Nearly a month after the World Health Organization (WHO) declared novel coronavirus a global pandemic, Ethiopia declared a state of emergency, when the country recorded 55 confirmed COVID-19 cases and 2 deaths. The government refrained from sending the country into lockdown in an effort to preserve the country’s economy. Since August, the government has been debating lifting the state of emergency or temporarily extending it for a further three months. Recently, an 80% spike in COVID-19 cases over a span of 12 hours was recorded, which was attributed to the testing campaign launched in early August, which aims to conduct 200,000 tests. In the first week of September, the number of confirmed cases in Ethiopia grew by 15.7% compared to 2.2% in Nigeria, 16.1% in India and 5% in the United States of America.
In addition to the COVID-19 pandemic, Ethiopia is also grappling with cholera and yellow fever outbreaks. According to a Ministry of Health (MoH) update, there was a 14% decline in pentavalent and measles-containing-vaccine first-dose (MCV1) coverage from January 2020 to April 2020. The decline in coverage in the first quarter of 2020 could be attributed to the reduced number of outreach sessions and demand for immunisation – primarily driven by restriction of movement; fear of contracting the virus; and shortage of personal protective equipment (PPE) for health workers. Following intense sensitisation efforts by the MoH, service uptake resumed in the second quarter. However, human papillomavirus (HPV) vaccine second-dose vaccination was postponed to October 2020 due to school closures.
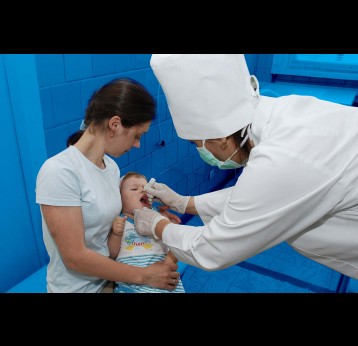
Each vaccination team had six members, including a health worker assigned to carry out COVID-19 screening and education.
A measles follow-up campaign, targeting 14.9 million children aged 9 months – 5 years, was initially planned for April but was postponed in light of the pandemic. However, following a National Immunization Technical Advisory Group (NITAG) recommendation that the measles follow-up campaign should be conducted, the MoH launched the campaign on 30 June under WHO’s pandemic guidance, and it has now been completed. The supplementary immunisation activities were done over 10 days to limit crowds and comply with COVID-19 protection measures. Each vaccination team had six members, including a health worker assigned to carry out COVID-19 screening and education. Reports indicate that, overall, the campaign was successful, with provisional results showing more than 90% coverage. The success was attributed to some key interventions, including, the availability of PPE and infection prevention and control (IPC), school closures and other COVID-19 precautions, strong social mobilisation activities, the proximity of vaccination sites to the communities and, in some places, the use of mobile teams and extended campaign implementation days. Though overall the campaign was successful, it was not without challenges. Mass political protests erupted the week the measles follow-up campaign was launched, following the murder of a popular singer. This affected four regions: Addis Ababa, Oromia, Dire Dawa and Harari; where the campaign resumed only once the security situation had stabilised.
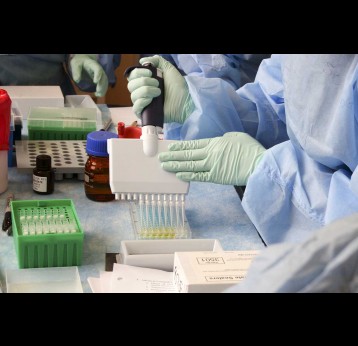
In addition to ensuring minimal disruption to health services such as immunisation services, the government has been focused on the broader COVID-19 response. The response focusses on strengthening community surveillance to improve case-finding, expanding laboratory capacity for testing samples, improving the quality of care at quarantine centres, following a reduction in the quarantine period from 14 to 7 days and incentivising local production of items such as PPE to prevent supply shortages.
Read the full 8 September situation report here.
Related content
Scientists around the world are working faster than ever to develop and produce vaccines that can stop the spread of COVID-19, with 21 vaccines now being rolled out in countries worldwide. Here is an at-a-glance overview of those vaccines and…
Taking the long view on vaccine markets
Gavi’s long-term approach to developing healthy markets for critical vaccines has led to greater stability and security, providing countries with the confidence that supplies will be available to meet their demand.
2019 was a landmark year for countries co-financing their vaccine programmes
In 2019, a higher share of Gavi-supported countries than ever before met their co-financing obligations on time, thanks to strong political commitment.
Strong systems for strong vaccine coverage
In 2019, countries delivered more than 230 million routine vaccinations, a record number, supported by unprecedented levels of health system funding from Gavi to support immunisation and protect the most vulnerable children. Here is what Gavi did…
The goal of our market shaping work is to help ensure vaccine markets work better for lower-income countries. We want the maximum number of people to receive the life-saving and health-protecting benefits of immunisation.
Experimental approaches to address post-transition risks
After transitioning out of Gavi support in 2017, the Republic of Moldova is mobilising champions and advocates to strengthen vaccine confidence – which is crucial to the success and sustainability of immunisation programmes.
Typhoid: immunising against antimicrobial resistance
Typhoid fever is increasingly resistant to the main antibiotics used to treat it. Gavi is supporting a new vaccine to help control this deadly disease – and fight antimicrobial resistance.
Gavi at UNGA: Global solidarity to defeat COVID-19 and create a better world for all
September 2020 marks the 75th anniversary of the United Nations General Assembly (UNGA). This year, the focus of the high-level General Debate is the importance of effective multilateralism.
Leaders in the fight against infectious diseases
Snapshots from DRC, India and Zambia illustrate country ownership and progress in the fights against Ebola, polio and HPV.
How health systems work and why they matter
Supporting health systems is essential for Gavi’s work to improve immunisation coverage and equity.
COVID-19 vaccines: what happens after clinical trials
If a COVID-19 vaccine is to reach the global public sometime next year, it will be the result of one of the fastest developments and rollouts of a vaccine against a new disease ever. In contrast, the RTS,S malaria vaccine, which is currently…
How Ethiopia is maintaining health services during a pandemic?
Ethiopia has overtaken Nigeria to become the Gavi-eligible African country most affected by COVID-19. Over the past week, the number of confirmed cases in Ethiopia has grown exponentially. Despite the pandemic, immunisation activities – both…