Two years after the introduction of the malaria vaccine, Burkina Faso celebrates its impact
Malaria cases and deaths declined significantly in 2025, according to national data.
- 24 April 2026
- 7 min read
- by Abdel Aziz Nabaloum

On 20 April 2026, in Ouagadougou, Antonia Konditamdé receives a dose of the malaria vaccine. For her mother, Florence Kayendé, who lives in Bonheur-Ville, a working-class neighbourhood on the southern outskirts of the capital, the vaccination brings relief above all.
In Burkina Faso, where malaria has long been a rainy season fixture, fuelling an annual swelling of anxiety among parents, the opportunity to better protect her child means a lot to Kayendé. “My child was vaccinated at five months, and again at six months. I find the vaccine very effective. I really appreciate the impact it has had on my daughter,” she says.
Like many Burkinabè, Kayendé has more than a passing personal acquaintance with the parasitic infection. For her family, malaria has meant anxious nights, repeated clinic visits and costs that were difficult to bear. She recalls a previous episode of malaria, affecting another of her children, that required several days of care. Today, she encourages other mothers to have their children vaccinated and to make sure they sleep under mosquito nets.
Rihanata Kouanda, mother of young Mohamed Sanfo, says the best tactic is combining preventive measures. That’s something she’s learned from the community health workers who regularly visit her neighbourhood to raise awareness: keeping living environments clean, eliminating mosquito breeding sites and administering monthly doses of seasonal chemoprevention to children during peak transmission periods are important. Her son has also been vaccinated. “We have benefited from all these prevention measures free of charge. The malaria vaccine is part of routine immunisation. It is a real opportunity for us as mothers. To protect my child properly, I did not hesitate to have him vaccinated,” she explains.
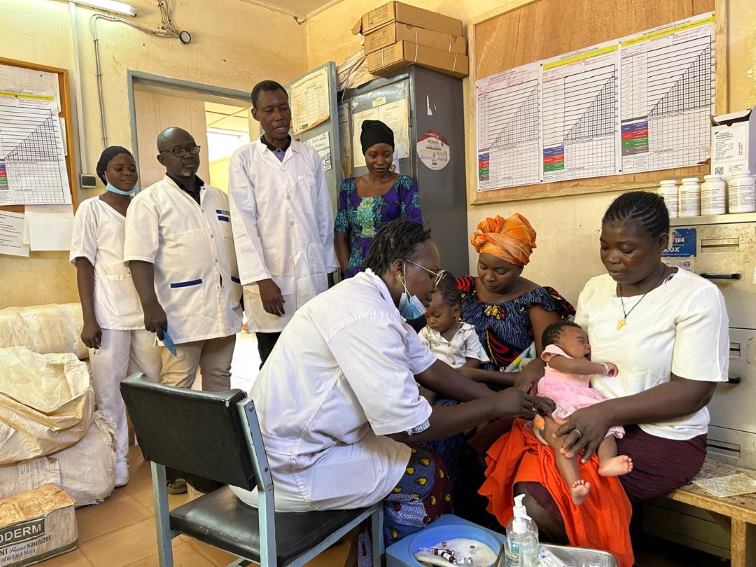
Credit: Abdel Aziz Nabaloum
Beyond the sense of relief, she also points to the economic benefits. According to her, a decline in malaria episodes has spared her family healthcare costs that were once difficult to afford. “It has helped us save what little money we have. Just imagine what we used to spend on treatment every time malaria struck,” she says.
A decline reflected in the data
Authorities report an unprecedented decline in malaria rates at the national level. At a press briefing in February 2026, Health Minister Robert Kargougou said the total number of recorded malaria cases fell from 10,805,020 in 2024, to 7,329,278 in 2025, a decrease of 32%. Over the same period, deaths fell from 3,523 to 1,979, a drop of 44%. Among children under five, cases declined by 39%, while mortality fell by more than 40%.

