The ‘black fungus’ epidemic hitting COVID-19 patients in India
Amid the 28.4 million cases and over 300 thousand deaths from SARS-CoV-2, a second epidemic has hit India. ‘Black fungus’, clinically known as mucormycosis, is an infection currently affecting nearly 12,000 immunocompromised patients recovering from COVID-19. But what is this infection and what does it mean for health systems?
- 9 June 2021
- 3 min read
- by Gavi Staff
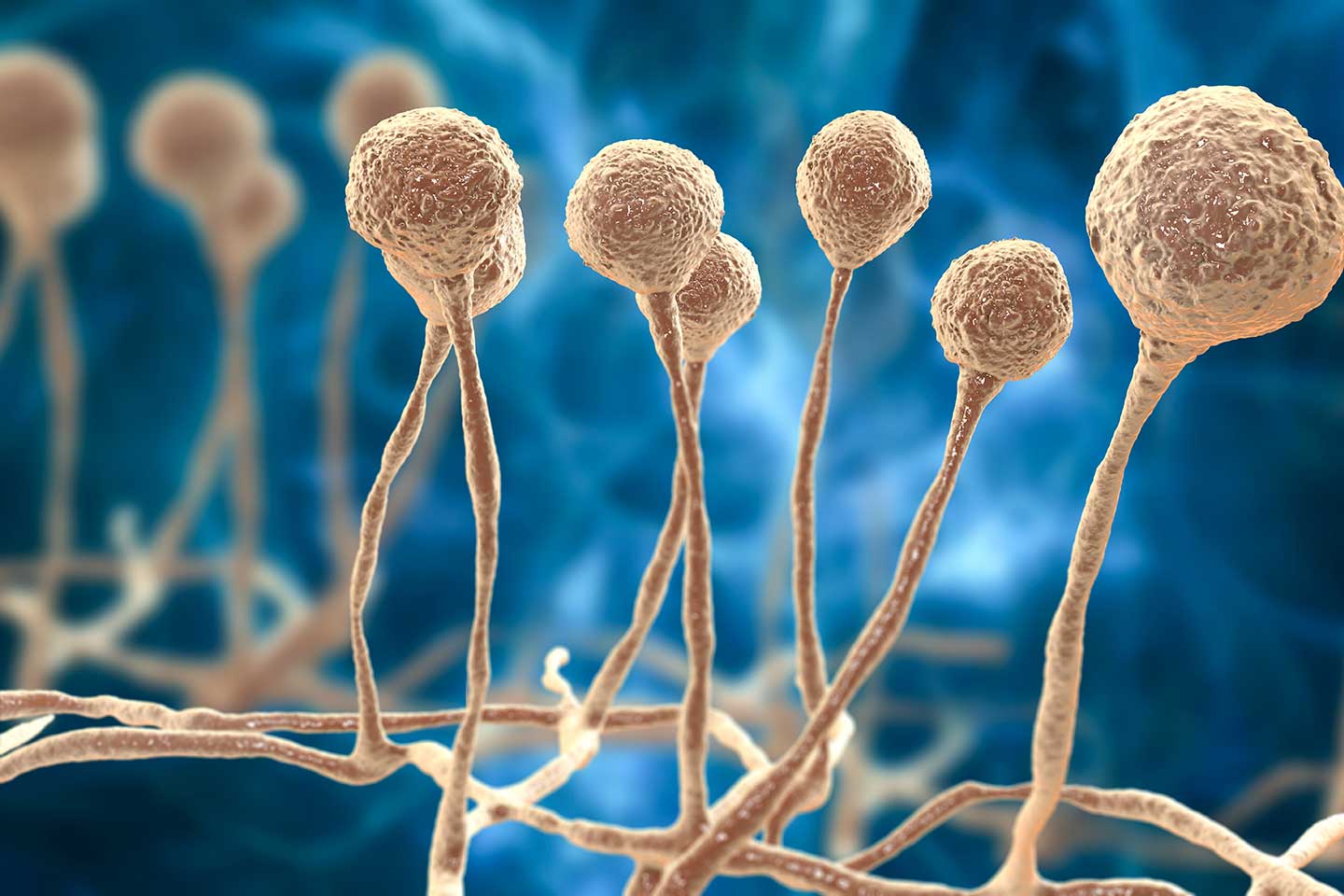
The COVID-19 wave currently ravaging India is leaving millions of recovering patients with compromised immune systems in its wake. One particularly brutal fungus – mucormycosis – is taking advantage.
The disease is an infection caused by fungi, which are spread through the inhalation of spores from the surrounding area, such as in soil or vegetation. They can also be transmitted intravenously during drug use or in a hospital setting following surgery. The infection is angioinvasive, meaning the pathogen colonises blood vessels, which can result in thrombosis (blood clots) and tissue necrosis (death of tissues).
While the infection can be extremely brutal, the fungus is only able to survive in patients with weakened immune systems.
This leads to loss of oxygen supply and accounts for the high case fatality rate – up to 50% in some regions. It is often characterised by a swollen, bulging eye, suggesting that the infection has spread to the central nervous system (CSN) through the nose or mouth. Many patients can only be saved through invasive surgeries to physically remove the eye or nasal cavity; however if caught early it can also be treated with antifungal medications such as amphotericin B.
While the infection can be extremely brutal, the fungus is only able to survive in patients with weakened immune systems, particularly those with diabetes mellitus or, as is happening now, patients taking immunosuppressant steroids to reduce their likelihood of dying from COVID-19. The suppression of the immune system from such drugs wears off after a patient stops receiving them, but until that happens they increase patients’ susceptibility to infection. The steroid dexamethasone has been shown to significantly decrease deaths among patients with severe COVID-19, but this benefit comes with a trade-off. This has made India particularly susceptible to the infection as rates of COVID-19 have increased drastically in the second wave and the healthcare system have become flooded with patients.
Have you read?
Even before the SARS-CoV-2 pandemic, India had already reported prevalence of mucormycosis at around 0.14 cases per 1000 within the population, compared to 1.7 per million in many high-income countries. These rates are linked to the occurrence of diabetes mellitus in India, in which cases are poorly controlled with medication or underdiagnosed due to lack of access to health services.
India is not the only country with an increase in mucormycosis cases. Pakistan, Nepal and Bangladesh have been reporting COVID-19-associated mucormycosis; however, these countries are not as highly populated and have not been affected by a wave of COVID-19 cases in the same way. Despite this, under 15% of people in these countries have received their first dose of vaccine, meaning that there is potential for similar mucormycosis epidemics to occur across other low- and middle-income countries. This would put a high burden on healthcare services which are already struggling from the pandemic. Therefore, it is vital to ensure vaccine equity across the world to protect healthcare systems and patients from COVID-19, as well as other associated, deadly, infections.









