Q&A: How to fix the worst malnutrition crisis in more than 40 years
Climate change, COVID-19 and the Ukraine war’s impact on food prices are combining to create the worst hunger crisis in decades. VaccinesWork spoke to Simon Bishop, CEO of the Power of Nutrition, about why this matters, and what we need to do to fix it.
- 2 March 2023
- 8 min read
- by Priya Joi

Q. What are some of the key interventions you focus on?
A. Our starting point is that evidence shows that improving nutrition in the first 1,000 days of life can deliver some of the biggest benefits in development. If you get that nutrition right, you end up with children who are much more able to fulfil their potential and therefore escape the cycle of poverty. If you don’t, then you end up with so-called stunted children – children who are too short for their age and are mentally impaired. That means they learn less at school, and are 20% less productive as adults than children who were not stunted.
Global malnutrition is just not getting anywhere near the attention and resourcing that it deserves. We’re seeing the worst malnutrition crisis in more than 40 years.
Some of the best buys in nutrition and the key interventions we focus on include Vitamin A supplementation, which is for both children and pregnant women or young mothers, micronutrient supplements for pregnant women, breastfeeding counselling and treating wasted (severely malnourished) children.
Q. How did the pandemic affect hunger and malnutrition, and what did that do to the progress made in improving nutrition?
The world has made good progress over the past two decades – in the 2000s one in three children under five on the planet was stunted (too short for their age and mentally impaired) because they didn’t have the right nutrition. That figure now is closer to one in five. However, we are seeing that progress being rolled back now, and it started with COVID-19.
This is combined with the long-term impact of climate change, such as extreme drought in the Horn of Africa, which is threatening millions with hunger and malnutrition. Added to that is the impact of the conflict in Ukraine, not just in grain being stopped from coming out of the country, but through the price increases we’ve seen in food, fertiliser and fuel, which have made the production, transportation and consumption of food much more expensive.
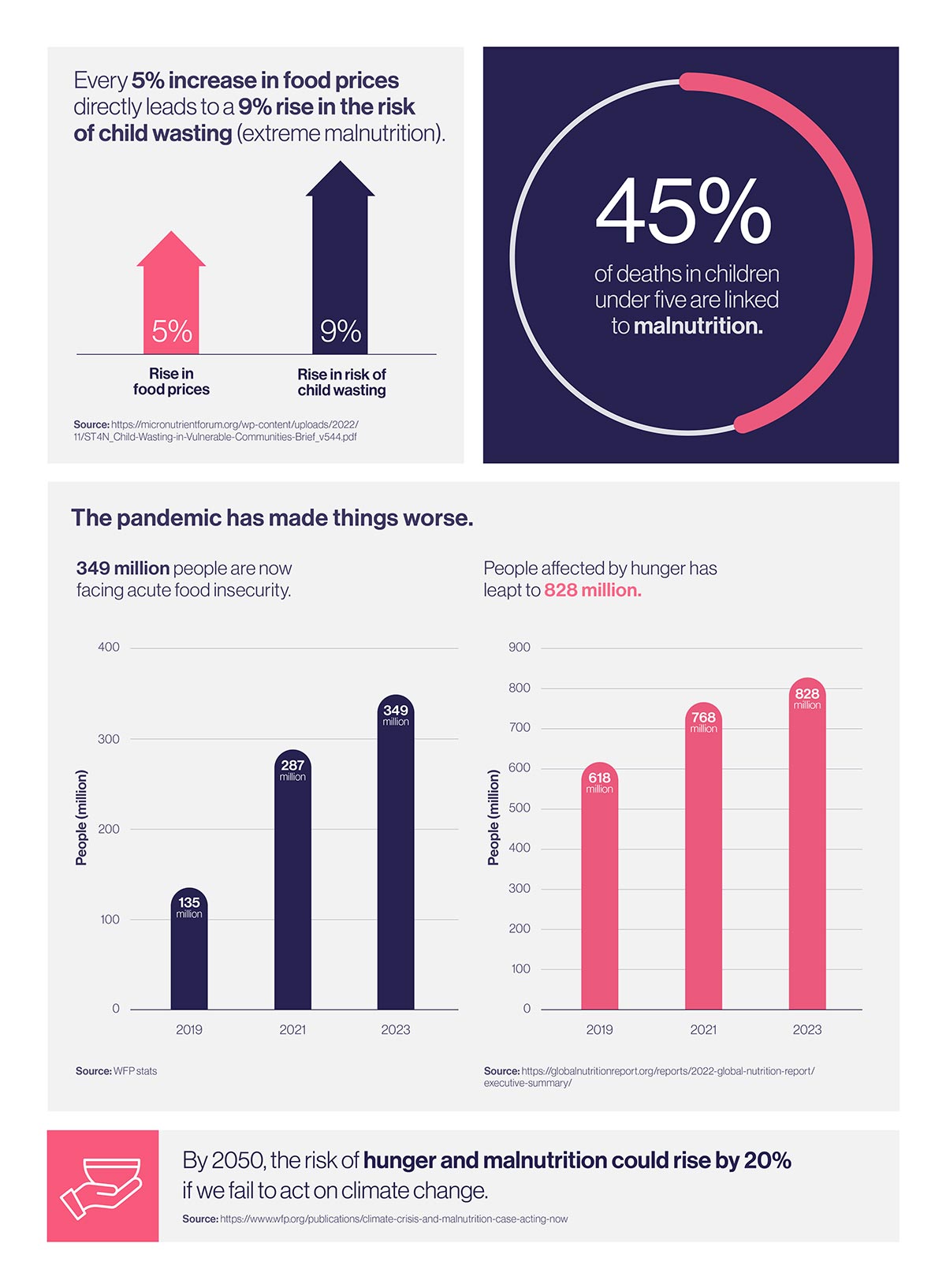
The global response to the current hunger ‘pandemic’ has been frankly woeful, and very disappointing. I recognise that the world’s bandwidth is constrained because of the conflict in Ukraine, and big natural disasters like the floods in Pakistan and the earthquake in Turkey and Syria. But global malnutrition is just not getting anywhere near the attention and resourcing that it deserves. We’re seeing the worst malnutrition crisis in more than 40 years.
There are already seven million people severely malnourished in Somalia and 27 million in Afghanistan. We know this is happening right now and yet there’s almost no attention at all.
We’re still predicting multiple famines in April/May across many parts of Africa, and probably in Yemen and Afghanistan as well. The world is on track to do what it does every time – not responding early enough and waiting until a famine is actually declared, which of course then is too late. There are already seven million people severely malnourished in Somalia and 27 million in Afghanistan. We know this is happening right now and yet there’s almost no attention at all.
Q. What is special about the way your organisation operates?
Partnerships are key to the way we work, as is country ownership. Our 22 main programmes across 16 countries are all government-owned. At the heart of our value as an organisation is that we are a convener. We bring together a range of funders and implementers, thereby crowding funding towards one big scalable programme; without us, there would be lots of separate smaller programmes that would have less impact overall.

