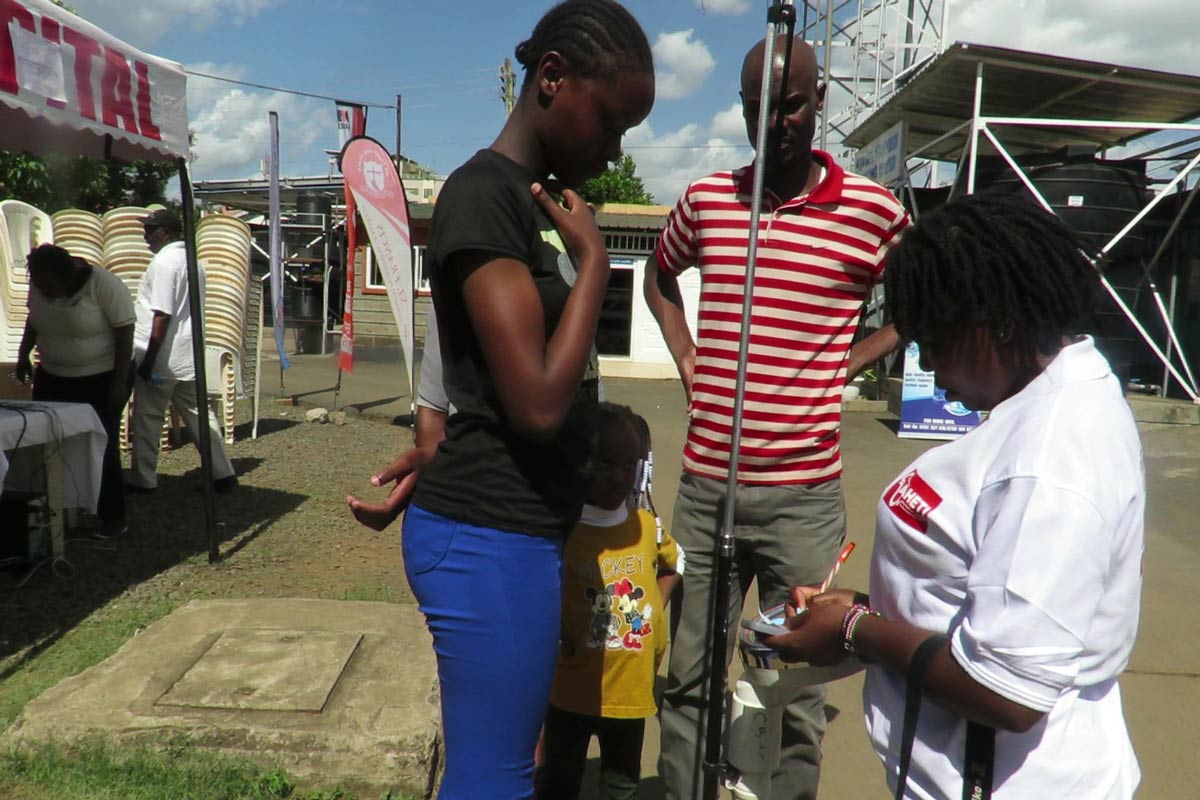On Kenya’s borders, the Ministry of Health works with truck drivers and sex workers to fight mpox
Both jobs can be socially isolating and physically exposed – an unsalutary combination amid a viral epidemic.
- 20 March 2026
- 6 min read
- by Pauline Achieng Tom

At a glance
- During the mpox surge of recent years, major transport corridors criss-crossing sub-Saharan Africa have also become avenues for viral spread.
- Border checkpoints have become vital nodes for disease control. “Our work can be very isolating and makes it hard to hear news. We only get human interactions at these stops,” said long-haul trucker Hamadi.
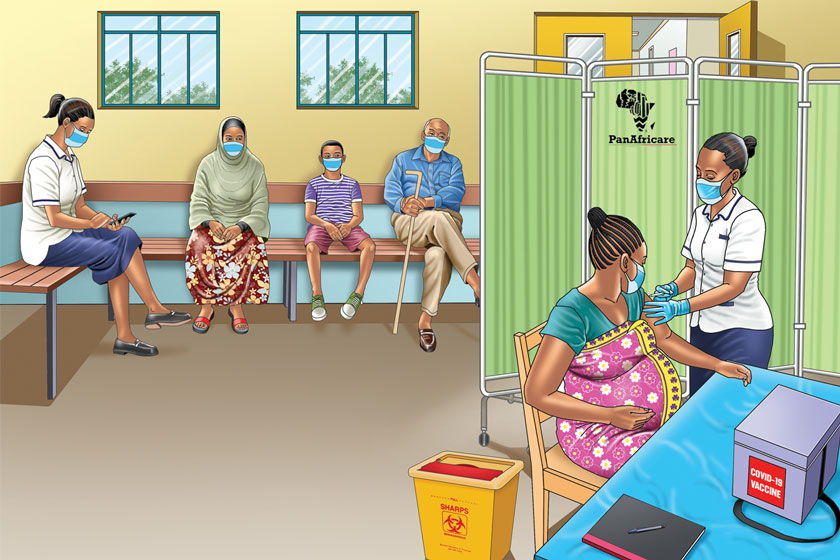
- Truck drivers and sex workers are two groups at particular risk. Along with frontline health workers, they were prioritised for vaccination during a late-2025 campaign focussed on Kenyan transport hubs.
