An anatomy of an outbreak: Measles hits urban India
Measles ripped through Thane, near Mumbai, after immunisation coverage dipped during the pandemic. VaccinesWork visited the city to hear about its devastating impact, as well as how social factors may have helped its spread.
- 28 April 2023
- 17 min read
- by Maya Prabhu
On her thirty-first day in the measles isolation ward at Rajiv Gandhi Medical College in Thane, Maharashtra, four-year old Saima was a tiny, hollowed-out form in her cot, breath gurgling rhythmically through the tracheostomy tube in her throat, eyes shuttling from her mother to her doctor and back. Someone had brought her a red balloon, and she held it scooped protectively in one arm.
“She’s better than previously,” said Dr Nishigandha Sonawane, the senior ward resident, as a neon-green “93” blinked encouragingly on Saima’s bedside oxygen monitor. “We’re planning to start feeds.”
This was what Sariful Nissa, Saima’s mother, had been waiting for. When she could finally feed her child, she said, she could begin to stop worrying.
“Measles is something we have a vaccine for since ages. It’s really sad, then, when we see that they’re not taking the vaccine. The vaccine was available.”
– Dr Shailaja Potdar, Associate Professor of Paediatrics at University Hospital, Thane
It had begun with a fever and “pimples” on the skin, said Saima’s father, Yahid Shah, a scrap labourer. Then the child’s jaw had seized shut, and that’s when they had brought her here, to this government-run tertiary care centre.
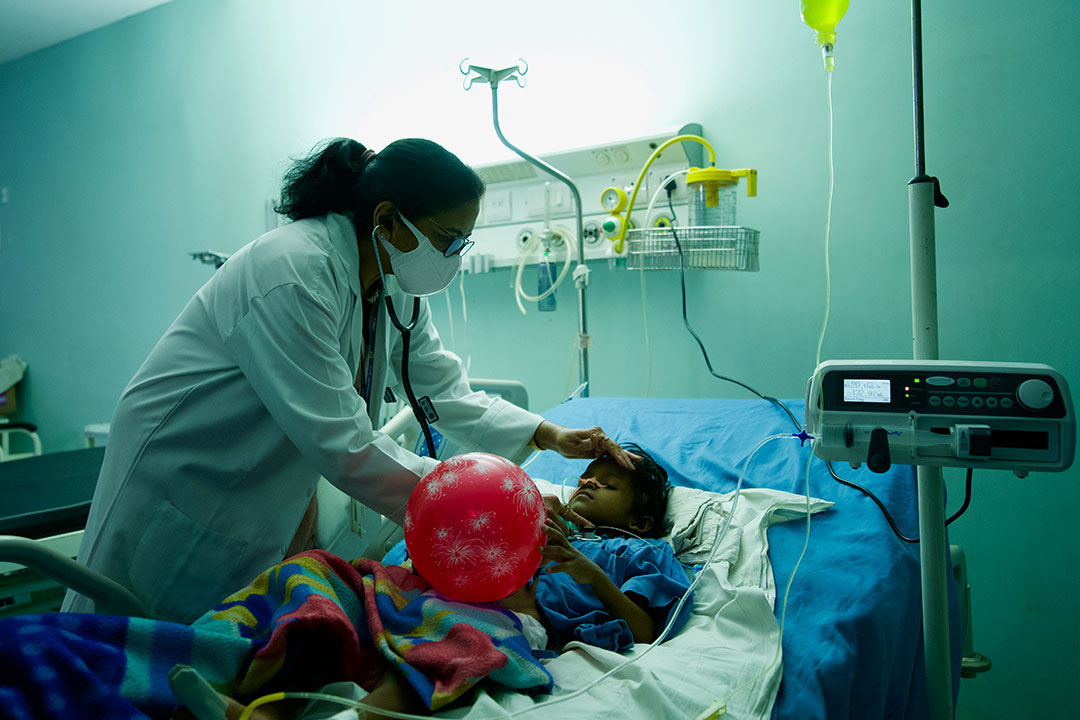
Credit: Gavi/2023/ Prakhar Deep Jain
“Initially, Saima had multiple episodes of spasm – she was not able to open her mouth,” Dr Sonawane explained. The “pimples” had been the tell-tale measles rash; the spasms were caused by tetanus, sometimes called lockjaw, a bacterial infection that had rooted and flourished in Saima’s body when her immune system was brought low by the measles virus. “We gave tetanus immunoglobulin, tetanus vaccine and antibiotics. After that, a tracheostomy was done, because of her ventilation, and she gradually started improving,” the doctor said.
