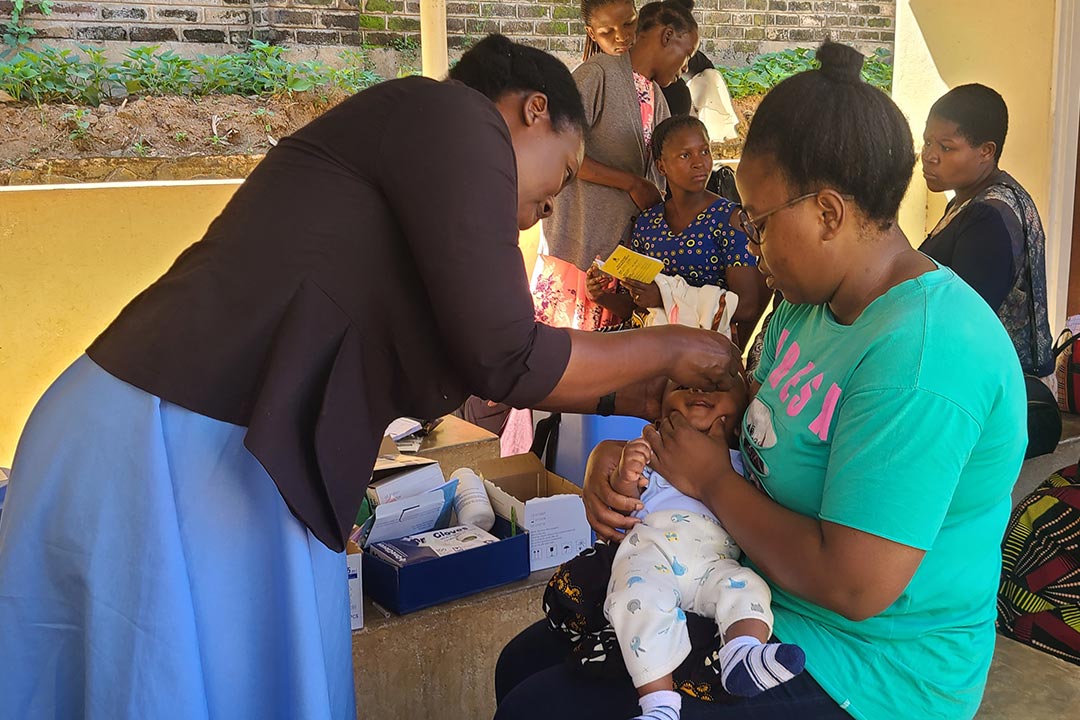
From immunisation to education: how vaccines shape children’s futures
Vaccines don’t just save lives; they shape how children learn, progress through school and build the foundations for their futures.
- 8 April 2026
- 12 min read
- by Linda Geddes

At a glance
- Children exposed to a rapid national vaccination campaign in Burkina Faso in 1984, which saw coverage with measles, meningitis and yellow fever vaccines jump from around 17% to 77% in just weeks, were more likely to attend and complete school. As adults, they were also more likely to enter formal employment and were more productive in agriculture.
- In rural Bangladesh, children whose mothers received tetanus vaccination during pregnancy, protecting them from infection around birth, not only had higher survival rates, but went on to achieve better schooling outcomes, with the largest gains among the poorest families.
- Children born after the roll-out of India’s Universal Immunisation Programme in the late 1980s, which expanded access to routine childhood vaccines nationwide, completed around 0.2–0.3 more years of schooling than those born before.
In 1984, Burkina Faso launched one of the most ambitious immunisation campaigns in modern history.
Within just two weeks, more than a million children were vaccinated against measles, meningitis and yellow fever, increasing national coverage from roughly 17% to 77%.
The campaign, known locally as the Vaccination Commando Program (VCP), was built on the idea that vaccination is one of the most cost-effective ways to save lives and improve children’s life chances.
Its rapid roll-out and the uneven coverage it achieved across regions created a rare natural experiment in the long-term effects of immunisation.
“Within just a few weeks, the government mobilised all its resources to vaccinate children, but without expanding hospitals or hiring more health workers,” says study co-author Prof Harounan Kazianga at Oklahoma State University in Stillwater, US. “That allows us to pin down the vaccination effect.”
Decades later, children exposed to the campaign were not only more likely to have survived early childhood, but to have attended school and completed their education.
The findings, as well as those of other recent studies, increasingly point to an exciting conclusion: that vaccines, long seen as tools of disease prevention, also shape how children learn, how far they progress through school and the opportunities that follow.
