As Burundi prepares to roll out vaccines against a leading cancer killer, survivors take stock
For Irakoze Gratia, diagnosis with cervical cancer was the start of a long, painful, expensive journey back to health. But as a survivor, she’s one of the lucky ones. She hopes the next generation won’t have to roll those dice.
- 13 April 2026
- 5 min read
- by Moses Havyarimana

At a glance
- In Burundi, more than 1,000 women die of cervical cancer – a preventable scourge – each year.
- With the country set to roll out the cervical cancer-preventing human papillomavirus vaccine to adolescent girls this month, survivor Irakoze Gratia is clear: “I advise all women to get vaccinated against HPV… take this advantage before it’s too late.”
- Gratia knows that even survival has a steep cost – not just in emotional terms, but also financially. To access life-saving treatment she borrowed from friends and family. The vaccine, by contrast, will be free of charge.
Cervical cancer survivor Irakoze Gratia, a Bujumbura resident, is one of the lucky ones. But still, it’s been a long and turbulent road from her diagnosis back to health.
“I started getting abnormal reactions in 2013 when I experienced endless menstrual periods,” recalls the 50-year-old mother of two. “Sometimes I experienced menstrual period twice a month. I am a driver and, in my mind, I thought it was because of the work or fatigue.”
She visited more than one Bujumbura doctor, leaving each time without a clear diagnosis. Her symptoms progressed. Around November 2016, she noticed a “liquid with bad odour,” and rushed back to hospital. She had a scan which, she says, “revealed wounds around my cervix”.
In 2017, gynaecologists confirmed that she had cervical cancer. “I started chemotherapy in September 2017 as the doctors told me I had stage 2B of cervical cancer. I followed all the protocols and the month after I was advised to go through radiotherapy.”
Meantime, her financial worries were growing. Irakoze is a taxi driver with a local transport service in Burundi, and raises her two daughters on her own, while her husband lives abroad. During her illness, keeping up with bills became impossible.
And then, she learned that she would need to travel all the way to India for radiotherapy.
She managed to raise the funds she needed from family and colleagues, and in January 2018, she set off. “I travelled to India for three months leaving behind my 10- and 12-year-old girls with relatives. It was really the hardest time in my life… the process drained me physically, emotionally and especially financially,” Gratia says.
But for Gratia, unlike for the approximately 1,100 Burundian women who die of cervical cancer each year, the story ends well. “I thank God that after three months in India I was told that I am cancer-free. It is now almost eight years since then and I am living a healthy life.”
Too late for too many
Dr Ndayikunda Innocent, a well-known gynaecologist practising at the private Procrea Polyclinic in Bujumbura, says that a large majority of cervical cancer patients in Burundi still get diagnosed far too late.

Credit: Moses Havyarimana
“The problem of women here, is that most of them come for consultation in critical conditions and when it’s already late. It is better if women between 25–65 years do annual screening, which gives a better chance of getting treated [successfully].”
Dr Ndayikunda indicates that certain groups of people ought to get screened more often than others: specifically those living with HIV/AIDS. “Women suffering from AIDS in most cases are vulnerable in getting cervical cancer because of the reduction of immunity in their body,” he explains.
Indeed, screening for 70% of women by age 35, and again by age 45, is one pillar of the WHO’s Cervical Cancer Elimination Initiative. The other two pillars are treatment for 90% of women in need, and preventive human papillomavirus (HPV) vaccination for 90% of girls by age 15.
An ounce of prevention
The HPV virus is extremely common, and causes the overwhelming majority of cases of cervical cancer. It’s also preventable with a single dose of vaccine.