Across the room, two other monitors glowed mutely, screens broadcasting the vital signs of their tubed-up charges: a whimpering one-year-old called Kanhaiya with a nasal cannula and a rough case of measles-associated bronchopneumonia, and 11-month-old Shahban, who came in feverish, suffering half-hour long convulsions. Now, Shahban was quiet – slack, in fact; dosed up on anti-epileptics, eyes like pale half-moons.
Much of the rest of the room was dark, beds stripped and stowed. This was mid-January, the ebb-tide of a major epidemic that had, in the busiest days of the December peak, seen the ward filled to capacity.
In the three months from late October, a total of 372 children were hospitalised with complications from measles across Thane. 177 of the sickest were treated here, several of them teetering for weeks on the critical brink. Two children, an almost-two-year-old boy and a six-year-old girl, died.
“In the past we have seen some scattered cases here and there,” said Professor Dr Vandana Kumavat, head of Paediatrics and a 28-year veteran of the department, “but never to such a magnitude.”
To the doctors, the outbreak was maddeningly avoidable.
"This child was unimmunised – unimmunised,” repeated Dr Kumavat at Saima’s bedside. She could have been speaking of any of the vast majority of measles cases she’d seen in the last months – 150 out of the 177 had been confirmed as totally immune-naive against measles. The remainder – many of whom had received just a first dose of the vaccine – had suffered “modified measles,” a less severe form, she said.
“In COVID times, what happened, because of lockdown, and because many facilities were fever OPDs – basically, they were treating fever cases – people were afraid of going to the health facility, and even there was a restriction of people coming together. So even though the immunisation sessions were carried out during lockdown, people were not ready to come to the vaccination site.”
– Dr Rani Shinde, Thane Municipal Corporation (TMC) Public Health Department
“The main problem was unimmunisation,” Dr Kumavat diagnosed, adding that malnutrition had been another common factor among the children sick enough to be admitted here. She described pleading with the families of the sick kids to go home and advocate for vaccination. “That is the most important message to be given to the society.”
“Measles is something we have a vaccine for since ages,” said her colleague Dr Shailaja Potdar, an associate professor of Paediatrics at the university hospital, who joined us in Dr Kumavat’s office. “It’s really sad, then, when we see that they’re not taking the vaccine. The vaccine was available,” she said, sounding angry, more than sad.
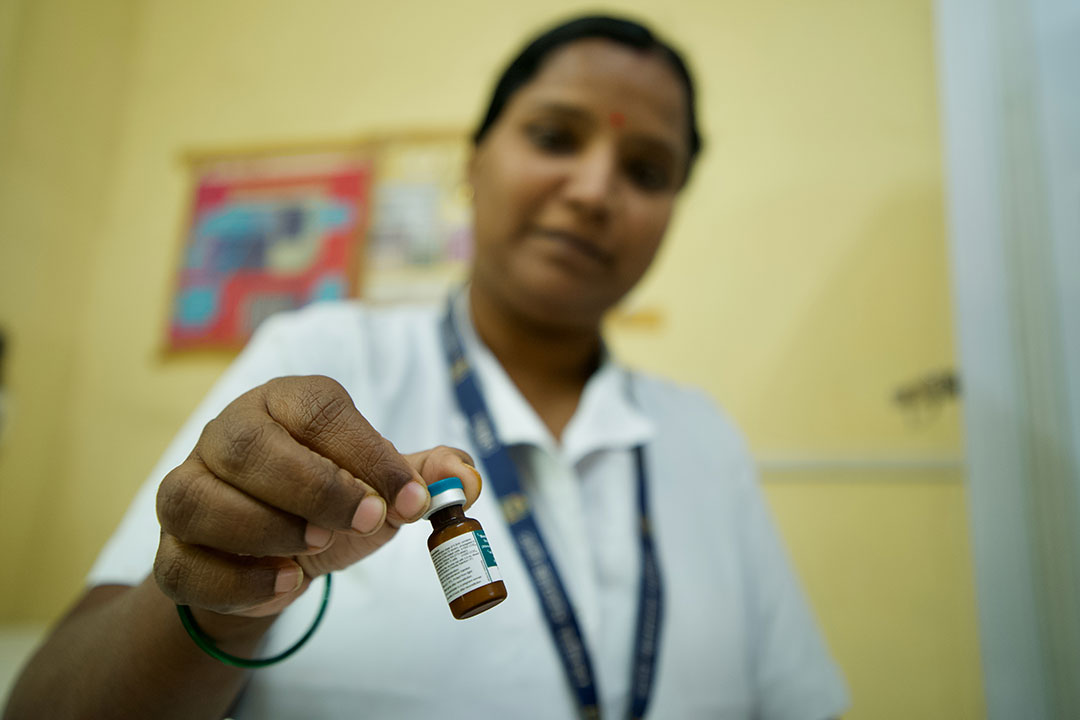
Credit: Gavi/2023/ Prakhar Deep Jain
*
If it was preventable (biomedically speaking, at least), the outbreak was also predictable. COVID-19’s shock arrival had dented routine immunisation coverage around the world, leaving tens of millions of children more vulnerable. “The consequences will be measured in lives,” warned UNICEF executive director Catherine Russell in mid-2022.
