How solar is powering maternal care and immunisation in rural Uganda
In rural Uganda a lack of reliable power means mothers are often forced to give birth in the dark. Now a new solarisation project is bringing light and reliable electricity to health centres across the country.
- 16 March 2026
- 8 min read
- by John Musenze

At a glance
- Like many health centres in Uganda, Nakifuma Health Centre III struggled with an unreliable power supply. “Power was more off than on,” a clinical officer said. That meant vaccines needed to be kept at a different facility in order to prevent risky temperature fluctuations, and mothers often gave birth in the dark.
- That changed in December, when a 12-kilowatt solar power system was installed at Nakifuma. Nurses applaud the better working conditions, and more births and vaccinations are being reported by the facility.
- Nakifuma Health Centre III is one of 250 facilities in Uganda to benefit from the Gavi-backed solar power project.
At exactly 17:44 on 26 February, under steady electric light, Esther Nalubega, 33, delivered a healthy baby boy at Nakifuma Health Centre III in Mukono District. His first cry echoed through a maternity ward that, for once, was not threatened by darkness.
Doctors asked her to stay three days for observation. She agreed without hesitation, something she had never done before. Unlike before, when mothers often opted to leave a few hours after delivery against medical advice, Nalubega felt comfortable with the doctors’ counsel.
“My first two children were born here. With my first baby, the power went off. With the second, we were told it had been deliberately switched off to save units. I asked to be discharged quickly because I was not comfortable staying in darkness,” Nalubega told VaccinesWork, while sleeping next to her newborn.
Credit: John Musenze
This time, she passed three peaceful days at the facility. She slept with the lights on. She watched television in the ward. Though she had no caretaker by her side, still she felt secure.
“It feels different now; I feel like I am home. You don’t fear the night,” she said.
From vaccine recipient to area supply hub
Nalubega is among the 120 mothers delivering at Nakifuma Centre III, Mukono district, each month. The same centre sees more than 300 children receive their vaccinations each week, according to Dr Mastula Namagembe, a clinical officer.

Credit: John Musenze
In other words, the health centre is busy around the clock. But before the installation of the 12-kilowatt solar system at the facility in December 2025, the facility was depending on the national power grid, which was unstable.
“Power was more off than on. The biggest departments affected were maternity and laboratory because all these depend on electricity. We used to keep our vaccines at Nagalama hospital and would pick what to use in the morning. Mothers were required to have a torch prepared in case,” Namagembe explained.
