7 ways gender inequality still blocks access to life-saving vaccines
Ahead of International Women’s Day, we look at the structural inequalities that still prevent women and girls – and those they care for – from accessing immunisation.
- 4 March 2026
- 6 min read
- by Linda Geddes
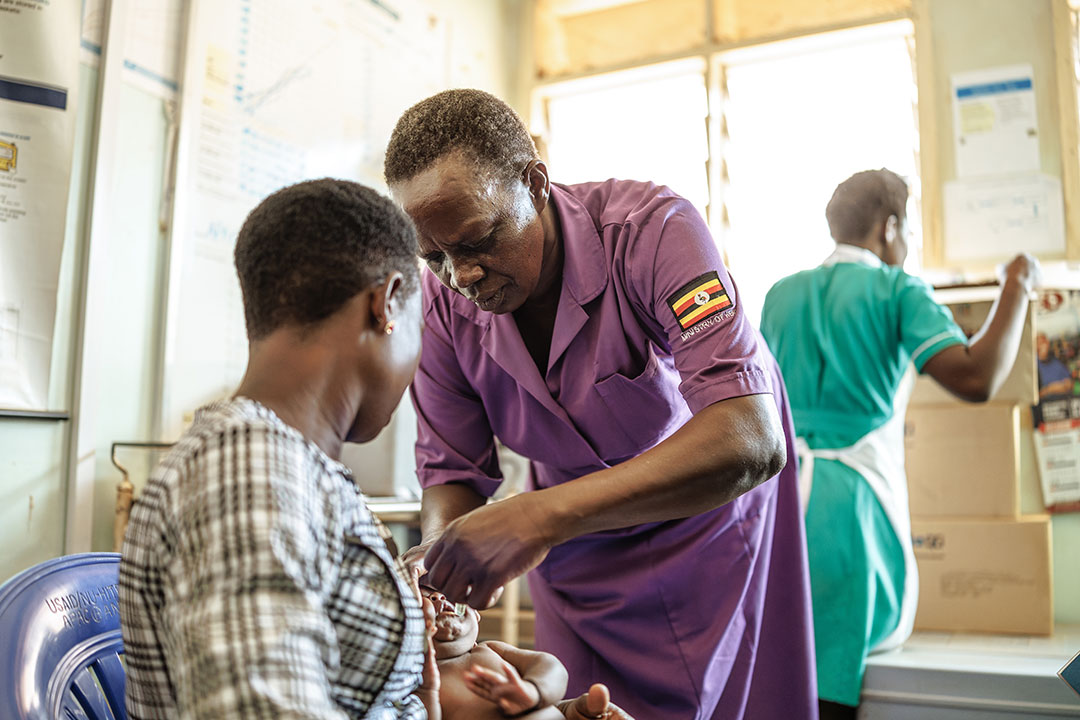
For many children, access to life-saving vaccines isn’t just a matter of supply, but whether the women in their lives have the time, money and freedom to reach them.
Around the world, the responsibility for getting children immunised typically rests on women’s shoulders, yet many lack the support, resources or autonomy to do so easily.
To mark International Women’s Day, we look at seven ways gender inequality is still shaping who gets vaccinated – and what is being done to change that.
1. Lack of information and awareness
Many caregivers may not have enough information about the importance and benefits of vaccines, making them less likely to seek vaccines out for their children. This awareness gap could be linked to limited access to health education or formal education, or communication strategies that fail to reach or resonate with caregivers.
Solutions: In many communities, trusted local health workers are helping to fill the information gap by bringing vaccine education directly to families.
For instance, in Liberia and Sierra Leone, where the malaria vaccine is being introduced, community health workers have been trained not just to deliver the vaccine, but to teach people about why it matters, who should get it and when vaccine teams will be visiting.
In Liberian communities where this malaria vaccine education is being provided, only 4% are reporting vaccine refusals.

Credit: Adeel Saeed
Meanwhile, in Sargodha, Pakistan, caregivers have been invited to see microbes under microscopes during community workshops, helping to link the bacteria they saw on everyday objects with the diseases that vaccines can prevent.
Afterwards, self-reported commitment to vaccination rose by 19 percentage points in the target group, and polio immunisation coverage hit 99%.
2. Division of household labour
In many families, caregiving and domestic responsibilities fall disproportionately on women.
Juggling childcare, household chores and in many cases income-earning work, they may have little time or flexibility to attend vaccination appointments – especially if other family members do not share or support these tasks. This makes missed appointments more likely.
Solutions: Engaging fathers more actively in health decisions can help rebalance this dynamic and improve vaccine uptake.

Credit: Edna Fleure
In Koukiri village in northern Benin, a ‘fathers’ club' is encouraging men to play a role in every aspect of child development – from nutrition to vaccination and medical follow-up. The initiative has reached more than 282 communities, directly impacting at least 3,000 households.
Similarly, in Akko in north-eastern Nigeria, a group of respected male community members have taken it upon themselves to speak with vaccine-sceptical fathers, helping to build trust and ensure more children are protected from infectious diseases.
3. Limited funds and financial access
Even where vaccines themselves are free, indirect costs, such as transport to the clinic and lost income, can pose substantial barriers to immunisation.
If women have limited access to or control over household finances, they may be unable to cover these costs, reducing their ability to travel to health facilities. This reinforces broader financial inequities and makes vaccine access dependent on family income dynamics rather than health needs.
Solutions: Tailored outreach and practical support can help close these gaps. In rural Leribe district, Lesotho, health workers discovered that a mother had stopped bringing her children for vaccination because she could not afford the small costs associated with clinic visits.