India’s immunisation system – the world’s biggest – had taken the largest hit in absolute terms. By 2021, coverage with the third dose of the basic diphtheria, tetanus and pertussis containing vaccines – a conventional indicator for vaccination coverage in general – was down 6% against 2019 levels, with the Indian cohort of missed children numbering an estimated 3.5 million, nearly 15% of the global total. An estimated 2.71 million, up from 1.38 million just two years earlier, were estimated to lack the protection of even a single vaccine.
Measles – the most infectious human virus we have – was bound to be the first vaccine-preventable disease to resurge. “From a disease-control point of view, we say, you know, measles will find communities that have low vaccination coverage, or susceptible persons,” measles expert Dr Peter Strebel told VaccinesWork when global measles incidence spiked 79% in the spring of 2022.
“Our outbreak, it came on 28th of October,” said Dr Rani Shinde of the Thane Municipal Corporation (TMC) Public Health department. As the programme lead for Reproductive and Child Health, Dr Shinde oversees routine immunisation for Thane area. When we visited her in her office at the TMC headquarters, a colossal, superficially dilapidated building, she was also coordinating the city’s outbreak response campaign.
In just two months, more than 80,000 doses of MR vaccine – “whether MR1, MR2 or additional dose” – had been administered, and it was working. New reports of fever-rash cases were slowing to a crawl.
Thane is a public health challenge: massive, dense, mobile, and swatched with poor informal settlements. India’s 2011 census pegged Thane district as India’s most populous, and today the city is a still-burgeoning commuter town, drawing more migrants than Mumbai proper.
But drive to Thane from Mumbai – along the Eastern Express highway, past rectangular concrete tower-blocks sprouting gridded out of marshy ground, as if, long ago, someone forgetful had planted a server farm in a swamp – and you’re unlikely to notice that you ever left one metropolis and entered another. In life and economics, the cities blur.
Mumbai was hit first. “When we got this news of Mumbai having cases of measles in particularly one area, and deaths of children in that area, that was a very alarming situation for us,” recalled Dr Shinde. Thane braced. “Our target was, like, we don’t want any single death in Thane. That was our target. Our honourable Commissioner-sir also committed for the same.”

Credit: Gavi/2023/ Prakhar Deep Jain
One hundred and fifty two-person health teams, pulled from now less pressing COVID-duty, scrambled across the city, knocking on doors, looking for ‘fever-rash cases’. “We said, if the cases come, we will manage those cases wholeheartedly,” Dr Shinde recalls. The cases came: in the period from 19 November to mid-January, 1,294 suspected measles patients were discovered in the outbreak zone and brought into care. She tapped at the number on a print-out with one finger. “This is the achievement of the field teams,” she said.
“We had two deaths in Thane,” she acknowledged, rueful. “But we tried a lot.”
In Thane, as elsewhere, the immunisation safety net had taken critical damage in the previous couple of years. “In COVID times, what happened, because of lockdown, and because many facilities were fever OPDs – basically, they were treating fever cases – people were afraid of going to the health facility, and even there was a restriction of people coming together. So even though the immunisation sessions were carried out during lockdown, people were not ready to come to the vaccination site,” she said.