Credit: Abdel Aziz Nabaloum
Beyond national figures, health workers say they are seeing the change in their day-to-day practice.
At the Cissin 17 Health and Social Promotion Centre (CSPS) in Ouagadougou, mothers wait outside the vaccination-and-weighing room, babies in their arms. Several say they have seen malaria episodes decline among their children thanks to stronger prevention. “My youngest child received free malaria tablets during the seasonal malaria chemoprevention campaigns. It’s a real opportunity for our country to have access to these products,” says Assita Traoré, who also reports fewer cases in her community more broadly.
Boubakaré Sawadogo, Head Nurse at Cissin 17, observes the same trend in his catchment area. Among children under five, the centre recorded 2,699 suspected cases, including 944 confirmed, in 2024, compared with 2,072 suspected cases, including 538 confirmed, in 2025. Among pregnant women, suspected cases fell from 1,231 to 733, and confirmed cases from 548 to 231.
This February, Health Minister Robert Kargougou reported that the total number of recorded malaria cases fell 32% between 2024 and 2025. Fatalities dropped by 44%.
“Often, when we compile weekly statistics on treated conditions, we find there are no malaria cases at all among children or pregnant women,” he says. For him, this clearly reflects a real decline in the disease.
A combination of interventions
At Cissin 17, as elsewhere, health workers emphasise a key point: this decline cannot be attributed to a single measure.
It is the result of multiple strategies deployed simultaneously, including seasonal malaria chemoprevention, distribution of long-lasting insecticidal nets, elimination of mosquito breeding sites, indoor spraying, rapid diagnosis, availability of treatment and free medicines for certain vulnerable groups.
Malaria vaccination, the newest technology to bolster Burkina Faso’s defence against the disease, strengthens an already multifaceted response. The vaccine is administered in four doses, scheduled at 5, 6, 7 and 15 months of age.
“With all these measures combined, we are seeing a real impact on reducing cases. The vaccine has further strengthened the fight against the disease,” says nurse Boubakaré Sawadogo, who also notes strong demand from families at his facility.
Nebilbié Bayili, head of the Expanded Programme on Immunization (EPI) at Cissin 17, highlights the positive reception of this new protection. According to him, the burden of malaria, both in terms of household spending and emotionally, has played a major role in encouraging uptake. “Because malaria causes so much harm and expense, when parents hear that a vaccine exists, they are willing to have their children vaccinated,” he says.
Nebilbié Bayili, head of the Expanded Programme on Immunization (EPI) at Cissin 17, highlights the positive reception of this new protection. According to him, the burden of malaria, both in terms of household spending and emotionally, has played a major role in encouraging uptake. “Because malaria causes so much harm and expense, when parents hear that a vaccine exists, they are willing to have their children vaccinated,” he says.
Fewer severe cases in health facilities
At the Pissy Medical Centre in Ouagadougou’s District 6, the picture is similar. In paediatrics, where the most severely ill children are referred, staff report a noticeable easing of pressure.

Credit : Abdel Aziz Nabaloum
“Between 2024 and 2025, we clearly saw a decline in severe malaria cases. During the rainy season, we usually expect to be overwhelmed, but that wasn’t the case last year,” explains Clarisse Toé, a specialist obstetric nurse and ward supervisor in the paediatric unit.
If you’re interested in malaria, read next
She attributes the improvement both to the various preventive measures being rolled out, and to prompt treatment of mild cases, which can help stave off the development of dangerous complications. When severe cases do still occur, she adds, they often involve children who have not benefited from the full range of preventive measures.
On the ground, grassroots health workers also report a shift. Gilbert Ouédraogo, a community health worker, says families are increasingly adopting preventive behaviours: sleeping under mosquito nets, keeping surroundings clean, following prevention campaigns and vaccinating their children. He warns, however, that the gains he’s seen will only last if efforts continue.
Real progress, but still fragile
For those leading the national malaria programme, the results seen in 2025 are encouraging, but they must not lead to complacency.
The Permanent Secretary for Malaria Elimination, Sidzabda Kompaoré, stresses that malaria remains a major public health challenge despite recent progress. “We now have effective tools to prevent and treat malaria. It is therefore no longer acceptable for people to die from this disease,” he says. He also notes that malaria vaccination has now been rolled out across all health districts in the country, and calls for every opportunity to further strengthen prevention to be seized.
The authorities’ stated ambition is to eliminate malaria by 2030. But on the ground, health workers and community agents are clear: the progress observed in 2025 is only possible because multiple tools are being used together, at scale and close to communities. In other words, malaria is no longer as inescapable as it once was in Burkina Faso — but the efforts to out-manoeuvre it must be kept up.
How is Gavi helping?
In Burkina Faso, malaria vaccination is being implemented by the government with support from several partners. Gavi contributes to financing the programme, while UNICEF supports vaccine supply, cold chain systems, training and community mobilisation. The World Health Organization provides technical and normative guidance. Other partners, including Jhpiego and USAID, have also supported the roll-out.