Since January and the new power source’s installation, the facility is now supplying vaccines to the neighbouring smaller facilities, especially private clinics approved to offer vaccination. The facility, which used to schedule vaccination sessions twice a week, is now offering immunisation four days weekly.
Keeping vaccines cool is vital. But is it enough?
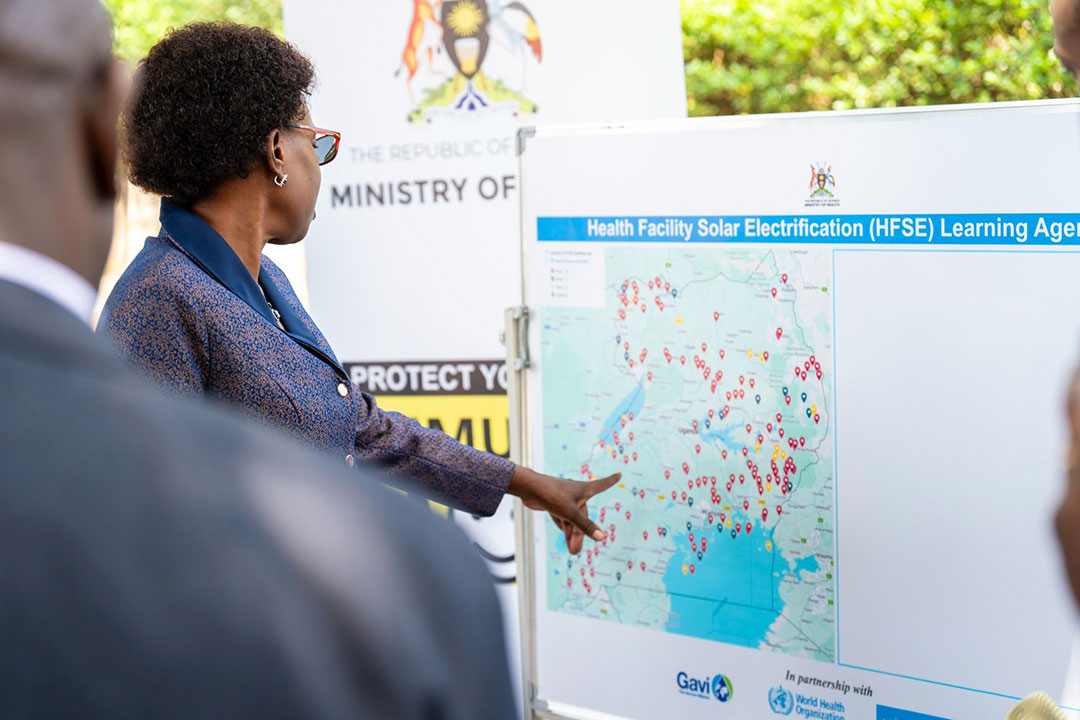
Nakifuma Health Centre III is one of 250 rural facilities benefiting from Uganda’s Health Facility Solar Electrification (HFSE) initiative, implemented by the Ministry of Health with support from Gavi, the Vaccine Alliance, UNICEF and the World Health Organization. The project aims to address one of the most persistent barriers in Uganda’s health system: unreliable electricity.
Jimmy Ameny, the grants coordinator for Gavi at Uganda’s Ministry of Health, said the shift from powering refrigerators alone to electrifying entire facilities followed a 2022 visit to Busi Island in Wakiso District with Gavi’s then-CEO, Dr Seth Berkley. Vaccines were safely stored, but a mother was delivering by lantern in a dark ward at 15:00.
Have you read?
“Wakiso is an urban district, so we wondered what happens in hard-to-reach districts. We realised that protecting vaccines alone without ensuring safe childbirth was incomplete. The child must first be born safely,” Ameny told VaccinesWork.

Credit: John Musenze
Ameny noted that under the pilot phase of the project, implementation stands at roughly 53% completion. Priority was given to high-volume, hard-to-reach facilities without stable grid power. Solar systems now support maternity wards, laboratories, outpatient departments and staff quarters, which was an important factor in retaining health workers in remote postings.
First launched in Zambia, the HFSE initiative secured around US$ 29 million in funding to instal 3–30 kWp solar photovoltaic systems and cold chain equipment (CCE) in 1,277 health facilities across Zambia, Ethiopia, Pakistan, and Uganda, and the majority of installations are projected to be fully implemented by the end of June 2026.
Healthcare in the dark
According to the Health Ministry, nearly 50% of the health facilities in Uganda do not have reliable electricity, with that tally including about 6,000 rural Health Centre IIs and IIIs – the backbone of rural primary care and the logistical linchpin for delivering care to hard-to-reach areas.
These health centres either have no grid connection or depend on generators that require fuel. Often, districts cannot afford that fuel, meaning they go without electricity. That, in turn, means that maternity wards run in the dark, laboratories shut down and vaccine refrigerators fail.