The arrival of COVID vaccines eased social anxiety, but the campaign to administer them occupied the time and attention of an already stressed health system. Overall, said Dr Shinde, routine immunisation became “a little bit an ignored thing”.
“Now we have seen this measles outbreak, might be we see other infectious diseases,” the paediatrician had warned, over tea in her office. “Diphtheria, pertussis. We had seen couple of cases of tetanus because people had not taken vaccines. We have to be watchful.”
– Dr Vandana Kumavat, Head of Paediatrics, Rajiv Gandhi Medical College
But more recently, the city at large had made committed strides to patching up its immunity gaps. Most parts of town were pretty much caught up before the outbreak hit, Dr Shinde thinks. But a few critical pockets had proved resistant to the health department’s efforts.
“The outbreak which we are seeing, we are seeing in a particular area, where there are certain communal differences,” Dr Shinde explained, cautiously. “There are certain faiths that particular communities are having in those areas. Even if we go routine-wise also, coverage of vaccination is also less there. And in COVID times it [the immunisation gap] has built up more – so outbreaks started in particularly that area.”
The area in question is Mumbra, or Mumbra-Kausa if you want to narrow in on the epicentre, an informally settled Muslim-majority enclave of a Muslim-minority state.
Even before the pandemic, Mumbra had a reputation for vaccine hesitancy. During a 2018 measles-rubella vaccination campaign, Dr Shinde told me, most of Thane had achieved 90% coverage, while Mumbra lagged at a vulnerable 40%.

Credit: Gavi/2023/ Prakhar Deep Jain
Part of the difficulty is the transience of the population, which includes large numbers of poor migrants from other states. In Mumbra’s ramshackle tenements, neighbours might not know their neighbours; might not know, for instance, when a community health worker comes knocking, that the lady next door has recently delivered a baby. Strong social ties, Dr Shinde explained, enable community health work. Floating populations are slippery.
Another portion has to do with access. Due to planning complications – land is scarce, and most of Mumbra is “unofficial” – there are fewer health centres here than there ought to be to service a population of this size. Moreover, the public health department has had a hard time recruiting locals as ASHA workers, India’s all-important female community health frontliners. Dr Shinde says that’s down to cultural ‘habits’. Muslim women, she says, are more likely to be wanted at home than their Hindu counterparts.
But what’s also plain is that a dangerous trust deficit has grown up between the Mumbra communities and the state organs of health.
“We will go deep inside Mumbra; I think it’s important,” said Dr Shinde, as we sped along Thane Creek in her official vehicle, a little bread-tin van. By now, the TMC was embarking on the third month of its colossal outbreak response vaccination campaign, and Dr Shinde – cheerful, pragmatic, almost intimidatingly capable – was pulling out all the stops to get Mumbra covered.
Two maulanas had been drafted in to broadcast the importance of vaccination at Friday prayers; the TMC’s honourable Commissioner himself – a senior Indian Administrative Service figure named Abhijit Bangar, by all accounts a valued and committed comrade in the fight against the epidemic – had turned up at meetings to underscore the city’s commitment to Mumbra’s corporators. (“If honourable Commissioner is in the field, it creates a different impact,” Dr Shinde observed).

Credit: Gavi/2023/ Prakhar Deep Jain
She showed me a WhatsApp group she’d created called “Mission Kick to Measles!” which made Dr Shinde – who sits high in an anonymisingly large pyramid of health workers – directly available to field staff in outbreak zone. Google Docs had been built for real-time data collation, a means of leapfrogging creaky official reporting mechanisms. "People are very well motivated,” she said “that sense of vaccinating each and every child has come up again. I’m optimistic about that.”
In just two months, more than 80,000 doses of MR vaccine – “whether MR1, MR2 or additional dose” – had been administered, and it was working. New reports of fever-rash cases were slowing to a crawl, just one or two a day now, and, as I’d seen myself a day earlier, the emergency measles isolation ward was moving in the hopeful direction of redundancy.
Have you read?