“Vaccination definitely has health impacts, but it also has various impacts beyond health,” says Prof Sachiko Ozawa, a health economist at the University of North Carolina at Chapel Hill, US. As policymakers grapple with tighter budgets and rising vaccine hesitancy, understanding these wider effects is becoming increasingly important.

vaccine against measles and rubella. Credit: Gavi/2021/Asad Zaidi
“The evidence has long been clear: vaccines don’t only save children’s lives, they improve educational outcomes and ultimately help economies grow,” said Dan Hogan, Head of Measurement and Strategic Information at Gavi, the Vaccine Alliance. “Every parent wants the same thing for their child: to have a fair chance at reaching their full potential. By boosting access to vaccines worldwide we can help secure that chance.”
How do vaccines shape children’s learning?
Early childhood is a critical window for development. By age three, the brain has reached around 80% of its adult size.
“It is a really vulnerable time of life, where having any major disease episode can substantially hinder your physical and cognitive growth,” says Dr Arindam Nandi, a health economist at the Population Council in New York and One Health Trust in Washington DC.
Some of the diseases targeted by routine childhood immunisation can have particularly damaging effects on development. Bacterial meningitis can lead to hearing or vision loss, as well as long-term difficulties with memory, concentration and learning. Severe measles can also trigger brain inflammation (encephalitis) or sight loss.
Other infections can disrupt children’s development in more subtle ways. For instance, both malaria and repeated diarrhoeal disease episodes can impair physical growth and contribute to stunting, particularly where undernutrition is also common.
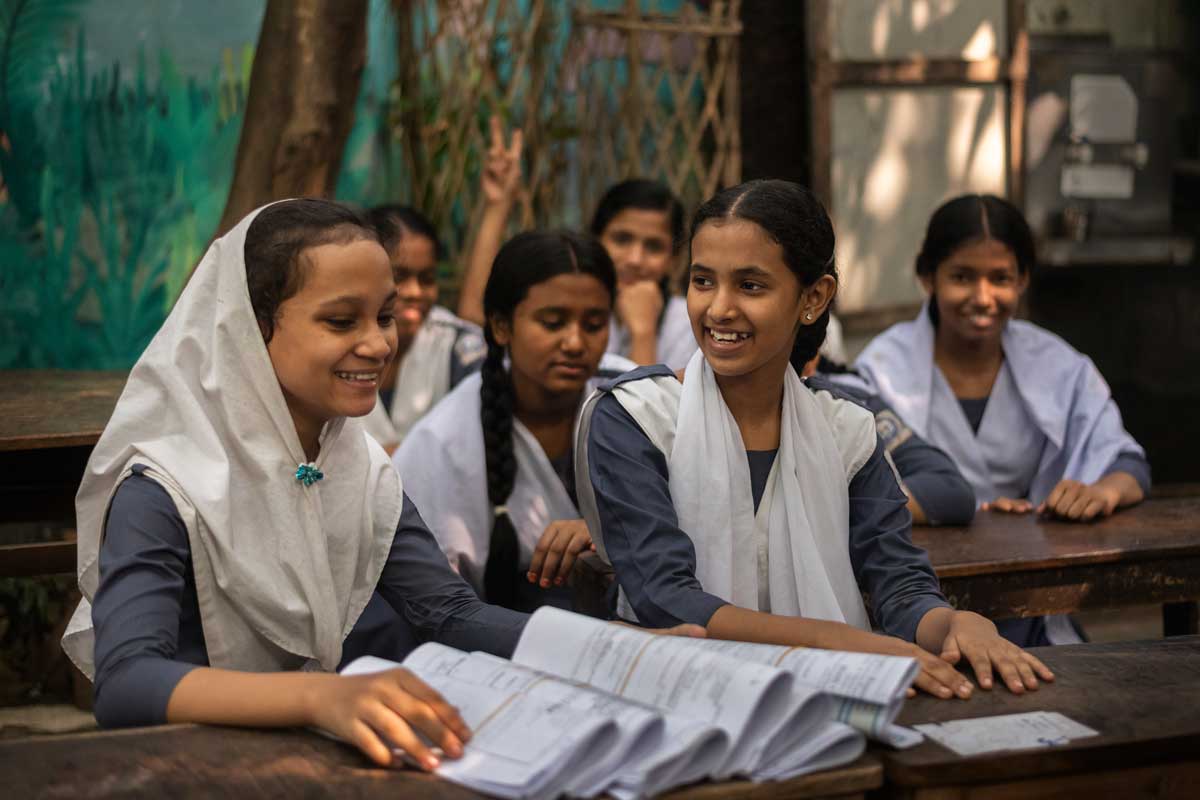
Stunting is strongly associated with poorer cognitive development and later educational outcomes.
