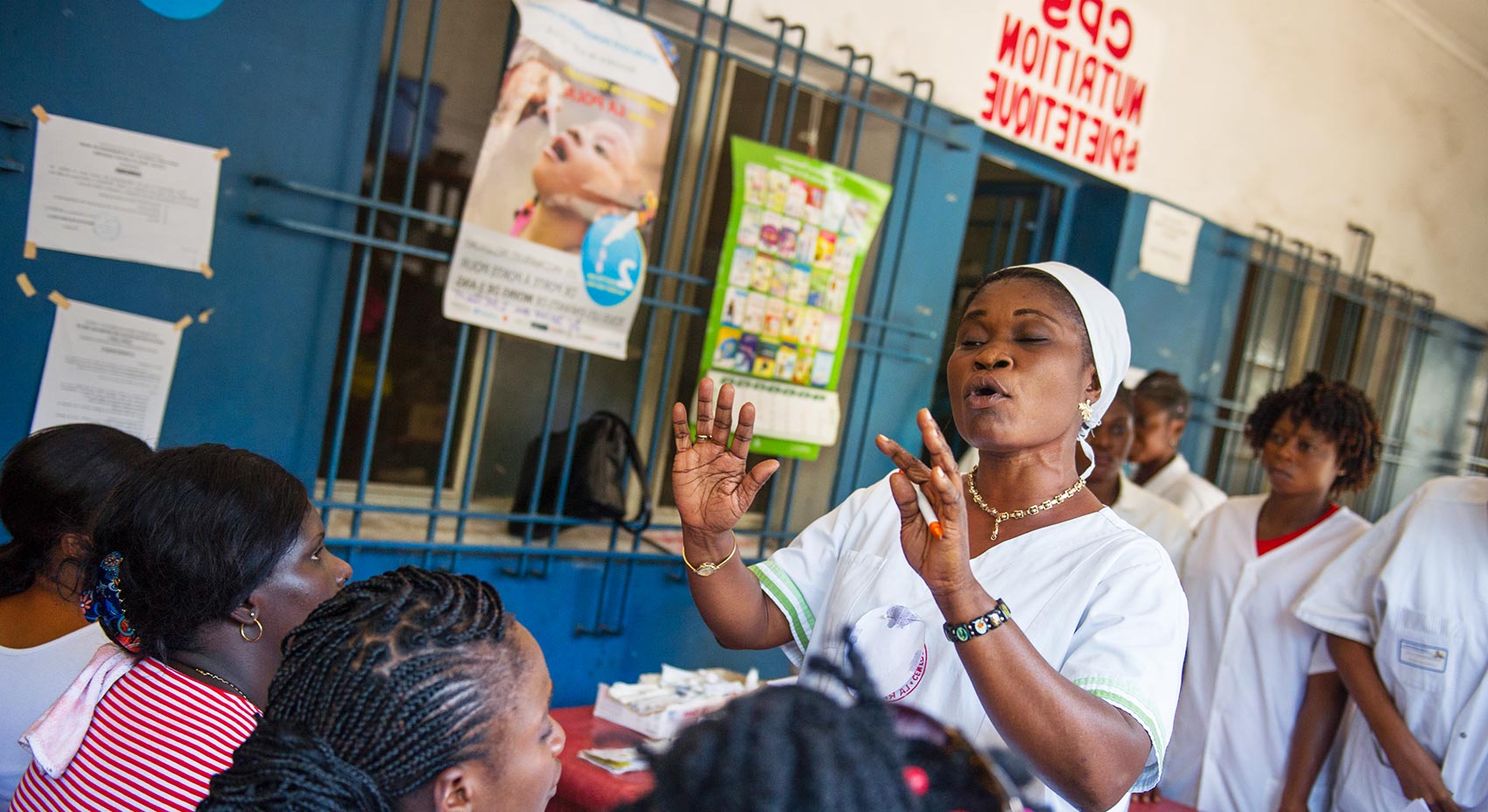The Democratic Republic of the Congo (DRC) is a country the size of Western Europe, riven by difficult terrain and crumbling infrastructure after decades of war and continuing conflict in the east of the country.