But while Dr Shinde felt confident enough to declare the outbreak “under control”, Mumbra-Kausa remained a perplexing concern. “The thing which bothers me as a professional looking after this programme, is that still the cases that are coming are coming from particularly that area only,” she said. “There are refusals, though we are going and explaining to them twice, thrice. Somehow we are not able to achieve 100% vaccination coverage in that area.”
“We need to know what is that thing that is holding them back. Even I, as a programme officer, I don’t understand exactly what that fact is.”

Credit: Gavi/2023/ Prakhar Deep Jain
Kausa Health Centre is small – a simple two-story building, dwarfed by Jenga-tower tenement blocks with pelts of grass sprouting from unplastered and unconvincing concrete seams.
According to Dr Hemangi Ghode, health centre in-charge, her staff serves a population of 162,207 people, and sees more than 200 outpatients a day. This was antenatal care day, and on the ground floor, a queue of pregnant women snaked past a long queue for the tuberculosis drug dispensary.
Upstairs, Neeta Kadam, General Nurse Midwife (GNM), was in the refrigerator room, sorting out vaccine stocks. Kadam consulted her ledger: that morning, she’d sent out 85 doses of MR vaccine with six different outreach teams.
Whether those doses would all get used was a question that elicited a twinkling smile. “In this area, whatever vaccine you want to introduce, it’s difficult,” she said. The most common, obstructive rumour, she said, was that vaccines caused infertility – that they were designed to “stop the community from growing.”

Credit: Gavi/2023/ Prakhar Deep Jain
We drove out to a vaccination session, this one pitched up in the front yard of a Kausa corporator’s home. The morning so far had been slow going, said ANM Vaishali Khiran: “You might expect eight, but fewer will come.” Mithali Nilekar, ASHA worker, smiling mildly, explained, “They don’t take vaccines. They say kids die of vaccination.” She regularly tried to correct that misconception, describing how vaccines produce protective immunity, but reactions were mixed. “Some believe me, some don’t,” she said.
The next parent to arrive was Saira Azmer Unissa, 32, a native of Uttar Pradesh, a northern state, who had been “mobilised”, it turned out, unnecessarily: her ‘Mother Card’ confirmed that her children were up-to-date on their vaccines.
Before she left, she sat down in the shade for a moment, and fell into friendly conversation with Dr Shinde, who promptly attempted to recruit her to the ASHA ranks. Unissa laughed – far from home and with five children, she had barely enough time as it was. And besides – she hoped to move out of Mumbra-Kausa. Her place here was tiny, she said, and the water regularly cut out.
Imam Uddin Shah, 27, a private tutor, betrayed by his dazzled smile that his two-month-old baby, Hamza, was his first. He shushed the boy gently when the needle prick made him cry.
Shah was bringing him for his vaccines, he said, “because you should keep faith in the government.” Faith in the government, it appeared, translated to faith in vaccination.

Credit: Gavi/2023/ Prakhar Deep Jain
Masira Shaikh suggested the inverse might also be true. She had heard of the outbreak and had brought in her one-and-a-half-year-old son for his second MR shot. She’d been putting it off: the boy had run a fever for three days after his first dose, and it had made her a tiny bit nervous. Meantime, around her, suspicion of vaccines had seemed to be growing – for the past couple of years she’d heard rumours of Trojan Horse population control campaigns.
“It’s due to such… cold wars… between the communities,” she said, searching a while for an apt English phrase.
*
The population-control myth cropped up again when we visited a so-called “refusal family” in a rough cement tower block close to the vaccination outpost. Dr Shinde knocked, and Irshad Khan, 36, a retail worker, answered. His wife Dinaz stood with him in the doorway of their single-room home. Behind them, baby Usman lay on the bed, giggling adorably to himself.
The other children were vaccinated, Dinaz said, but to Usman, “we didn’t give it because we were scared”. Irshad had heard in the market and on WhatsApp that the child would be rendered infertile.

Credit: Gavi/2023/ Prakhar Deep Jain
Dr Shinde spoke warmly and fast: “You didn’t give it because you were scared. But I would like to tell you that we get the vaccines from the Government of India. We give the same vaccine to everyone. It is not like a different one is being sent to Mumbra or Panch Pakhadi in Thane. The same vaccine comes everywhere. It would be so difficult to make different vaccines for different people!”
