Vaccines, bed-nets and insecticides team up to fight malaria on the shores of Lake Victoria
Siaya is one of Kenya’s most malaria-plagued counties, with a prevalence rate of almost 30%. But health workers say a combination of vaccines and environmental defences promise improvement.
- 23 April 2026
- 6 min read
- by Edna Osuo

At a glance
- Siaya County in Kenya has a staggering 29% malaria prevalence rate. Of all the people admitted to county hospitals with fevers last year, 70% tested positive for the mosquito-transmitted infection.
- Locals are ready to do what it takes to protect their children from the disease – and that means mounting a layered defence. Bed-nets build a barrier, spraying kills the insects, and for the youngest and most vulnerable, immunisation offers a portable, internal shield.
- Nurse Maureen Apiyo says cases among the immunised cohort are fewer and less severe already, and she expects to see the malaria burden decline further in the coming period.
Ruth Akinyi was all smiles as she stepped out of the immunisation room of Wagai Sub County Hospital in Kenya’s Siaya County, adjusting the wrapper around her second-born child. This moment was a milestone: her toddler had just received the final dose of the malaria vaccine.
“I didn’t want my child to suffer the way I did while growing up,” she said. “When I first came to this facility, the health workers explained to me the importance of the child having the malaria vaccine – the reason I made sure that I completed all the four doses.”
That wasn’t all Akinyi had done. As recommended, she’s constructed what’s referred to by health workers as a “layered defence” in her home: immunisation for her youngest, and insecticide-treated mosquito nets and Indoor Residual Spraying (IRS) for the entire household.
“For sure I have seen their importance in protecting my family,” she said.
Malaria hotspot
Joseph Siaya County, located on the shores of Lake Victoria, remains one of Kenya’s hardest-hit malaria zones. According to Joseph Ogutu, Acting Malaria Research Coordinator for the county, malaria prevalence here stands at about 29%: significantly higher than the national average of roughly 6%.
Proximity to the lake, coupled with warm temperatures, helps to create favourable conditions for the Anopheles mosquito, the primary vector for malaria transmission, to breed.
Of the patients that presented to Siaya health facilities with a fever last year, as many as 70% tested positive for malaria, said Ogutu.
Health authorities in the county are not only targeting the mosquitoes, but deploying a holistic strategy that targets both the mosquitos and the human.
Treated bed-nets are handed out free-of-charge at health facilities, and create a physical and chemical barrier between sleeping humans and hungry mosquitoes. Indoor Residual Spraying (IRS), meanwhile turns homes into a deadly environment for the insects.
“The Anopheles mosquito tends to rest on walls before and after biting,” Ogutu explains. “By spraying the walls, we kill them at that point.”
The malaria vaccine, which has been administered in Siaya since 2019, when Kenya became one of three countries to participate in the pioneering Malaria Vaccine Implementation Programme, is the newest ‘layer’ in the layered defence. Preventive treatment for pregnant women (IPTp), using sulfadoxine-pyrimethamine, improves protection for this particularly vulnerable group.
“Each intervention plays a very important role, but none is sufficient on its own,” says Ogutu. “The idea is to combine methods to protect the people, and at the same time to attack the mosquito. That is how you reduce transmission.”
Powerful, portable protection
The vaccine is administered in four doses, starting at age six months. “It does not completely prevent infection, but it significantly reduces the risk of severe illness and death,” said Maureen Apiyo, a nurse at Wagai Sub-County Hospital.
She further explains that such kind of limitation is expected. “Malaria is caused by a parasite, which is far more complex than a virus or bacteria,” Apiyo explains. “That is why the vaccine cannot fully stop transmission. But it adds a powerful layer of protection.”