At the Namanga border between Kenya and Tanzania, rows of trucks line the roads, engines grumbling as they inch towards the checkpoint. The sun is scorching. Many drivers have stripped off their shirts.
Security clearance comes first, followed by a mandatory stop at the Port Health Authority desk for screening. A flush of posters announce a disease of urgent concern for the wardens of the crossing: mpox. Up by the counter, a banner detailing the virus’s modes of transmission, symptoms and prevention measures hangs next to a mounted hand sanitiser dispenser.
Among the drivers seeking clearance is long-distance trucker Ibrahim Hamadi, who has driven through more than 14 countries in sub-Saharan Africa and is on his way back from a trip to the Democratic Republic of the Congo (DRC), one of the countries hardest-hit by mpox.
Mpox, previously known as monkeypox, is a viral disease characterised by painful rashes, swollen lymph nodes and fever, which usually surface within two weeks after exposure. While most people recover, it can lead to death. The disease can be transmitted through skin-to-skin contact, with sexual networks driving spread in many places.
The disease first broke out in the DRC in 1958, but a global resurgence since 2022 has seen unprecedented numbers of people suffer the illness, and led both the World Health Organization (WHO) and the Africa Centres for Disease Control (Africa CDC) to declare states of emergency. Africa CDC’s mpox emergency was lifted in January 2026.
Risk on the roadways
For truck driver Hamadi, awareness of the disease that had already been spreading rapidly across the continent for years, came late. “I had no idea what the mpox was. I only got to hear about it at the border in 2025. Our work can be very isolating and makes it hard to hear news. We only get human interactions at these stops.”
Truck drivers’ social isolation and extreme mobility make them a priority group for the Risk Communication and Community Engagement (RCCE) team at Kenya’s Ministry of Health (MOH).
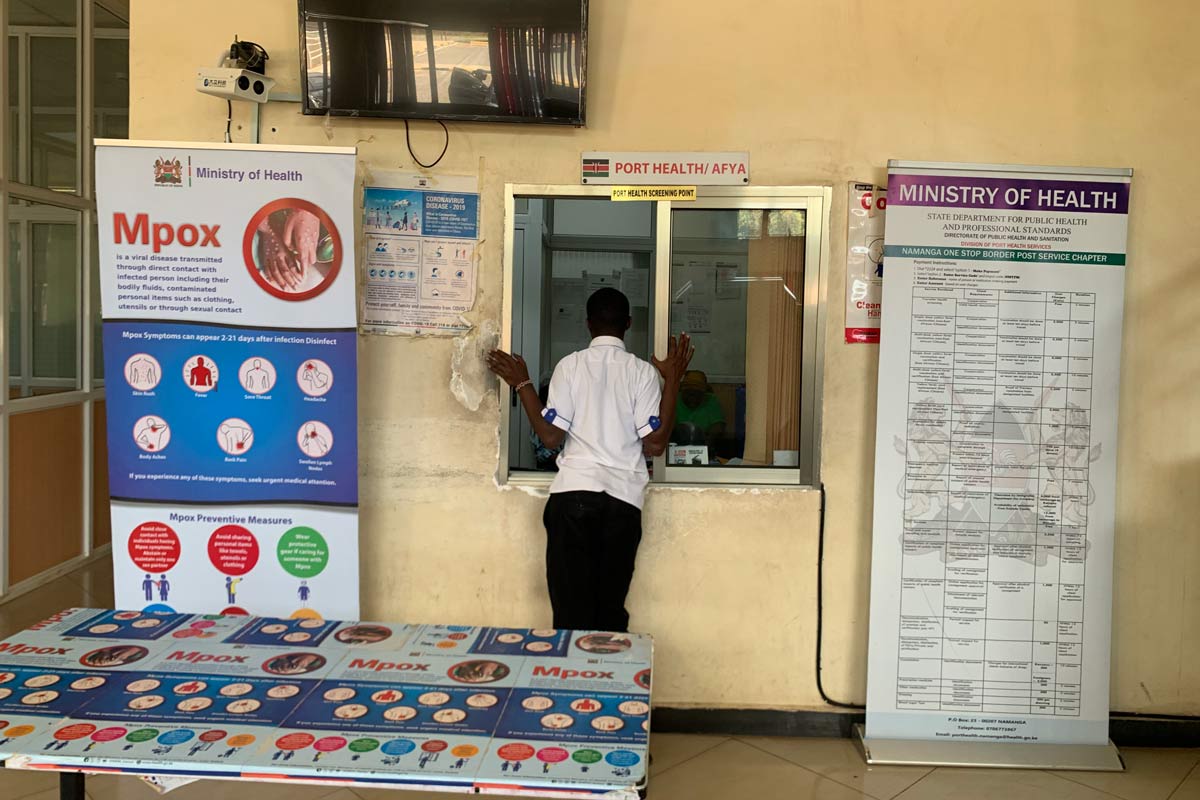
According to data from the MOH, as of March 2026 there have been a cumulative 1,065 mpox cases across 38 counties nationwide, with a case fatality rate (CFR) of 1.7% .
