic OOP health spending.
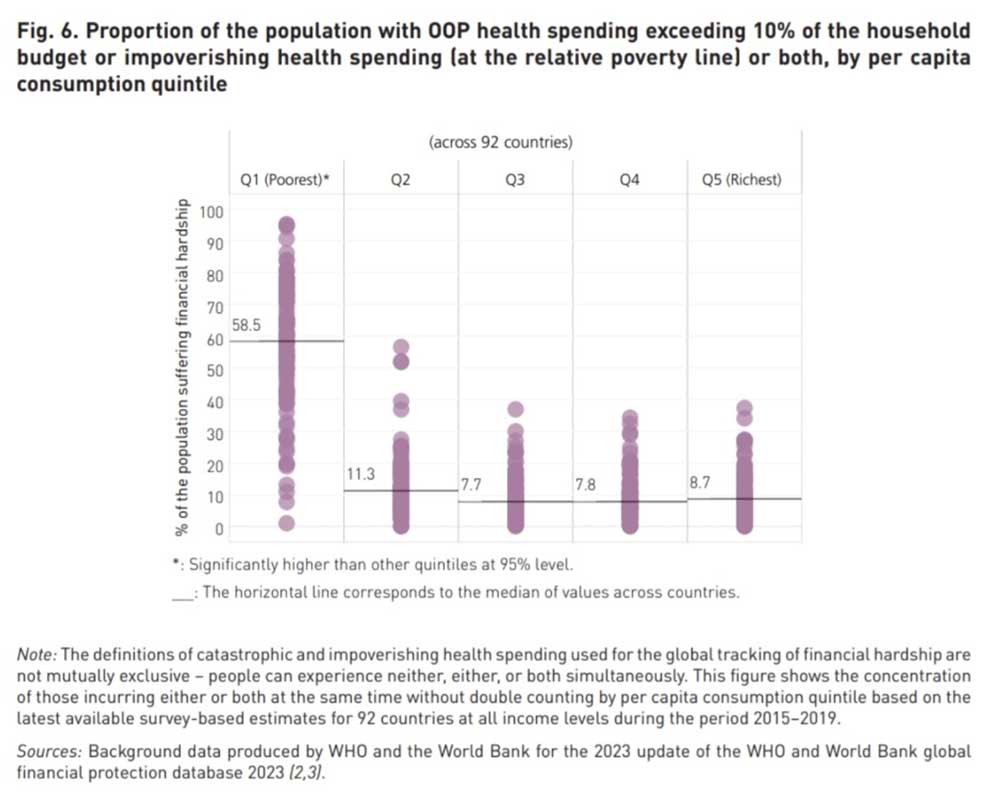
Image: WHO/World Bank
COVID-19 has had an impact: the global SCI score did not change between 2019 and 2021, as healthcare resources were diverted to dealing with the pandemic.
"The combined macroeconomic, fiscal, and health impacts of the pandemic, and emerging evidence on rising poverty, led to the weakening of financial protection globally, with higher rates of forgone care due to financial barriers and more people incurring financial hardship due to catastrophic and impoverishing OOP spending," says the report.
There are discrepancies in the coverage for different areas of health. Infectious diseases, including tuberculosis, have seen the most significant improvement in service coverage, with an average of 7% per year.
But the report warns that reductions in coverage levels could lead to rapid increases in disease burden, potentially exacerbated by multiple crises, such as the expansion of infectious disease vector habitats due to global climate change.
Whereas, before 2015, noncommunicable diseases and reproductive, maternal, newborn and child health only saw small improvements of 1% or less, with little or no improvements since.
Have you read?
Since 2000, the number of people facing financial hardship due to spending more than 10% of their household budget on health expenses has increased by 76% and passed 1 billion in 2019.
"Catastrophic OOP health spending reduces households' ability to consume other essential goods and services such as food, shelter, clothing, or education," according to the report.
It's estimated that 2 billion people experienced catastrophic spending, or impoverishing health spending at the relative poverty line.
What needs to happen to get back on track?
Urgent political action is needed to achieve UHC by 2030, say WHO Director-General Dr Tedros Adhanom Ghebreyesus, and World Bank Group President Ajay Banga.
"Reaching the goal of UHC by 2030 requires substantial public sector investment and accelerated action by governments and partners, building on solid evidence and reorienting health systems to a primary health care approach, to advance equity in both the delivery of essential health services and financial protection."
To achieve this goal, "modern, fit-for-purpose" health information systems are also necessary to support policy development, they add.
"Such shifts are essential as we continue to respond to and recover from the COVID-19 pandemic's impacts on health systems and the health workforce, and as the challenges posed by deepening macroeconomic, climate, demographic, and political trends threaten to reverse hard-won health gains around the world."
Earlier this year, the World Economic Forum and L.E.K. Consulting laid out a shared health and healthcare vision for 2035: to achieve equity, transform healthcare systems, encourage innovation and secure global environmental sustainability, with equity as the foundation.

Image: World Economic Forum
Across four strategic pillars, the Global Health and Healthcare Strategic Outlook: Shaping the Future of Health and Healthcare pre-empts potential barriers both public and private stakeholders may face, and demonstrates ways to mitigate these through case studies from across the world.
"Lack of access to essential health services is not only a matter of inconvenience; it's a stark reminder of the inequality that still plagues our world. It's a call to action, a plea for change, and a reminder that health is a basic human right we must ensure for all," said Shyam Bishen, Executive Committee Member and Head of the Centre for Health & Healthcare at the World Economic Forum.
"We at the centre have established a Global Health Equity Network to help solve this access challenge. In addition, we are working on improving the overall health system through digital healthcare transformation, which will help create better efficiencies and access."
Written by
Kate Whiting Senior Writer, Forum Agenda
Website
This article was originally published by the World Economic Forum on 13 October 2023.