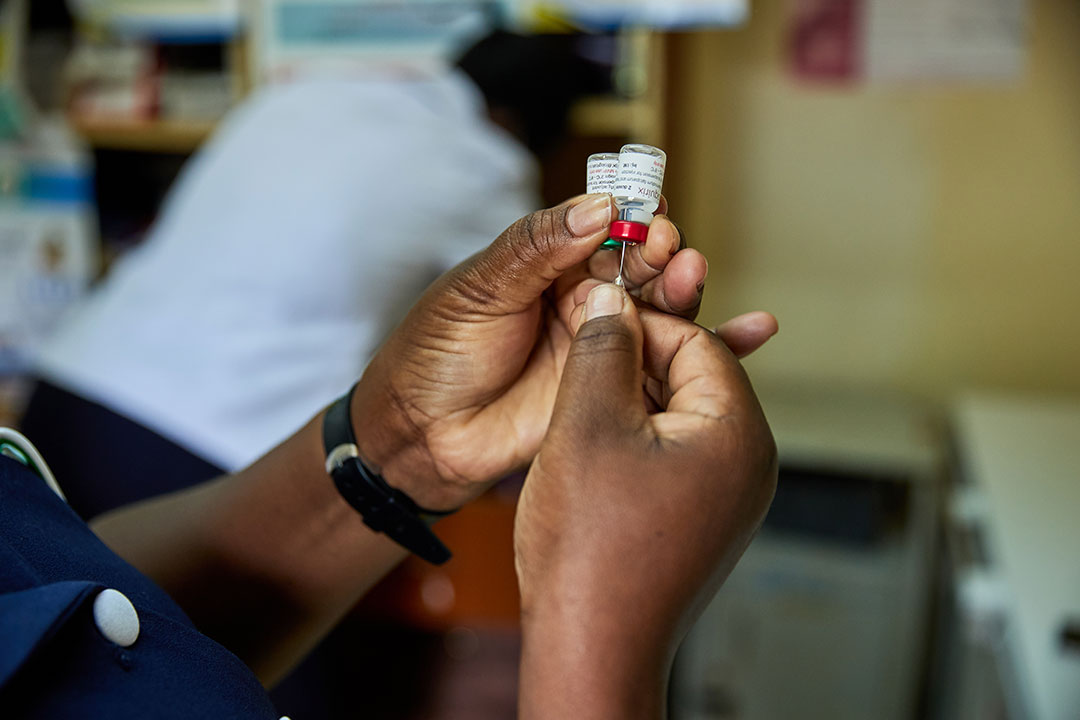
Gavi/White Rhino Films-Lameck Orina
She further emphasises that unlike mosquito nets or sprayed walls, the vaccine works internally. “It is the protection a child carries at all times that helps their immune system respond more effectively when exposed to malaria,” said Apiyo.
On an average day, Apiyo says she vaccinates between 10 and 15 children, with many of those receiving malaria doses.
“The response from parents and guardians has been largely positive,” she says. “We first take them through health education and after they understand why the vaccine is important, we then proceed to administer the vaccine.”
She has also observed a shift in outcomes. “We are seeing fewer severe cases and complications,” she tells VaccinesWork. “Nowadays, when vaccinated children get malaria, the severity is much lower than before.”
Challenges still remain
Children not getting all the doses has been the greatest challenge her team has faced, Apiyo says.
“The last dose, given at around two years, is the hardest one,” she says. “Some parents stop after the earlier doses, because the child looks healthy.”
To address this, health workers actively follow up with caregivers through phone calls and via community health promoters. They also make sure to remind families not to compromise on environmental protections. “While the vaccine protects from within, mosquito nets remain one of the most effective tools, and IRS work externally to prevent infection in the first place,” adds Apiyo.
Have you read?
According to Apiyo, Siaya county presents a high mosquito nets ownership, standing at 95%, but proper usage is slightly lower, with some cases of misuse reported.
To address this, community health promoters conduct household visits and health education sessions to reinforce the correct use.
Siaya recently conducted its first large-scale IRS campaign, reaching over 100% of its targeted households, with coverage exceeding 273,000 structures, according to Apiyo. “Although formal impact studies are ongoing, early community feedback suggests a reduction in mosquito presence,” she adds.
Protecting mothers and new life
“Today being my first antenatal visit, I have already received a mosquito net and preventive malaria medication,” said Beryline Akoth, a patient at Wagai Sub-County Hospital.
Akoth said she has learned how to take care of and protect the unborn baby from malaria. “After delivery I will also bring my baby for all the doses required to prevent the baby from diseases,” she adds.
Pregnant women are among the most vulnerable to malaria, facing risks that extend to their unborn children. “Through routine antenatal care, they receive nets and intermittent preventive treatment to reduce infection risk,” Apiyo explains.
Health experts stress that the success of malaria control in Siaya depends on how well the various preventive interventions work together. “No single tool can eliminate malaria, but together, combined, they can significantly reduce infections, hospitalisations and deaths,” Apiyo emphasises.
“If we sustain this approach of using vaccinations, nets and spraying, we expect to see a decline of cases.”





