Do kids get long COVID? And how often? A paediatrician looks at the data
Children can get long COVID, but it seems to be less common than in adults. And they tend to recover quicker.
- 30 August 2021
- 6 min read
- by The Conversation
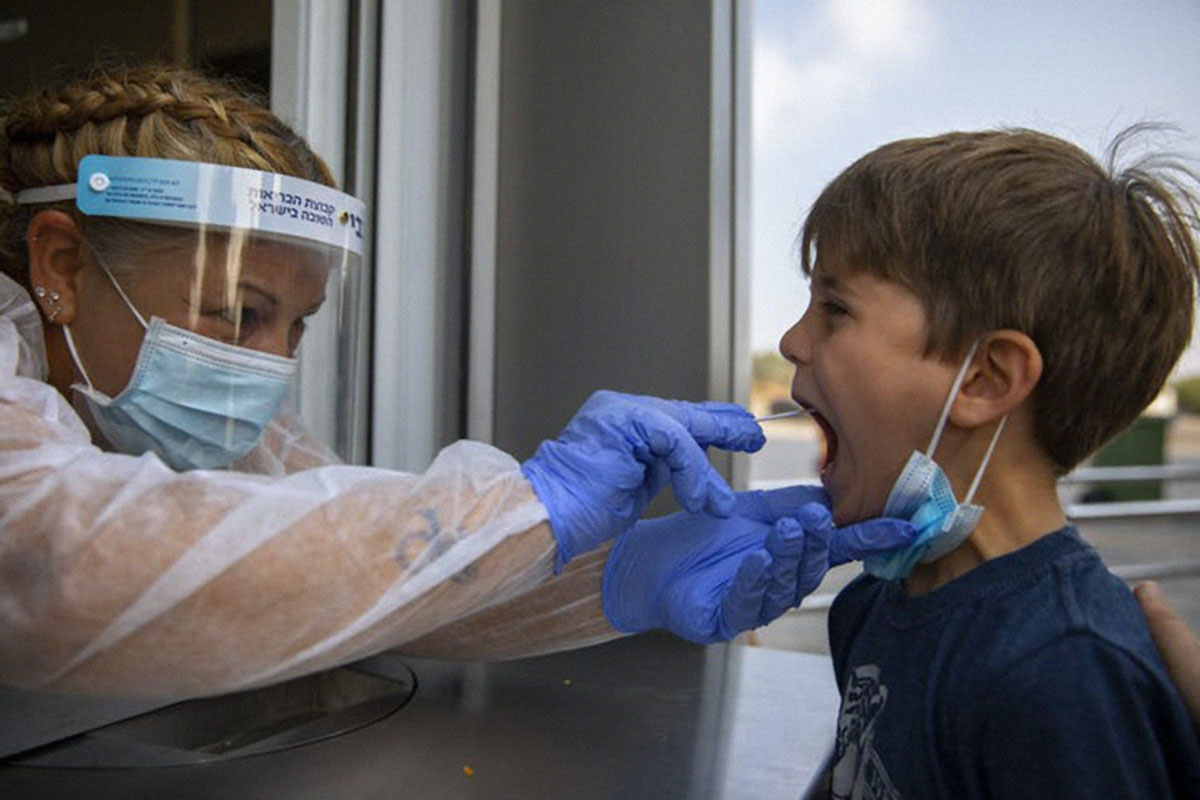
Since the rise of the more infectious Delta variant, we’ve seen reports of more cases in children than with previous strains of the virus.
Many parents are becoming more concerned about COVID in kids. One question many are asking is whether kids can get “long COVID”, too, where symptoms persist for months after the initial phase of the illness.
I’m a paediatrician and infectious diseases expert, who cares for children with COVID-19, and have been following the research in this area.
Children can get long COVID, but it seems to be less common than in adults. And they tend to recover quicker. Let’s go through the data.
What is long COVID?
There’s still no standard definition of long COVID, and the syndrome itself is quite variable.
Even though there’s no one form of it, three broad types of symptoms frequently occur:
-
cognitive effects, such as slowed thinking or “brain fog”
-
physical symptoms, including fatigue, breathlessness and pain
-
mental health symptoms, such as altered mood and anxiety.