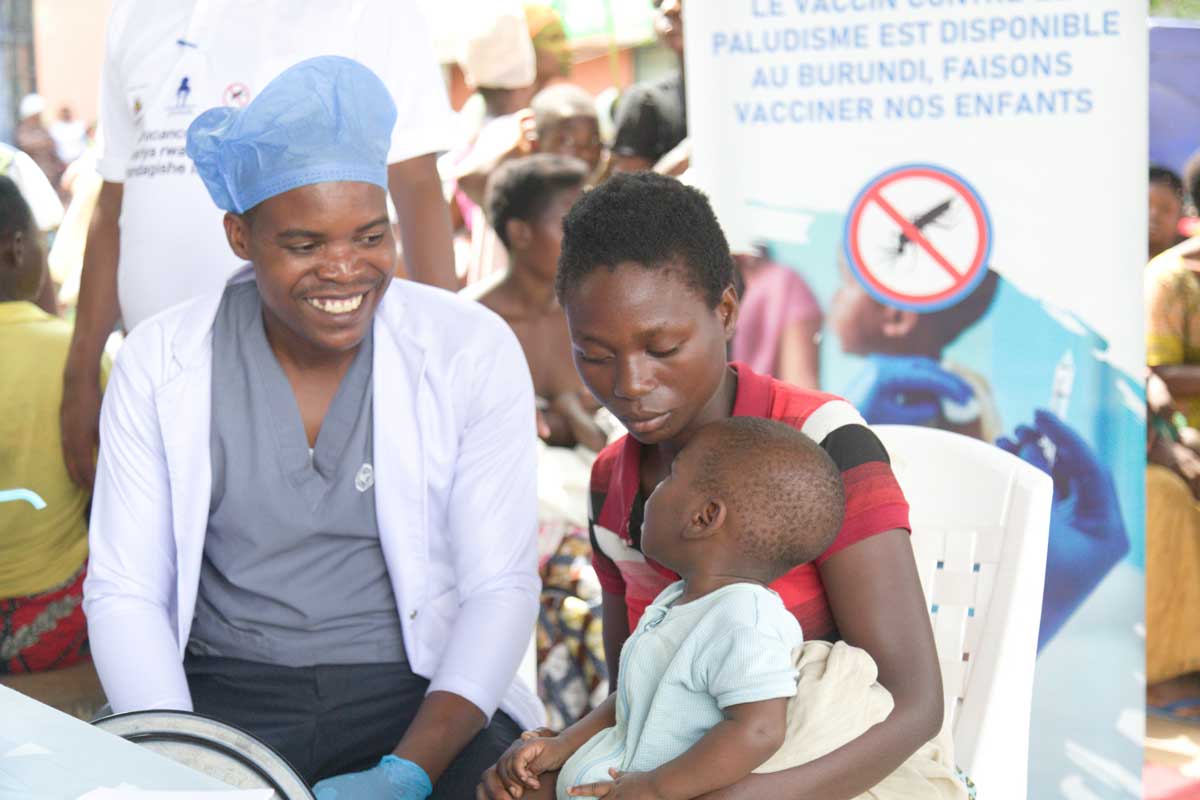
This World Cancer Day, the Ministry of Health released a statement celebrating the upcoming inaugural public roll-out of that vaccine to Burundian girls aged 9 to 14.
“Burundi [will introduce] the HPV vaccination in phases with the ultimate goal to integrate it into the Expanded Programme on Immunization,” confirmed Dr Polycarpe Ndayikeza, the spokesperson for the Burundian health ministry.
Have you read?
The experience of countries with well-established HPV vaccination programmes promises that the roll-out will profoundly alter rates of both disease and mortality in Burundi.
Denmark, a country that introduced the HPV vaccine in 2008, found that high-risk types of HPV had been almost eliminated among vaccinated women a decade later. Researchers in the Netherlands found that vaccinated women had a 90% lower risk of developing invasive cervical cancer than their unvaccinated counterparts.
For Gratia, the utility of prevention is a no-brainer. “I advise all women to get vaccinated against HPV… take this advantage before it’s too late, and conduct annual cervical cancer screening.”
Dr Ndayikunda too projects a profound impact, and in fact advocates for mandated vaccination for eligible girls, to guarantee maximum uptake.
Not just the vaccine
Ministry spokespeople point out that the government’s efforts to roll back cervical cancer don’t end with the jab.
“The government is now taking action on VIA/VILI screenings in health centres. Gradual introduction of HPV testing in selected pilot sites, training of healthcare providers, awareness campaigns were made, and more than 155,000 women were reached by last year,” said Ndayikeza. The government has also said it has initiated the construction of the National Reference Centre for Oncology to improve patient care.
Biopsies and histological confirmation are now available at Kamenge University Hospital, Burundi’s pre-eminent tertiary facility. Surgical treatment is accessible in referral hospitals, but radiotherapy remains “limited”. Regional partnerships with countries including Rwanda and Tanzania remain the main route for patients who need it.