Meet the Benin woman fighting FGM and vaccine-preventable disease
Sanny Taïbatou, a survivor of female genital mutilation (FGM), devotes her days to teaching communities to shield girls’ bodies from both pathogens and the knife.
- 6 March 2026
- 7 min read
- by Edna Fleure

At a glance
- Sanny Taïbatou’s earliest attempts to raise awareness against female genital mutilation (FGM) in the pockets of northern Benin where the practice is ongoing, ended in failure.
- Since then, she’s learned that information about the risks are not enough. What’s demanded is a sensitive renegotiation of the meaning of protection – a conversation that also includes vaccination.
- As one mother credits Taïbatou with sparing her daughter the ordeal she suffered, another says simply: “Taïbatou is our lucky star.”
On 6 February 2026, the International Day of Zero Tolerance for Female Genital Mutilation, Sanny Taïbatou begins her rounds in the Ladjifarani neighbourhood. The young woman, in her thirties, knocks on doors, sits with mothers, talks through vaccination schedules and preventable diseases, and then broadens the discussion to cultural practices that continue to endanger girls’ health.
She carries within her the wound inflicted by her grandmother. Excision marked her childhood. She also carries the memories of the illnesses that claimed the lives of children in her generation.
Gradually, she understood that information alone is not enough. Resistance is rooted in powerful social norms: loyalty to ancestors, fear of exclusion, pressure linked to marriage.
“When I was little, I didn’t have access to the facilities we have today, where systems are in place to make sure no child misses their vaccinations,” she says. “Among children of my generation, many died from incomprehensible diseases. Many suffered from polio and are living with disabilities today. If we had had today’s strategies, a great deal could have been avoided.”
For Taïbatou, these two realities belong to the same story: that of children exposed to risks that can now be prevented.
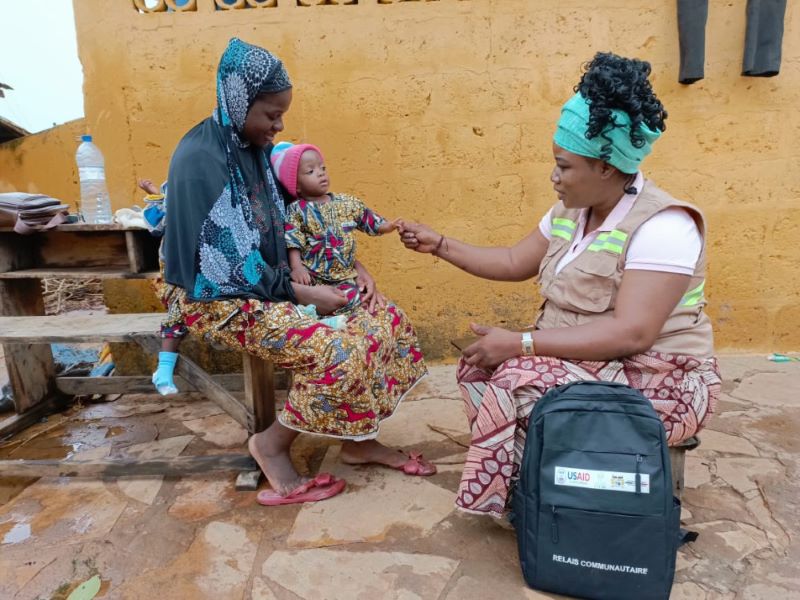
Credit: UNICEF Benin.
A contrasting context
In Benin, female genital mutilation (FGM) remains a reality, particularly in certain northern regions. According to national data, around 9% of women aged 15 to 49 have undergone FGM, while 0.2% of girls aged 0 to 14 are affected. Despite the prohibition of the practice under Law 2003-03, it persists in some communities.