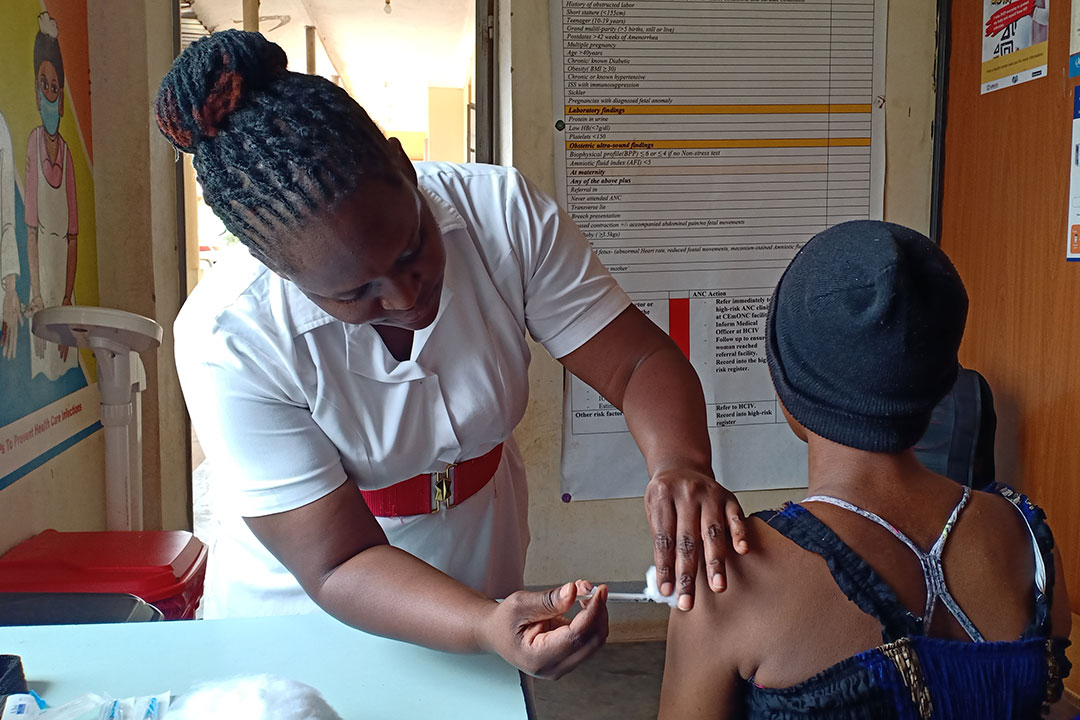
Credit: John Musenze
The knock-on effects of that are grave, and account for at least a portion of Uganda’s maternal and child mortality statistics.
According to the 2022 Uganda Demographic and Health Survey – the most recent published – maternal mortality ratio stands at 189 deaths per 100,000 live births. While multiple factors contributed to this this burden, health experts say unreliable electricity compounds risks pre- and postnatal deliveries and emergency obstetric care.
Children are also left at risk by the ways that unreliable electricity supply impacts immunisation. Much as Uganda’s immunisation coverage is above 90% for key antigens such as DTP3 and the first dose of measles-rubella, by both Ministry of Health and WHO estimates, coverage disparities remain in remote districts. A study by researchers at Makerere University found that only about 24% of all facilities achieved adequate vaccine cold chain management standards, exposing doses to potential temperature excursions and wastage.
Midwives unencumbered
But at Nakifuma Health Centre III, the installation of the solar grid has seemed to tackle these challenges by root and branch. “From its installation, we have never seen power gone. We do not know if it has gone or not: it’s automatic power-on solar, so there’s no disruption, not even for a second,” Dr Namagembe highlighted.
Betty Nakazibwe, a midwife who has worked at the facility for a year now, said she had previously found it hard to do her job.
“As a midwife, you use your hands to help a mother giving birth, but on many days, we were forced to use torches and phone-lights. In most cases, a mother could tear and require stitching, but you can’t do this using a torch, even when someone is holding it for you. That is no longer the case. We have a baby warmer which uses power, so whenever power was off, it was no use and now our warmer uses solar,” she told VaccinesWork.