The ministry has screened over 8.8 million travellers at different points of entry, as early transmission was concentrated along major transport corridors linking Mombasa, Nairobi, Nakuru, Kisumu, Busia and Malaba.
In an interview with VaccinesWork, Principal Secretary in the State Department for Public Health and Professional Standards Mary Muthoni explained that epidemiological investigations grounded the Ministry’s engagement of truck drivers and sex workers.
“The initial cases were largely among truck drivers using the northern transport corridor,” she said “The second-most affected group were the sex workers who interact with truck drivers along the same routes.”
However, Elijah Nyaga, the chairperson of Long-Distance Drivers and Conductors Association, says reaching truck drivers quickly is not always easy.
“Getting real-time information to drivers can be difficult, due to their isolation and varied technological abilities and access,” Nyaga said. “When the first cases of mpox were confirmed in truck drivers, the Ministry of Health called us for meetings so we could help communicate with our members.”
Partnering up made it easier to rally truck drivers to the public health initiative even before vaccines arrived in-country.

Sex workers, another high-risk group, were also included in the outreach. For one sex worker who operates between the Namanga and Mlolongo rest-stops in Kenya, the early days of the viral outbreak were marked by confusion as alarming information circulated online.
“Here at the border most of our clients are the truck drivers,” she said. “At first we did not know that mpox could be transmitted through contact. Health officials explained what symptoms to look out for, as well as measures we could take to ensure our safety and that of others.”
Frontier and frontline
On the frontline of mpox surveillance at Namanga, Nurse Officer Mercy Wanjiru, who works with the Port Health Authority, remembers the early days of the mpox epidemic as shrouded in fear and stigma. But she also credits the government for taking swift action.
Health ministry operatives trained up port staff on the then-unfamiliar disease, and quickly shared official guidelines on how to deal with suspected cases.
“We confirmed the first cases by observing symptoms from the travellers while screening them, because mpox is something that you can [often] see physically.”

The Namanga Port Health Authority worked closely with Namanga Health Centre from where, according laboratory technician Evans Lein, samples from suspected cases were dispatched to Nairobi for confirmation.
In the meantime, a concerted effort to sensitise truck drivers and sex workers in the border town continued. “These two groups interact a lot, so we first sensitised clearing agents who helped sensitise truck drivers,” Lein noted.
Apart from the truck drivers’ association and sex workers’ representatives, the Ministry also worked closely with partners like WHO, UNICEF, Africa CDC and AMREF to bring key populations up to speed on disease control guidelines.
Have you read?
Getting protected
In September of 2025, The Ministry of Health received 10,700 doses of the mpox vaccine from Gavi. With the advice of WHO and the help of partners, those doses were deployed to three counties along the country’s principal transport corridor: Busia, Nakuru and Mombasa.
“Coordination teams deployed the vaccines from Nairobi central vaccine stores to the vaccination teams. The final recipients of the vaccines were truck drivers, sex workers and frontline healthcare workers,” confirmed Muthoni.
“The choice to vaccinate [only] these groups was also informed by the few number of vaccine doses. We therefore had to identify the most high-risk groups, which also included frontline healthcare workers, who usually come in contact with infected individuals as they manage them.”
MOH confirms that 10,697 people have been vaccinated so far and the ministry aims to vaccinate more as they await to deploy the additional 20,000 doses of mpox vaccines received from Gavi.
“Vaccines save lives,” concluded Muthoni. “Both routine as well as reactive campaigns are crucial, because vaccines are a key cornerstone for disease prevention.”
The Ministry of Health in Kenya has also increased its surveillance and sensitisation efforts to protect the wider population from renewed spread.