How will COVID-19 vaccines be approved for use in Australia?
Australia is set to get the green light to roll out the Pfizer vaccine any day now. There is a complex process behind this.
- 28 January 2021
- 6 min read
- by The Conversation
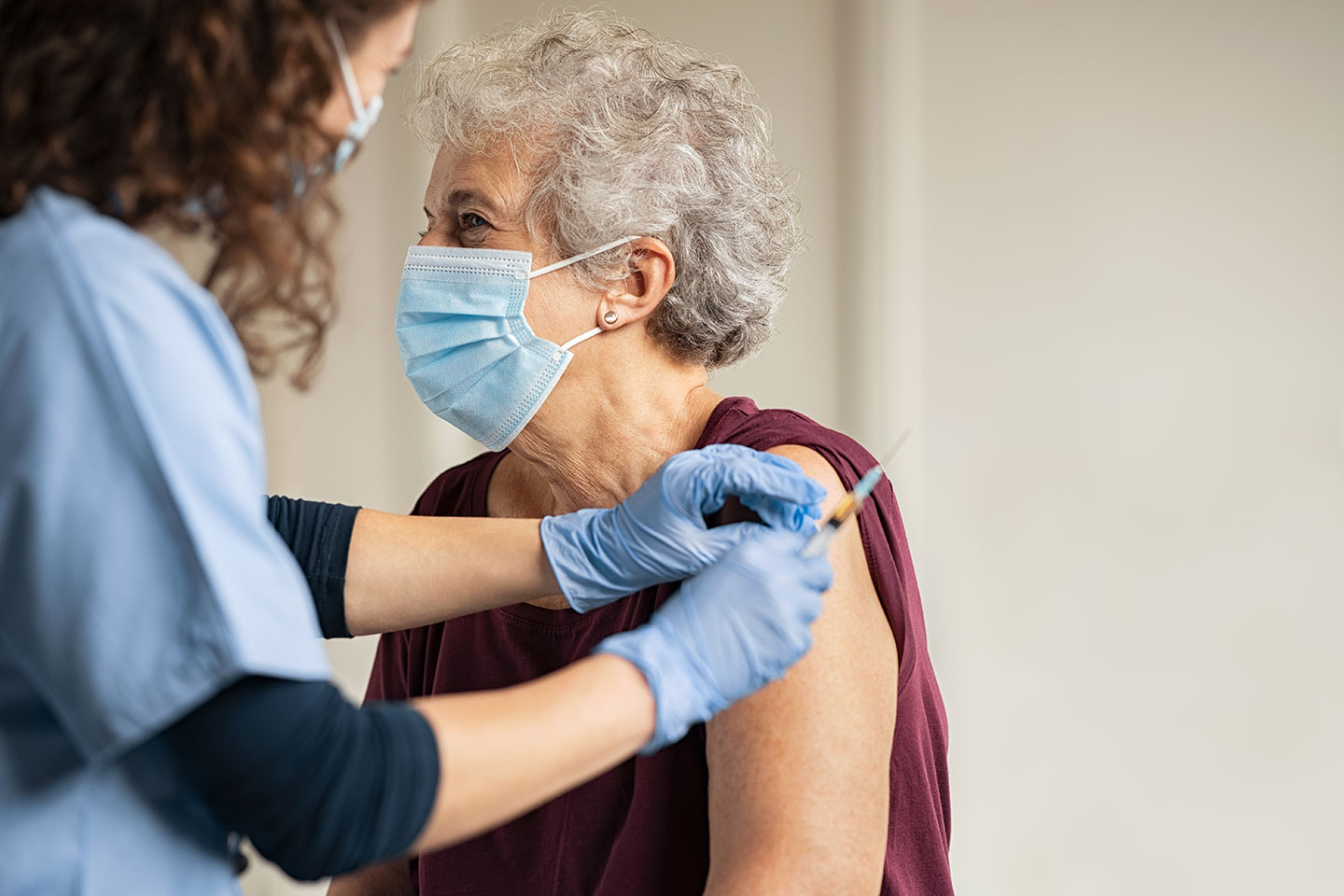
Some Australians could be receiving a COVID-19 vaccine within weeks.
