Pneumococcal vaccine is saving lives already

Mwai Kibaki
President of the republic of Kenya
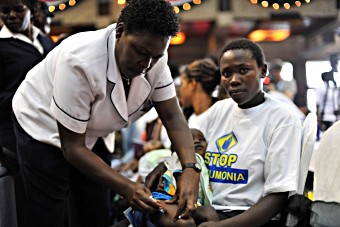
Mary Wambui looks on as a nurse delivers the first of three pneumococcal vaccine doses to her daughter Esther Nyambura in February 2011. The scene will be repeated countless times in health clinics across the country, as Kenya targets 85% pneumococcal vaccine coverage by 2012.
From the mountains and forests of western Kenya through the savannah grasslands and down to the sea, Kenyan parents can now protect their children against pneumonia, the biggest killer of children.
Introduced to Kenya earlier this year, a new vaccine to prevent pneumococcal disease, the leading cause of pneumonia, is reaching all corners of our country and should be available for 85% of Kenyan infants by the end of 2011.
The first country in Africa and one of 15 countries to have introduced the pneumococcal vaccine already, Kenya is immensely proud to be part of the fight against pneumonia. This new vaccine could eventually save 7 million lives by 2030.
The life-saving power of immunisation is remarkable enough, but the accelerated time frame for this vaccine is truly outstanding. In the past, it took up to a decade for life-saving vaccines to reach countries such as Kenya.
But this time the pneumococcal vaccine reached Kenya faster than ever before.
The GAVI Alliance is a broad coalition of partners including WHO, UNICEF, and the World Bank that was set up in 2000 to save lives and protect health by increasing access to immunisation. Everybody should know this name.
By concluding long-term supply agreements with the manufacturers of pneumococcal vaccine at a ceiling price, GAVI helped reduced market uncertainty and encouraged manufacturers to develop their production capacity and supply at lower cost.
Kenya may have been one of the first developing countries to receive this vaccine. But it is not the only one.
In the past year alone, 14 other countries from Nicaragua through to Yemen have also received the pneumococcal vaccine. And by 2015, GAVI expects that nearly 60 countries will have introduced this vaccine into their routine immunisation systems to protect millions of childrens.
Roughly 98.5% of pneumonia deaths occur in less developed countries, where physical isolation or political instability can mean medical care is hard to reach. But by preventing disease in the first place, immunisation removes the need for prompt hospitalisation or medical treatment.
The pneumococcal vaccine prevents more than pneumonia, though, protecting against pneumococcal meningitis too. In this way, it protects the health of the roughly one quarter of African children who, having survived pneumococcal meningitis, face lifelong disabilities such as deafness, seizures, or mental retardation.
To be clear, immunisation is not the only way to prevent pneumonia. Breast-feeding, improved nutrition, the reduction of indoor air pollution and antibiotics are important interventions too.
And there’s still a long way to go before this vaccine reaches millions more children around the world.
But the introduction of the pneumococcal vaccine in our country means Kenya is now on the wide, straight path towards reducing unnecessary child mortality and protecting the health of our country’s children.