Despite these huge challenges, its immunisation programme has achieved impressive progress over the past two decades, increasing basic vaccine coverage and almost halving child mortality over the same period.
Yet this progress hasn’t been universal. A major 2018 cluster survey revealed a country divided. In North Kivu an impressive 79% of children were fully immunised, compared with just 7% in Maniema. To get a clearer idea of why this was happening at a local level, in early 2018 Gavi initiated work to gather and analyse this subnational data.
The results gave a clear picture of what was driving this underperformance. Only 10% of districts nationwide went through 2017 without experiencing a stock-out of vaccines. Even within health zones there were huge disparities in terms of service availability: in the capital, Kinshasa, there were fifteen times more immunisation sessions in one district than in another just a few kilometres away.
Despite the numerous challenges exposed by this new analysis, DRC had one important trump card: a strong, well-staffed Ministry of Health with the political capital and will to turn the country’s routine immunisation programme around.
It also had partners ready and willing to support this effort. Gavi, working alongside Alliance and expanded partners, spent the summer of 2018 working with the Ministry of Health and other partners to devise a plan that would complement current performance-based health sector reforms and address the structural issues holding back DRC’s routine vaccination programme, focusing on the provinces that were found to be furthest behind.
Frequent disease outbreaks had diverted attention away from routine immunisation – the first and best line of defence against outbreaks – towards reactive campaigns. The new plan’s underlying vision would be to put routine immunisation back at centre stage, framed with the message ‘Routine is the new emergency!’
In October 2018, Gavi’s Deputy CEO Anuradha Gupta joined DRC Health Minister, Dr Oly Kalenga, in Kinshasa to launch the Mashako Plan, named after former DRC Minister of Health, Professor Leonard Mashako Mamba, who approved the introduction of the first Gavi-supported vaccine back in 2001.
The plan is ambitious – to boost national vaccine coverage by 15 percentage points within 18 months, protecting 220,000 additional children. But it has a clear target population of nine vulnerable provinces and achievable objectives, including a 20% increase in the number of immunisation sessions and an 80% reduction in vaccine stockouts.
The plan also includes several innovations to boost coverage, such as performance-based funding and the use of smartphones to aggregate data and target low-performance areas. Regular coverage surveys will ensure the plan stays on track. Gavi’s Cold Chain Equipment Optimisation Platform is aiming to increase the proportion of health areas with working cold chain equipment, from just 16% in 2016 to a target of 80% by the end of 2019.
It’s difficult to underestimate the challenges of improving routine immunisation coverage in a fragile country the size of DRC. But by drilling down into the data, hunting out the gaps in coverage and targeting them ruthlessly, the Mashako Plan could prove to be a workable model for boosting the number of children receiving routine vaccines in even the most difficult of settings.
A world first: the Ebola vaccine passes its first major test
While the government was poised to label routine immunisation as the new emergency, a more familiar health emergency was brewing in northern DRC. In May 2018 an Ebola outbreak was declared in Equateur province.
This was DRC’s ninth Ebola outbreak since the disease was discovered, but it was the first to include a potentially powerful new weapon in the response effort: a vaccine. Nearly 3,500 people at risk received the vaccine during the outbreak, which was declared over in late July.
The stockpile of Ebola vaccines, which is yet to be licensed, was available thanks to a unique agreement between Gavi and the vaccine’s manufacturer, whereby Gavi committed to procure future doses of licensed vaccines when they become available.
In return the manufacturer committed to apply for licensure to a stringent health authority and in the meantime to ensure a stockpile of at least 300,000 investigational doses would be available in the event of an outbreak.
Sadly, this stockpile would be needed again just a month later. On 1 August another outbreak was declared in North Kivu, a region torn apart by instability, conflict and mistrust of the government. This outbreak would prove far tougher to contain and control.