Amid the continued spread of the virus and emergence of highly contagious variants, the federal government has accelerated the start of the roll out — initially set for March 2021 — to February.
Other countries, who have been less successful in containing the virus, have already begun vaccination programs. While this has been met by celebration around the world, there have also been concerns about possible side-effects.
It is expected the Therapeutic Goods Administration (TGA) will approve the Pfizer vaccine for use in Australia any day now. Approval for the AstraZeneca vaccine is expected in early February.
Given the uncertainty surrounding the virus and the speed at which vaccines have been developed, what processes are in place to assure Australians’ safety?
What is the TGA?
The TGA is part of the federal Health Department. Its job is to regulate any product that carries a therapeutic claim. This includes prescription drugs, medical devices, certain food supplements, and of course vaccines.
It maintains the Australian Register of Therapeutic Goods (ARTG), which records every therapeutic good available in the country.

The TGA regulates therapeutic goods in two main ways. First, it authorises products so they can be put on the ARTG and distributed. This involves its experts reviewing safety and efficacy data.
It then monitors products once they are in use. This includes collecting, analysing and reacting to data from health-care providers, patients, manufacturers, and overseas regulatory authorities.
How does it work?
The TGA says it adopts a “risk-based approach”. That is, it must be satisfied a vaccine or medication’s benefits outweigh its risks.
The TGA therefore is not tasked with the impossible goal of avoiding all risks. Rather, it must make sure that only products carrying acceptable risks can be marketed.
So, for example, common minor side effects (such as a stomach ache) associated with certain painkillers are deemed acceptable compared to their benefit. Similarly, a severe but rare side effect can be acceptable where the medical benefit is significant. This is the case with vaccines.
Along with internal scientific and medical staff, the TGA is advised by seven committees, providing independent expert advice on scientific and technical matters. There includes a specific committee for vaccines.
Have you read?
Vaccine approval under ‘normal’ circumstances
The TGA requires a manufacturer or importer (the “sponsor”) to demonstrate the safety and efficacy of their product.
That is, companies need to show not only that their product is not harmful, but it does what it is supposed to do.
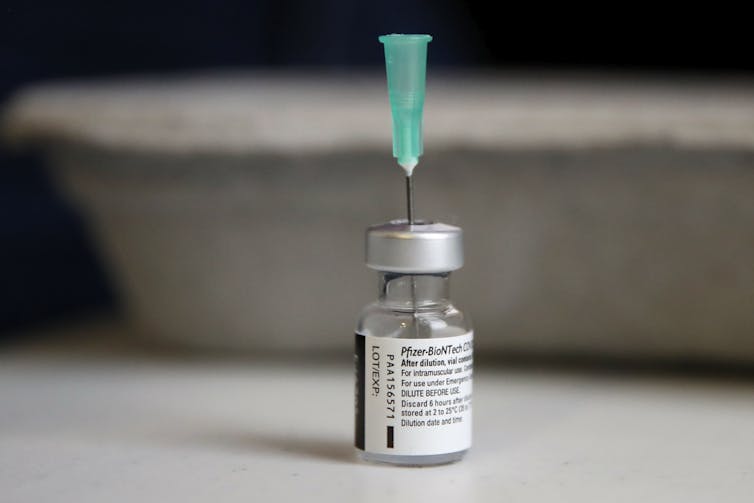
Sponsors must submit a substantive body of clinical data, gathered according to Good Clinical Practice guidelines, which are developed in keeping with world’s best practice.
The TGA also reviews the data using internationally recognised guidelines from the European Medicines Agency.
The key data for approval arises from the third phase of clinical trials. These test a new product on very large groups, which can number in the tens of thousands. The TGA review can take up to eleven months.
If a therapeutic good is approved, but a problem later emerges, the TGA can recall it.