She told them about her own children, four-year-old twins. “Why do I want to vaccinate my children?” she asked herself, since Dinaz and Irshad seemed uninclined to. “If they contract the disease it will ruin their lives!” She told them about scientific studies, about the World Health Organization and its recommendations, warned them to be wary of nonsense WhatsApp rumours.
As we left, she seemed deflated. “We can’t always say so many things,” she said. “Fifteen minutes we spent – and though he is saying he will come, I’m not sure that he will.” To her, mistrust in the health system seemed to be a straightforward vote for danger over safety. When it came to her own children, she’d tell me later, she placed her trust in the treating doctor as if she was a layperson, and not a physician herself. Is that too much to ask? She seemed to mean.
But in recent years, India’s large Muslim minority has found itself increasingly marginalised. In Mumbra-Kausa, troubled national currents felt very close to the surface. “It’s like an underbelly” a Hindu resident of Mumbai had said, when I mentioned I was going to Mumbra; elsewhere in Thane, the words “they” and “them” seemed to stalk conversation about the neighbourhood.
In a 2015 profile for national newspaper the Hindu, writer Basharat Peer identified it as India’s largest Muslim ghetto, and traced its traumatic origins. “The Bombay riots of December 1992, which overwhelmingly killed Bombay Muslims, and the retaliatory bomb blasts in January 1993 by the Muslim underworld, reconfigured the social geography of the city,” he writes. Overnight, Mumbra, a safeish distance from the conflict and at that point a settlement of just 45,000 mostly-Muslim people, ballooned. By the 2011 census, its population was nearer a million – a city in itself, built in a flinch from majoritarian violence.
It seemed clear to me, in other words, that the infertility myth was an irrational articulation of a deeper, understandable sense of insecurity.

Credit: Gavi/2023/ Prakhar Deep Jain
The tragedy is the irony: the self-protective anti-vaccine myth finally negates life.
Arhad Khan, from Kausa, was not yet two when he fell ill in mid-November. His breathing became troubled, but his family was wary of government clinics – as they had reportedly been wary of vaccination – and said they preferred to wait for a private doctor to see him. He grew precipitously sicker.
On 23 November, after a great deal of convincing, according to Dr Hemangi Ghode, and too late, according to Dr Vandana Kumavat, he was admitted to Rajiv Gandhi Medical College hospital, where he was intubated. On November 27, he died with measles-linked bronchopneumonia, septicaemia and Acute Respiratory Distress Syndrome (ARDS).
His grandmother, Rakhiya, said he had been a playful, restless, bright, boy, disinclined to sit still in laps, transfixed by football. He could kick a ball all the way to the end of the corridor – she gestured down the dim common hallway – and he already knew his whole alphabet.
Rakhiya stood wedged between the door of her home and the door-frame, blocking entry, telegraphing wariness. Later, Dr Ghode and Dr Shinde told me they suspected she was shielding other children inside from view of the health workers.
The conversation grew tense. “Can you bring back my child?” Rakhiya asked angrily, at one point. It appeared she regretted his admission to hospital, believing it had worsened his chances.
The implied accusation bruised Dr Shinde, who was downcast on the drive back to central Thane, murmuring stormily about “bullshit doubts”. “These things are discouraging one,” she said. “I understand her feelings – but things were done in good faith to help her out.”
She was worried, of course, that the doubt could spread. Mistrust, unlike measles, is difficult to inoculate against.
She rallied. “Something inside me says – no, these are poor people. You have to work with dedication,” she said.
Credit: Gavi/2023/ Prakhar Deep Jain
A few days later, I received an update from Dr Kumavat on my phone. “Saima Shah 4 yr case of Tetanus with measles is much better,” she wrote. “We have started oral feeds.”
A week and a half after that, another message landed. It was a picture of Saima: slight, serious-faced, but standing on her own two feet, a large sticking plaster where the tracheostomy tube had been. “Saima discharged last week,” read an accompanying message.

Credit: Vandana Kumavat

Credit: Vandana Kumavat
This outbreak was over. The risk of another remained. “Now we have seen this measles outbreak, might be we see other infectious diseases,” the paediatrician had warned, over tea in her office. “Diphtheria, pertussis. We had seen couple of cases of tetanus because people had not taken vaccines. We have to be watchful.”