Credit: UNICEF Benin
“Female genital mutilation is still widely practised in northern Benin. It affects more than one in three girls and has only declined by 10%,” notes Dr Credo Nascimento, a physician who has worked together with Taïbatou.
At the same time, childhood vaccination coverage has steadily improved. Community outreach workers move through neighbourhoods to provide information about vaccination schedules, preventable diseases and catch-up doses. But here too, uptake depends on trust and dialogue.
It is within this space that Taïbatou’s strategy takes shape.
Building on trust
Her first attempts at individual awareness-raising against excision ended in failure. She then joined the Network of Women Leaders for Development, which has been working against FGM for decades.
Gradually, she understood that information alone is not enough. Resistance is rooted in powerful social norms: loyalty to ancestors, fear of exclusion, pressure linked to marriage.
Her strategy now consists of intervening during community outreach information sessions. She begins with vaccination – a subject that is already broadly accepted – before addressing mutilation.
In the region, she even serves as a facilitator, enabling vaccination teams to reach communities that were initially hostile to immunisation. She has persuaded several women and men to join her in this struggle, which involves both regular follow-up of vaccination schedules and the fight against female genital mutilation.

Credit: UNICEF Benin
“Taïbatou is our lucky star,” says Amina Orou, who sells cowhides at Zongo market. “When my husband refuses to let me take our children for vaccination, she’s the one I call for help. She has such strong arguments that my husband gives in easily.”
Those arguments rely less on injunctions than on closeness and shared experience.
Sahana Tikandé, who sells woven cloth, explains how Taïbatou prevented her daughter’s excision. “I was excised and it was only after 20 years of marriage that I was able to have a child. I was resigned to watching my daughter go through the same ordeal. But thanks to her, we narrowly avoided the worst. On top of that, I was able to catch up on vaccinations thanks to her arguments in convincing my husband. It’s a victory I treasure deeply.”
In these conversations, the same mechanisms are at work. It is necessary to reassure, to explain, to persuade husbands, to engage grandmothers in dialogue. Excision is often presented as a protective inheritance. Vaccination likewise requires adherence to a form of prevention whose benefits are not always immediately visible.
In both cases, the task is to reshape the definition of what truly protects a girl.
Resistance and ambiguities
Originally from a Fulani camp where excision is a long-standing norm, Taïbatou is the only one among her siblings to oppose it.
Awa, a practitioner who requested anonymity, is one of those who continues to defend what she calls an “ancestral heritage”. She takes part in initiatives aimed at raising families’ awareness about vaccination, yet refuses to abandon excision.
“It is a ritual that prepares a girl for married life,” she explains. “I support all initiatives for childhood vaccination, but giving up excision feels like betrayal. I cannot betray my mother, who placed this knife in my hands.”
Have you read?
She knows Taïbatou and her struggle. “We share common battles, such as vaccination for children. Perhaps one day she will manage to convince me.”
This coexistence reveals the complexity of the field: vaccination enjoys growing support, while abandoning mutilation requires a deeper questioning of social norms.
Village chiefs largely support vaccination campaigns. On FGM, they move more cautiously. “It is not easy for us, as guardians of tradition, to stand against our customs and practices. We must move step by step,” says Tikandé M’Bo, a village chief.
The perspective of health workers
On 18 February 2026, the first day of the Muslim fast, Taïbatou organises a new session with the support of a midwife.
Nancy has worked at the district hospital for ten years. She has seen the consequences of both realities. “Before being posted here, I did not imagine the extent of the work required. I have witnessed serious situations involving children.”
“It was difficult to see children leave without being vaccinated. Today, vaccination is the first line of defence in protecting children.”
Yet she continues to receive young girls, sometimes infants, suffering from haemorrhages after excision. “The justification is still rooted in tradition. It is difficult.”
Rebecca, a nurse at the same centre, notes that some families still choose to remain at home in case of complications. “Excised girls are often treated at home. Many families do not seek professional medical care for fear of repercussions.”
Redefining protection
Across Benin, community health volunteers lead discussions on nutrition, hygiene, vaccination and family planning. In Parakou, those same spaces are now also used to question a practice that has long been presented as protective.
For Sanny Taïbatou, the link is clear. The same conversations that help a child receive a missed vaccine dose can also open space to reconsider excision.
The outcomes are not always immediate. Some families agree. Others hesitate. Resistance remains.
But in courtyards and community meetings where vaccination schedules are discussed, the definition of protection is being renegotiated, step by step, household by household.