Special provisions for COVID-19 vaccines
The devastating speed of the COVID-19 pandemic has prompted regulatory authorities across the world to speed up approval processes.
Almost all have used existing special provisions to fast-track their reviews. Importantly, clinical trials have been conducted at unprecedented speed thanks to unlimited funding and motivated volunteers.
The scientific consensus is that the rigour of clinical evaluation has not been compromised.

Similarly, the TGA can conduct a speedier review of clinical data.
Instead of reviewing all the data prior to registration, the TGA conducts a preliminary assessment. This is followed by rolling submission of clinical data, leading to provisional registration. In other words the process is accelerated by allowing the TGA to look at data on an ongoing basis.
This special pathway is in place for treatments or vaccines for life-threatening diseases.
A provisional registration means the vaccine is approved for a set period of time (to be determined by the TGA), during which vaccinations can start under close monitoring. Following this, the vaccine proceeds to full registration.
Benefits outweigh risk
Both the Pfizer and AstraZeneca vaccines have conducted phase three trials on tens of thousands of participants. Additionally, the TGA stresses it will only approve provisional registrations when the data so far makes clear
the benefit of early availability of the medicine outweighs the risk inherent in the fact that additional data are still required.
In the context of COVID-19 vaccines, provisional registration reduces bureaucratic hurdles, while maintaining the highest possible scientific rigour.
Working with the international community
The TGA does not operate in a vacuum either.
Regulatory authorities worldwide and the World Health Organisation have committed to work together on COVID-19 vaccines and medicines to improve “regulatory alignment”.
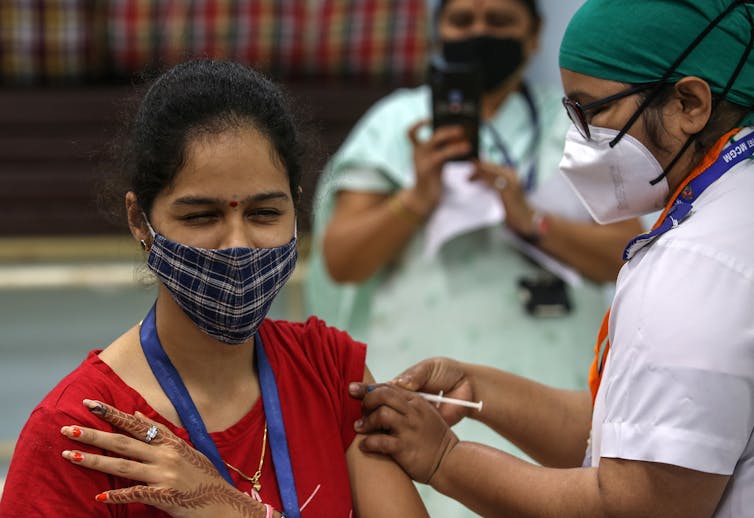
The TGA is a member of the International Coalition of Medicines Regulatory Authorities, which has committed to full cooperation and transparency between its members, particularly with regard to sharing data.
The TGA is also part of the Access Consortium alongside regulatory authorities from Singapore, Canada, Switzerland and the United Kingdom.
So, while the speed of development of the first COVID-19 vaccines is unprecedented, so is the level of global monitoring over their safety and efficacy.
Authors
 | Marco Rizzi | |
 | Katie Attwell |

This article is republished from The Conversation under a Creative Commons license. Read the original article.
Disclosure statement
Marco Rizzi receives funding from the WA Department of Health.
Katie Attwell receives funding from the Australian Research Council and the WA Department of Health. She is currently funded by ARC Discovery Early Career Researcher Award DE1901000158. She is a member of a government advisory committee, the Australian Technical Advisory Group on Immunisation (ATAGI) COVID-19 Working Group. All views presented in this article are her own and not representative of any other organisation. Dr Attwell has also received speaker's fees from Merck in the past.
Partners

University of Western Australia provides funding as a founding partner of The Conversation AU.