We use our convening power (partly our reputation around doing great programmes and partly our ability to pool funds to maximise efficiency), which brings these different players together. We have funders like the Bill and Melinda Gates Foundation, Cargill, Unilever and the Rotary Fund, and on the implementation side we have partnerships with UNICEF, World Bank, World Food Program, Save the Children and so on. Bringing these partners together to deliver evidence-based interventions at scale is really how we drive transformative impact.
Have you read?
Q. Do we need more of this type of convening activity in other parts of global health and development too?
Absolutely. There could be an equivalent to The Power of Nutrition in education, for example. One of our big strategy shifts is becoming more multisectoral, so that means a programme will have health, water, sanitation and hygiene (WASH), education and food systems interventions integrated together, because we know nutrition is relevant to all of those sectors. We are moving in this direction because often we can drive more impact through multisectoral programmes, as opposed to just having a narrow health systems programme.
Q. You helped prevent 600,000 cases of stunting by the end of 2022 – a target that was met two years early. What were the key factors in reaching that goal, and reaching it ahead of target?
We hit this target early because of two related things. One is our convening power and the other is the smart use of grants to leverage other types of money.
Our Ethiopia programme is a good example of how convening power can help. It is a US$ 30 million government-owned integrated nutrition programme, and the government put in $2 million of the $30 million. The on-ground implementation partners are UNICEF and Action Against Hunger. The funders include some of our own money from our some of our founding partners (the British Foreign Office, as it was when we started, and Children Investment Fund Foundation), but also from the Eleanor Crook Foundation, the END fund and the Rotary Foundation. This shows how we bring these different partners together.
The second factor is the smart use of grants. So with our Madagascar programme, the government were going to take out a $14 million loan from the World Bank for nutrition programming. We offered a $10 million grant with the condition that the grant would double the size of the loan. The programme ended up being $90 million.
Zero-dose children who never get a single vaccine tend to be from the poorest and most marginalised communities, and they are the same communities that don’t get the right nutrition either.
We now have eight programmes with the World Bank totalling $410 million, and in six of them we’ve proven that us bringing grants to the table has incentivised the governments to allocate more of their international development assistance to nutrition. And we’re now partnering with the Islamic Development Bank to try and replicate that. This could happen with the African Development Bank as well.
Q. Gavi’s first-ever partnership involving nutrition in disease prevention has been with The Power of Nutrition and Unilever. How well joined up have programmes been so far?
Programmes have not been integrated anywhere near enough. Both sectors are trying to help the same vulnerable children. Zero-dose children who never get a single vaccine tend to be from the poorest and most marginalised communities, and they are the same communities that don’t get the right nutrition either. The silos between nutrition and immunisation are similar between the Water, Sanitation and Hygiene (WASH) and the education sectors.
It’s a scandal. Only one in five kids who are severely malnourished and on the edge of dying get the treatment they need.
The programme with Gavi in Indonesia is aiming to help one million children by integrating handwashing, nutrition and immunisation. We’ve got increasing evidence to show that integrating these interventions is a smart use of money as well as a good return on investments. In Indonesia, stunting affects nearly a quarter of children under five years. Around a quarter of deaths in children under one year in Indonesia is attributable to diarrhoea.
How combining immunisation, handwashing and nutrition could help fight disease

A new partnership aims to improve the lives of Indonesian children through an integrated approach to health.
The Indonesian government has done a great job stepping up on nutrition with a significant increase in attention on it. So it’s good place to try out a partnership like this. Next, we’d like to come up with a multi-country African partnership.
Q. If there was one thing that you could think of right now, that would make a huge difference to your work, whether that’s more partnerships or more government buy in or more funding, what would it be?
At the risk of being overly simplistic, it’s money. Over the last 40 years, only about 1% of traditional grant aid has been allocated towards nutrition despite everyone recognising that it’s foundational to all of the Global Goals. There are incredibly effective interventions with vitamin A and micronutrient supplements, breastfeeding counselling and treatment for wasting , and only around one in five of those in need get them.
I mean, it’s a scandal. Only one in five wasted kids, who are severely malnourished and on the edge of dying, get the treatment they need. This is happening across Somalia and other parts of the Horn of Africa, Yemen, Afghanistan and elsewhere. These are not expensive interventions, so it is obviously much more than the money. We try to be super-efficient by delivering cost-effective nutrition with the money we raise, and leveraging grants to enable countries to borrow money. But ultimately, we just don’t have enough money and that’s just a tragedy.