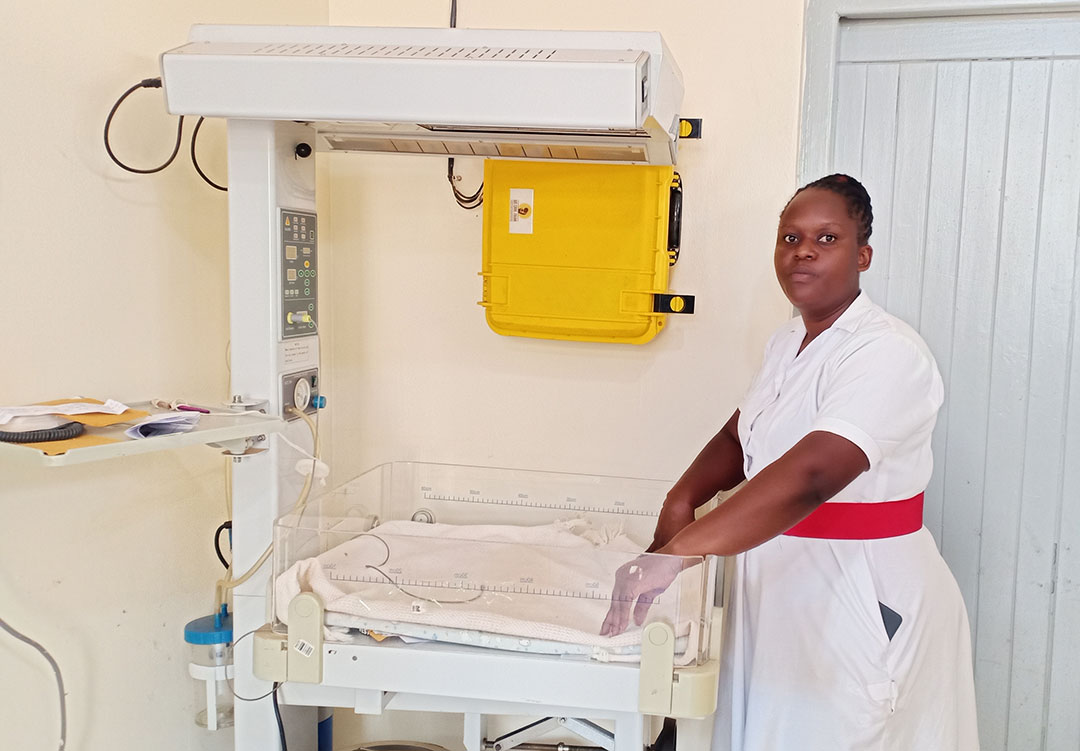
Credit: John Musenze
Nakazibwe highlighted that since vaccines were not kept within the facility, but at another facility 10 km away, it was hard for her do her job reliably, and in a timely manner.
“As a midwife, I want to thank Gavi for this: there’s nothing as good as working in a good working environment. In my staff unit, I now use the electricity to even watch TV, unlike last year. You work on a mother at night when you are comfortable. I am able to help 24/7 mothers; time is no longer against me because the facility is 24 hours light.”
More mothers, more care
In Omoro district, northern Uganda, Acet Health Centre III is another facility that has been lit up by solar power since December 2025.
Before that, Acet Health Centre III stored vaccines at another facility, which meant immunisation sessions were limited to twice a week and the facility majorly operated during the day for just about 12 hours. Today, the facility works 24/7 and staff are always available to assist anyone at any time of arrival.
“Sometimes our power units would run out when we had no funds to reload immediately, and services would be disrupted because most of our equipment depends on electricity. We at times take days or weeks without power but the laboratory microscope runs steadily, the maternity wing is brightly lit and vaccine refrigerators maintain constant temperatures around the clock,” said Dr Justin Ojok, the senior clinical officer in charge of the facility.