Having symptoms that persist for more than 28-30 days following the onset of COVID is increasingly being labelled as long COVID in the medical literature.
The cumulative effect of long COVID symptoms can have a profound impact on sufferers’ ability to function in their daily life, work or schooling.
Does it occur in children?
Long COVID probably does occur in children but it is likely less common than in adults.
Two Australian studies are useful here. In one study of adults and children, researchers found 20% of over 2,000 COVID cases in New South Wales had persistent symptoms at 30 days. By 90 days, this had reduced to 5%. The youngest age group (0-29 years) were more likely to recover quicker than older age groups.
In a study from Victoria that looked at children only, 8% of 151 children with mostly mild infections had some persistent symptoms for up to eight weeks. However, all had fully recovered by 3-6 months.
In these children, the number of symptoms at 28 days was fewer compared to that in the first week of their illness.
The study found 1.8% of children has symptoms at day 56. Headache, fatigue and loss of smell were the main issues.
Three-quarters of the children with persistent symptoms went on to report a full recovery. However, a quarter were not followed up, so it was unclear how many among this small group may have had longer-term problems.
The same study observed children who had other viral illnesses, not COVID. It found 0.9% showed persistent symptoms at 28 days. This suggests a “background rate” of non-specific symptoms like headache and fatigue occurs in children, which is important to consider — although the rate in children following COVID was considerably greater.
Have you read?
Some studies of COVID in children, for example, from Italy and Russia, have found persistent symptoms to be more common.
But these studies looked at variable populations, such as only those who were hospitalised or had moderate to severe illness, or collected data retrospectively.
Also, the children were infected during the first wave of COVID in Europe and the overall societal impacts may have contributed to some of the ongoing problems reported in children, like fatigue and insomnia.
This variability between studies makes it hard to compare them to work out the real rate of long COVID in children. Taken together, there seems to be a relative increase of persistent symptoms in teenagers compared with younger children.
What about Delta?
These studies were done before the effects of new variants of concern, most notably Delta, which has shown an increase in the number of COVID infections in children.
Delta might be leading to increased severity of COVID in adults. But there’s no compelling evidence yet that Delta is more severe in children.
Current admission rates in the 2021 Delta outbreak in NSW are no greater than those in children across Australia during 2020.
Both adults and potentially children who get more severe COVID in the initial (“acute”) stage of their illness seem to be at increased risk of long COVID. But if Delta isn’t causing more severe illness in kids, it’s reasonable to expect Delta won’t increase the risk of long COVID in children either.
Scientists need to agree on a consensus definition of long COVID, and a standardised way to measure it.
Given the non-specific nature of many long COVID symptoms, research also needs to include a control group of kids who haven’t had COVID to really determine the COVID effect.
Do persistent symptoms occur following other viral infections?
Yes. Common examples include the glandular fever virus, also known as Epstein Barr virus, and Ross River fever virus.
Studies report up to 10-15% of children and adults with these infections report chronic symptoms including fatigue, pain, slowed thinking and altered mood.
What actually causes persistent symptoms following viral infections, including COVID, remains a major focus of researchers. Persisting infection itself is not likely.
Major theories include chronic inflammation, blood flow disturbances or nervous system damage.
What should I do if my child has had COVID?
Some children do have persisting cough and fatigue around the four-week mark.
Parents are understandably concerned, but should be reassured most children will fully recover. If there’s a pattern of improvement, that’s a reassuring sign.
If symptoms continue beyond four weeks, it’s sensible to stay in touch with your GP or paediatrician.
In terms of persistent symptoms following other infections, we do know what helps to promote recovery. Things to consider are:
-
aiming to have your child gradually return to normal activities
-
where fatigue is an issue, use rest well, in short periods and after doing activities.
Returning to normal activities may require planning, including liaising with teachers around school return, which is especially important in the context of online learning.
Aim for incremental gains, remain optimistic about recovery, and always seek help if you’re not sure what to do.![]()
Authors
Philip Britton, Senior lecturer, Child and Adolescent Health, University of Sydney

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Philip Britton receives funding from the National Health and Medical Research Council, the Commonwealth Department of Health and NSW Ministry of Health.
Partners

University of Sydney provides funding as a member of The Conversation AU.