Credit: Pascalinah Kabi
Rather than leaving the family behind, frontline workers travelled to her home, vaccinated the children there, and helped provide the necessary medical booklets and basic support to reconnect the household with the health system.
4. Mobility and safety constraints
Travelling long distances can also be a major deterrent for many caregivers, particularly younger mothers. Safety concerns, remoteness and limited transport options sometimes intersect with gendered restrictions on movement, making it even harder for women to bring children for routine immunisation.
In communities with poor infrastructure – or where women are not allowed to travel alone – these barriers can delay or prevent timely vaccination altogether.
Safety challenges do not only affect caregivers. In some settings, female community health workers themselves face harassment, intimidation or unsafe working conditions – factors that can disrupt vaccination efforts and reduce coverage.
Solutions: Addressing safety for both caregivers and frontline workers is essential to ensuring vaccines reach every community. Bringing services closer to communities can also make a real difference.

Credits: Angeline Anyango
In Kenya’s northern Wajir County, mobile clinics travel to where nomadic families are living, helping overcome both distance and insecurity – including fears of attack or sexual violence that can make long journeys unsafe for women and children. In rural Liberia, volunteer vaccinators routinely travel long distances on foot or by motorcycle to reach remote settlements, often navigating difficult terrain and weather.
Meanwhile, in Djenné, Mali, where growing conflict and insecurity are affecting immunisation rates, health authorities have authorised trained community health workers to deliver vaccines within their own neighbourhoods, maintaining services even where travel to distant facilities is too dangerous.
5. Cultural restrictions on interactions between women and men
In some religious or cultural contexts, female caregivers may be reluctant, or feel unable, to seek immunisation services if they are delivered by male health workers.
Social norms governing interactions between women and men can complicate clinic visits, delay care or deter caregivers altogether, particularly in conservative or rural settings. When services are not delivered in culturally acceptable ways, access to vaccines can suffer.
Solutions: Expanding the role of trusted female health workers and community advocates can help bridge this gap.

Credit: Huma Khawar
For instance, in a culturally conservative part of northwestern Pakistan, female ‘bridge’ figures were recruited to connect families with health services, acting as culturally acceptable intermediaries and helping ensure children did not miss routine vaccinations.
In Kenya’s Masaailand, ‘guardian mothers’ have played a key role in promoting the HPV vaccine, using their respected status within communities to reassure families and counter misinformation. Similarly, in western Kenya, traditional birth attendants – long trusted by women during pregnancy and childbirth – have been trained to become vaccine champions, encouraging caregivers to complete immunisation schedules.
6. Long wait times and inconvenient clinic hours
Long wait times at clinics and restrictive opening hours disproportionately penalise caregivers who are also juggling paid and domestic work.
When clinics clash with work or household responsibilities, caregivers – especially women with limited scheduling flexibility – may be forced to delay or miss vaccinations for their children.
In Bengaluru, India, reporting by VaccinesWork has highlighted how rigid clinic schedules can make it especially difficult for poor, working mothers living on the city’s margins to keep up with routine immunisation.
When opening hours clash with daily wage work or long commutes, families may delay or miss appointments – illustrating how adapting services to the realities of caregivers’ lives is essential to closing coverage gaps.
Solutions: Adjusting vaccination clinic hours to better suit working parents can help to reduce this barrier.

Credit: JSI
In Port-au-Prince, Haiti, a Gavi-supported project introduced weekend clinic hours at 21 sites. At one clinic in Cité Soleil, the number of children receiving a third dose of the pentavalent vaccine has significantly increased, rising from 3,167 in 2017 to over 5,400 in 2023.
7. Negative attitudes from health providers
Caregivers may be discouraged from returning to clinics if they encounter disrespectful, dismissive or otherwise negative attitudes from staff.
The behaviour of health workers strongly influences caregivers’ trust and willingness to engage with health systems – particularly when mothers feel judged, blamed or unwelcome at clinics. When trust breaks down, follow-up visits and full immunisation schedules are more likely to be missed.
Solutions: Supportive, respectful care strengthens vaccine uptake and broader engagement with healthcare.

Credit: Anik Rana
For instance, in Nepal, a rigid male/female ID system initially prevented many transgender people from receiving the COVID-19 vaccine, until a local awareness campaign and cooperation from authorities helped remove documentation barriers and make vaccination more inclusive.
Another example comes from Lagos State in Nigeria, where HIV-positive mothers face stigma that could discourage them from seeking routine immunisation for their children. With support from trained ‘mentor mothers’, who provide counselling and accompany them to clinics, many women have overcome their fear of judgement and had their babies immunised.









