Malaria vaccines are working. We cannot afford to lose momentum.
This World Malaria Day we can celebrate one of the most rapid and successful vaccine introductions in history. Our mission now is to sustain this progress.
- 25 April 2026
- 4 min read
- by Sania Nishtar

For thousands of years, malaria has been a relentless presence in the lives of millions of families, claiming hundreds of thousands of young lives every year and placing an unbearable burden on health systems. And while in recent decades the prospect of a malaria vaccine had begun to offer the prospect of a new tool to turn the tide against this ancient disease, its progress had felt frustratingly slow.
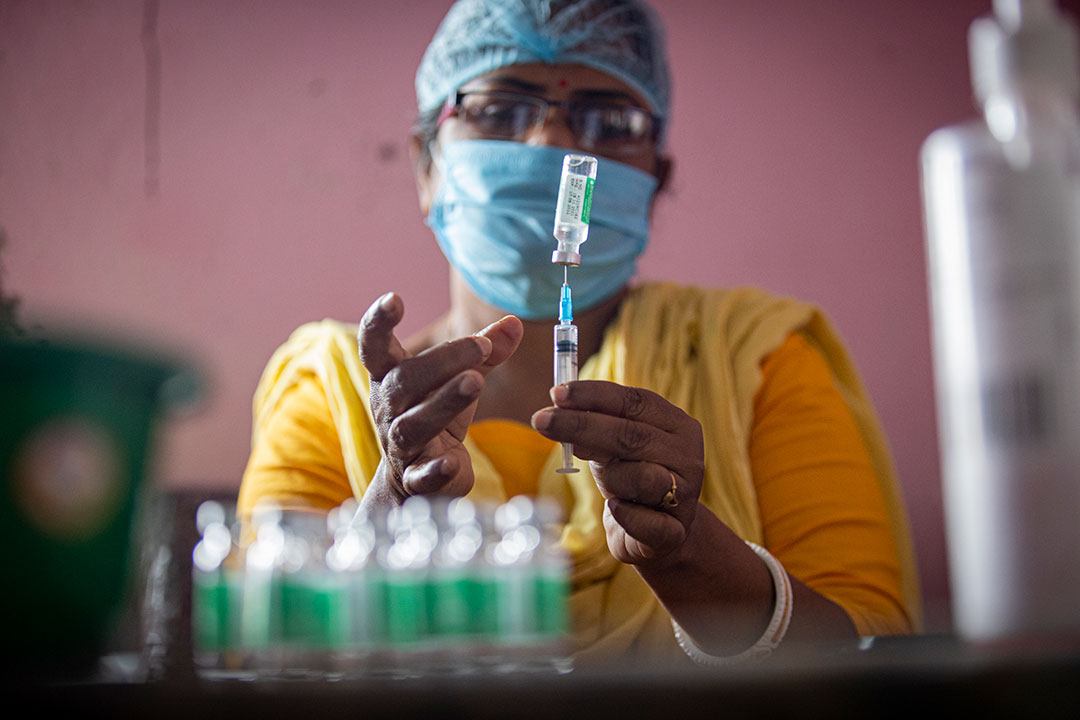
In 2024, things changed dramatically. Since that time, 25 African countries have introduced malaria vaccines into their routine immunisation programmes with the support of Gavi, the Vaccine Alliance, making this the fastest routine vaccine rollout in Gavi’s history. Already, over 50 million doses have reached children living in some of the world’s highest burden settings.
This is a historic milestone, not just because a malaria vaccine exists but because it is now being delivered at scale, through national immunisation systems, to the communities that need it most.
Are malaria vaccines making a difference?
The evidence emerging from countries already using the vaccines is compelling.
Early reports from Kenya, Malawi, Ghana and Cameroon are showing substantial reductions in severe malaria cases and hospital admissions among vaccinated children. These findings align with data from the earlier pilot programmes, which demonstrated that both first‑generation malaria vaccines – RTS,S and R21 – were over 70% effective in preventing cases during the first year when given ahead of peak rainy seasons.
This doesn’t match the efficacy of other vaccines that Gavi provides, but the overwhelming burden of malaria on the African continent means that 180,000 young lives could be saved by 2030 thanks to the vaccine.
The impact is even clearer when we look at country‑wide data. In Burkina Faso the introduction and nationwide expansion of malaria vaccination, alongside other established malaria control measures, helped drive a 32% reduction in malaria cases between 2024 and 2025.
Among children under five, the group most vulnerable to malaria, the reductions were particularly sharp. Overall, malaria‑related deaths fell by around 50%.
These are the kinds of results global health practitioners work toward for decades, and rarely achieve so quickly.
Why do first‑generation vaccines matter so much?
RTS,S and R21 are often described as “first‑generation” malaria vaccines. That term matters.
They are not the final word in malaria prevention. But they are the essential bridge between decades of research and a future where second‑generation vaccines could deliver even higher efficacy, longer duration of protection and simpler dosing.
Investing in these first vaccines does two things at once. It saves lives today by reducing the huge burden of illness and death among children at highest risk. And it builds the evidence, delivery experience and market certainty that stimulate innovation for tomorrow. The demand for malaria vaccines remains high.
Without sustained deployment of RTS,S and R21, the pipeline of next‑generation malaria vaccines becomes weaker, not stronger.
In global health, breakthroughs rarely come fully formed. They are built step by step, on the back of earlier successes that prove what is possible.
What has Gavi achieved and what is now at risk?
Gavi’s malaria vaccine programme stands among its most successful introductions. Over the next five years, the Vaccine Alliance aims to help countries fully vaccinate 50 million additional children.
But this ambition now faces a stark constraint. Gavi has not yet reached its fundraising target and is operating in the context of a 30% funding shortfall. As a result, difficult choices have had to be made.
We are prioritising support for the lowest‑income countries, guaranteeing sufficient malaria vaccine supply to cover up to 70% of eligible children, focused on areas of moderate to high transmission. For countries preparing to transition away from Gavi support, however, we cannot offer the same assurance. In these settings, rollout may slow, access to malaria vaccines may suffer and momentum could be lost.
This is particularly concerning at a time when climate change is expanding malaria transmission zones and intensifying seasonal risk.
If you’re interested in malaria, read next
Why does sustaining momentum matter now more than ever?
One of the greatest risks in global health is success followed by complacency.
The rapid and remarkable rollout of malaria vaccines has shown what is achievable when political will, science and financing align. But progress against malaria has never been linear. History has taught us that hard‑won gains can be reversed when investment falters.
With full funding, Gavi could do more to expand coverage, support all countries that need the malaria vaccine and ensure that today’s success fuels tomorrow’s innovation. The reward will be counted in millions of children, countless communities, spared the suffering malaria brings.
This World Malaria Day, the message is clear: we are finally turning the tide against one of humanity’s oldest diseases. Now we must ensure we do not loosen our grip just as victory comes into view.