Transforming tuberculosis treatment in Sri Lanka
Shifting from a paper-based system to an electronic one has made navigating tuberculosis treatment easier for both healthcare workers and patients.
- 13 December 2022
- 4 min read
- by Aanya Wipulasena

It is a sunny afternoon in Colombo. Sixty-two-year-old W L Nandasena is at the Chest Clinic to do his monthly tuberculosis check-up and take a course of medication for the next month.
A quick search on her work computer shows Dr Gawrie de Silva, the additional District Tuberculosis Control Officer at the clinic, that Nandasena has received his medication from the pharmacy, and is up to date with his treatment.

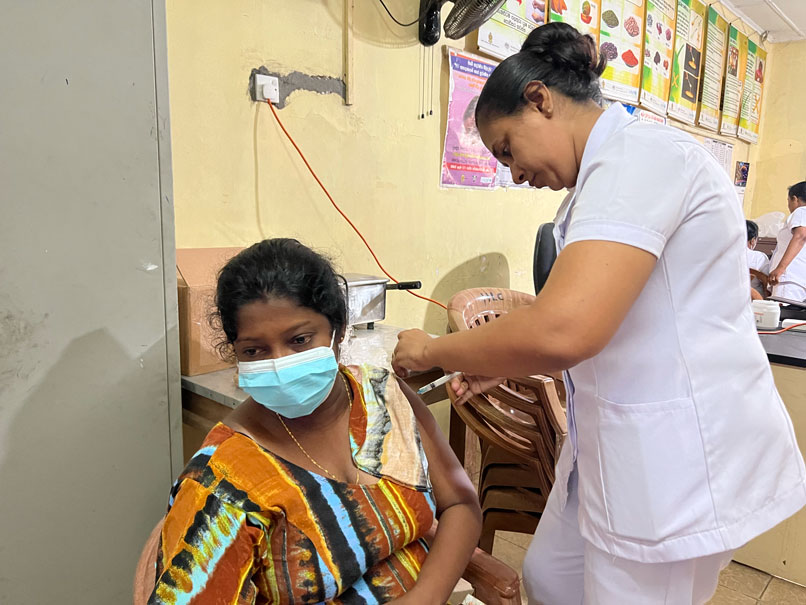
Credit: Aanya Wipulasena
“During the COVID-19 travel restrictions this system [ePIMS] was extremely helpful. We were able to track patients who were undergoing treatment and post or deliver their medication to their homes because they couldn’t go to clinics.”
"This system makes it very easy to see the history of a patient. See here, this shows if he is doing well with the treatment," Dr Silva says, pointing at the monitor of her computer.
Sri Lanka introduced the electronic Patient Information Management System for Tuberculosis (ePIMS) several years ago in a bid to streamline data to ensure better healthcare and gradually mitigate the spread of tuberculosis.
Dr Silva says that the ePIMS was successfully implemented in 2019, and now Chest Clinics from all around the country feed information about patients into the system every day.

Credit: Aanya Wipulasena
"We have information about a patient from the day he or she is diagnosed till the completion of six months-long treatment. The best part about the electronic system is that we can see the whole story of a patient [in a few clicks])," Dr Silva says.
Prior to the ePIMS, the tuberculosis care system was entirely paper-based. This meant healthcare officers had to go through large files to learn the history of a patient and rummage through piles and piles of paperwork to calculate the number of tuberculosis patients recorded in each clinic to formulate the island-wide cases for each year. This was easier said than done.
Under the new system, after a patient is registered, tuberculosis-related healthcare givers update his or her record at each point of treatment, including the lab where the tests are conducted, and the pharmacy where the medication is issued. The system also indicates if the patient's close contacts were traced and tested.
Have you read?
For patients like Nandasena, it means that he will not miss his vital course of treatment.
"If I fail to show up on a clinic day, an officer at the hospital calls me on my mobile phone asking to come to get my medicine. Because of that, I put in the extra effort to get my medication on time," he says.
Nandasena was diagnosed with tuberculosis in June 2022. Contact tracing found that his daughter had the disease as well. She is also a registered patient at the Colombo Chest Clinic.

Credit: Aanya Wipulasena
Some tuberculosis patients tend to stop treatment when their symptoms subside, assuming they are cured. Health workers such as Dr Silva constantly check the system to make sure no patient is left behind. The ePIMS helps to keep tabs on all patients.
"During the COVID-19 travel restrictions this system [ePIMS] was extremely helpful. We were able to track patients who were undergoing treatment and post or deliver their medication to their homes because they couldn't go to clinics," Dr Silva adds.
Statistics from the National Programme for Tuberculosis Control & Chest Diseases (NPTCCD) show that, in 2021, Sri Lanka had more than 6,500 tuberculosis cases, while in 2020 the number of cases was over 7,000. In 2019 the country recorded nearly 8,500 cases.
Checking on her computer, Dr Silva points out that the Colombo district has thus far recorded (end of November 2022) more than 2,000 cases, which is 25% of the total cases recorded island-wide.
Dr Mizaya Cader, team lead of the Planning, Monitoring, and Evaluation Unit at the NPTCCD, says that she conducted a study and found that before the ePIMS was introduced it could take weeks to register a new patient, start treatment and conduct contact tracing.
"With this real-time data sharing, our healthcare system is much more efficient now," she says.
However, getting used to the new system has not been a walk in the park for many healthcare workers. "Our main challenge is motivating people to move from paper-based work to the electronic system. Not everyone is tech-savvy," she explains.
The NPTCCD is continuously conducting training for healthcare workers to encourage them to use the system.
The shortage of infrastructure facilities in Sri Lanka is another hurdle the NPTCCD has to navigate. Some clinics don't have enough computers and some struggle with internet connectivity. Despite these challenges, Dr Cader is hopeful that the system will be used to its best potential in the near future as it is also extremely systematic and less time-consuming.
Nandasena, who got his check-up done and received the medication, is leaving the clinic.
"I didn't have to stay for hours to get my treatment at the clinic. The service is very beneficial to people like me," he says.