Measles can also suppress the immune system – a phenomenon known as immune amnesia – leaving children more vulnerable to other infections for months or even years after the initial illness.
“Even when children are not dying, infections can still result in missed school days and difficulties keeping up with lessons,” says Prof Anita Shet, a paediatrician and infectious diseases researcher at Johns Hopkins University in Baltimore.
The consequences of serious or repeated childhood illness can spread beyond those who are infected.
When children are sick, caregivers may need to take time off work, reducing household income and job stability. In the case of highly contagious diseases such as measles, outbreaks can disrupt entire schools, as rising absenteeism affects both infected children and their classmates.
By preventing these illnesses, vaccination helps protect not only children’s health, but the conditions they need to learn, stay in school and reach their full potential.
It’s not only infant vaccines that can have an impact on children’s learning and education.
Cervical cancer typically strikes women in their 30s and 40s, during their peak parenting years, and is preventable with the HPV vaccine. Besides the emotional turmoil of a mother’s death, it can also have practical consequences.
“Maternal orphans are significantly more likely to drop out of school,” says Shet. “And if the mother is undergoing chemotherapy, or is out of action, that will have an impact on the family and children’s learning as well.”
How much difference do vaccines make to education?
During the 2000s, a growing body of research began linking early-life interventions such as deworming, malaria prevention or nutritional supplementation to improved school attendance and learning. Researchers began to ask whether routine childhood immunisation might have similar long-term effects.
One of the earliest studies focused on tetanus in rural Bangladesh. Tetanus is a severe and often fatal disease that historically claimed many newborn lives, often thorough infections acquired at birth. Survivors can experience lasting health problems that affect brain development and learning.

The Bangladesh-based study examined the impact of vaccinating pregnant women against tetanus. Doing so also protects their infants, because antibodies against the bacterium are transferred across the placenta.
As well as substantially reducing the neonatal death rate, the study found improvements in educational outcomes as these children grew older, equivalent to roughly an additional quarter year of schooling among those from the poorest households.
Similar patterns have since been observed for other immunisations at a much larger scale.
In India, Nandi and colleagues drew on data from the phased roll-out of the country’s Universal Immunisation Programme in the 1980s, which dramatically expanded access to routine childhood vaccines, including the measles, polio and diphtheria, tetanus and pertussis (DTP) vaccine, to compare children born just before and after vaccines became widely available.
By comparing cohorts born just before and after the programme reached different parts of India and, in some cases, even siblings within the same household, the team was able to isolate the effects of early-life vaccination from other factors such as family characteristics or local conditions.
“You’re comparing people from the same or highly similar socioeconomic background, and just asking, ‘Did the child who was exposed to vaccination have higher schooling attainment?’” Nandi explains.
Across multiple analyses, the study found that individuals who were exposed to vaccination in early life completed roughly 0.2 to 0.3 additional years of schooling, with positive effects observed across both rural and urban areas.
While such gains might sound modest, they are meaningful – particularly when they affect millions of children. “If you look at other educational interventions, such as building new schools, they have a similar type of impact in countries such as India,” says Nandi.
“You also have to remember that in many of these contexts, the average level of schooling is not that much. In India, for example, the average was around seven years in the 1990s, so an additional 0.3 years is actually quite a sizeable improvement.”
The results were particularly striking for women: “We found a much larger educational impact on women: almost one extra year of schooling completed for those who got exposed to the vaccination programme in early childhood,” Nandi says.
What about learning outcomes?
However, years of schooling tells only part of the story. Other studies have taken this a step further, tracking individual children over time to examine how vaccination affected not just whether they attended school, but how well they learned.
One such study, known as Young Lives, has followed children in several low- and middle-income countries, including India, Vietnam and Ethiopia, from early childhood into adolescence.
Drawing on this data, Nandi and colleagues found that children who received the measles vaccine in infancy tended to achieve not only more months of schooling, but also modest yet consistent improvements in reading and maths scores.
They observed a similar pattern for the Hib vaccine, which protects against a leading cause of meningitis.
Do these educational gains carry through into adult life?
Children who stay in school longer and achieve more tend to earn higher wages and enjoy better employment prospects as adults. So, do the gains associated with vaccination follow the same trajectory?
Evidence from Burkina Faso suggests they might. By exploiting differences in vaccination coverage across regions and birth cohorts, researchers were able to examine how early-life exposure to vaccination was associated with outcomes decades later.
In area with high vaccination coverage, school enrolment was around 10% higher, while primary school completion increased by about 13%.
Individuals from these areas were also around 7% more likely to enter formal, wage-paying employment as adults: a relatively small but important part of the labour market that offers greater security and protection.