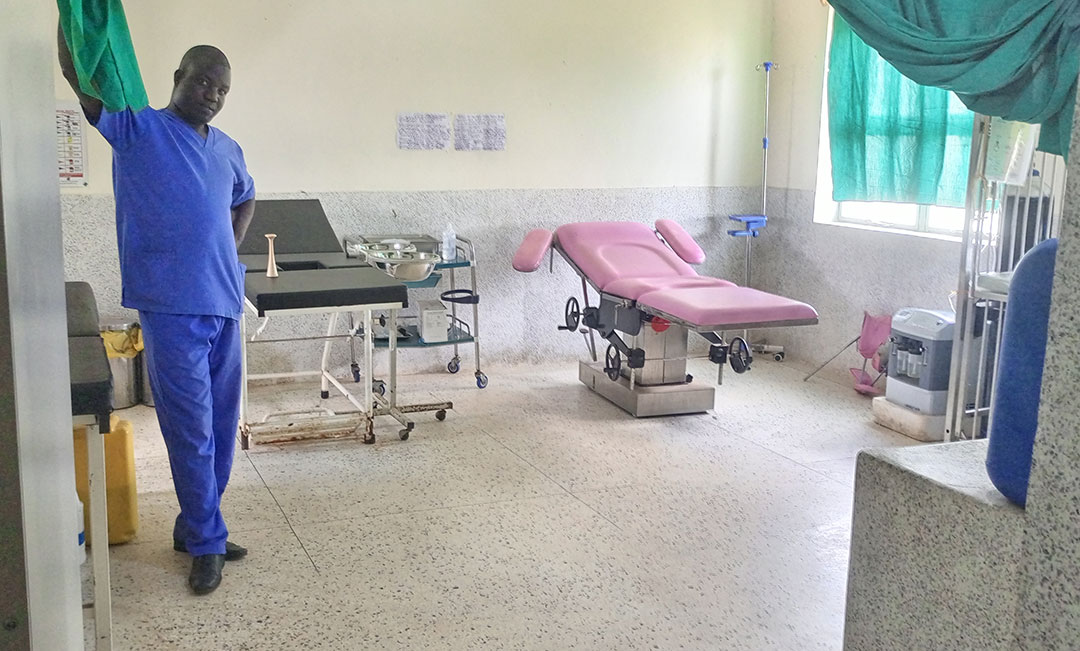
Credit: John Musenze
Dr Ojok reported that since solarisation, the facility has seen an increase in mothers coming in for maternal services, from about 24 a month, to about 62 a month. The facility has also become a storage point for neighbouring centres such as Binya HCII and Odek HCIII, which face ongoing electricity challenges.
Dr Ojok said that with reliable electricity, the hospital is planning to digitise patient records, which he expects will improve efficiency.
Darkness cost lives
The change is not just a relief but a life-saver, according to Sarah Akot Auma, a midwife at Acet Health Centre III. “I recall one day we had no electricity, and a mother decided to go to another facility, which is very far from us. Unfortunately, the baby had gotten tired and was born dead upon arrival,” she said. “Many mothers in the neighbourhood would rather give birth from home than come here in darkness. We could use our torches and phones to save lives because even during the day, the rooms are a bit dark.”

Credit: John Musenze
Light is vital, but Auma noted that the solar system also powers other critical tools that find daily use: sterilisation equipment, a blood pressure machine used to detect pregnancy complications early, and an oxygen concentrator that supports newborns with breathing difficulties before referral.
Boosting deliveries and daily immunisation
Like other facilities, Acet received a solar system powering its maternity ward, laboratory, vaccine refrigerator and parts of staff housing through the HFSE initiative.
Each facility included in the scheme also receives a WHO-prequalified vaccine refrigerator designed to maintain temperatures between 2°C and 8°C, the required range for most routine vaccines. Health workers at each centre have been trained in basic maintenance, including panel cleaning and system monitoring.
Immunisation services have expanded to daily sessions, with 483 children receiving routine vaccines over January and February, including HPV doses for adolescent girls. Moreover, no vaccines have needed to be discarded due to vaccine vial monitor alerts of temperature-linked spoilage.