The effects also appeared to extend beyond formal employment. In a country where most people work outside the formal economy, the team also examined agricultural productivity and found that vaccinated individuals produced around 6% more per hectare than their peers.

Crucially, this was not because they were using more land, labour or fertiliser. “A potential explanation is that their labour is just more efficient,” Kazianga says.
“If one person is protected against measles and another catches it but survives, and both go on to work as farmers, the one who has been healthier over their lifetime is likely to get more out of the same hour or day of work.”
Still, the relationship is not always straightforward. Labour market outcomes depend on many other factors, including gender norms, education systems and the availability of jobs.
“You might see strong effects on schooling, but those don’t always translate cleanly into labour market outcomes,” says Nandi. “A lot depends on what opportunities are available later in life.”
While direct evidence linking childhood vaccination to adult earnings remains limited, there is stronger evidence for the mechanisms that connect them. In a recent review, Ozawa found that a one standard deviation improvement in cognitive ability – equivalent to moving from average performance to roughly better than two-thirds of people – was associated with a 5% increase in wages.
“Although data are limited, if you have better cognitive ability, you tend to have higher school enrolment, academic achievement and educational attainment, and that tends to lead to higher wages,” Ozawa said.
Where are these effects on education strongest?
The benefits of vaccination are not evenly distributed. Across multiple studies, the gains in schooling and learning tend to be greatest among children from the poorest households: those who face the greatest burden of infectious disease to begin with.
In Bangladesh, for example, the impact of maternal tetanus vaccination on schooling was concentrated among children from the lowest socioeconomic groups.
The reasons may be both biological and social. Children growing up in poorer environments are more likely to experience repeated infections, undernutrition and limited access to healthcare, all of which can impair physical growth and cognitive development.
Preventing even a single episode of serious illness during this critical window can have lasting effects.
Vaccination may also help level the playing field in more indirect ways. In settings where school enrolment is not universal, parents may prioritise sending healthier children to school, while those who are frequently sick fall behind or drop out altogether.
On the flip side, a lack of access to vaccines can deepen existing inequalities. “Vaccine inequity creates a double disadvantage, where children who are the most likely to miss out on vaccines are often those who also already face significant barriers to education, economic mobility and family stability,” says Shet.
“That’s why, if they’re protected, they have that much more of an advantage. But if they're not, the inequity actually worsens.”
In this sense, vaccines are not just a health intervention, but a potential equaliser, one that can help narrow gaps in education and opportunity between richer and poorer children. “Vaccines play a big role in improving equity,” says Shet. “They’re an economic lever in that sense.”
This dynamic is not limited to low-income settings, she adds. As vaccine uptake declines in some high-income countries, similar patterns are beginning to emerge. “As hesitancy rises and uptake falls, we're seeing more outbreaks – for example, measles in the US. And it’s often the most disadvantaged communities who are hit hardest. We’re likely to see these inequalities play out more clearly as coverage declines.”
Have you read?
What does this mean for policymakers?
Taken together, the evidence suggests that vaccination does more than prevent illness: it shapes the foundations of human capital. By protecting children during critical periods of development, vaccines can influence not just survival, but learning, productivity and future earnings.
For policymakers, this has important implications. In many countries, spending on immunisation is still framed primarily as a health cost, rather than an investment. Yet studies like the one in Burkina Faso suggest that the returns may extend far beyond the health sector into education, labour markets and the wider economy.
That matters at a time when global health budgets are under pressure and vaccine hesitancy is rising in some parts of the world. If resources are limited, the priority is to invest in interventions that deliver the greatest overall benefit. “Vaccination is a huge return on investment,” says Kazianga.

Communicating these wider benefits may therefore be increasingly important. “When vaccine-preventable diseases fade from view, clinical messaging alone loses traction,” says Shet. “We need to speak to what parents hold closest: their child’s future. In our messaging, we need to link vaccination to learning and long-term success.”
The challenge is that many of these benefits unfold slowly and are difficult to measure. Unlike hospital admissions or deaths averted, improvements in learning, productivity or earnings may take years – even decades – to become visible. As a result, they are often overlooked in funding decisions.
Yet the broader picture is becoming harder to ignore. Vaccination is not just a tool for preventing disease, but one that helps create the conditions for children to thrive. “These diseases that we immunise against don’t just kill,” says Nandi. “Despite advances in medicine and improvements in water, sanitation and broader public health, even a single serious episode of disease can have an impact over your life course.
“That ‘over the life course’ element needs to be remembered when it comes to discussions about improving vaccination rates around the world. It’s going to have an impact on your schooling, on your learning, on your labour market outcomes. Infectious diseases have a much broader impact than just killing children.”