Gavi diagnostic support
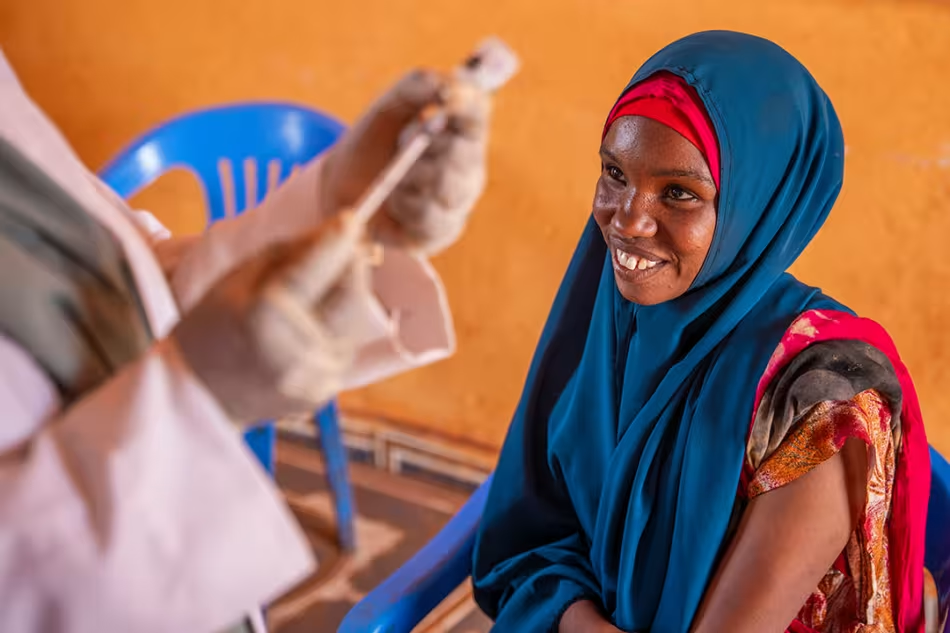
Gavi diagnostic support
Gavi supports countries with relevant diagnostics to improve targeting for yellow fever and cholera vaccines, while also ensuring that fit-for-purpose tests are available for measles and rubella, meningococcal meningitis and typhoid fever.

Vaccine information
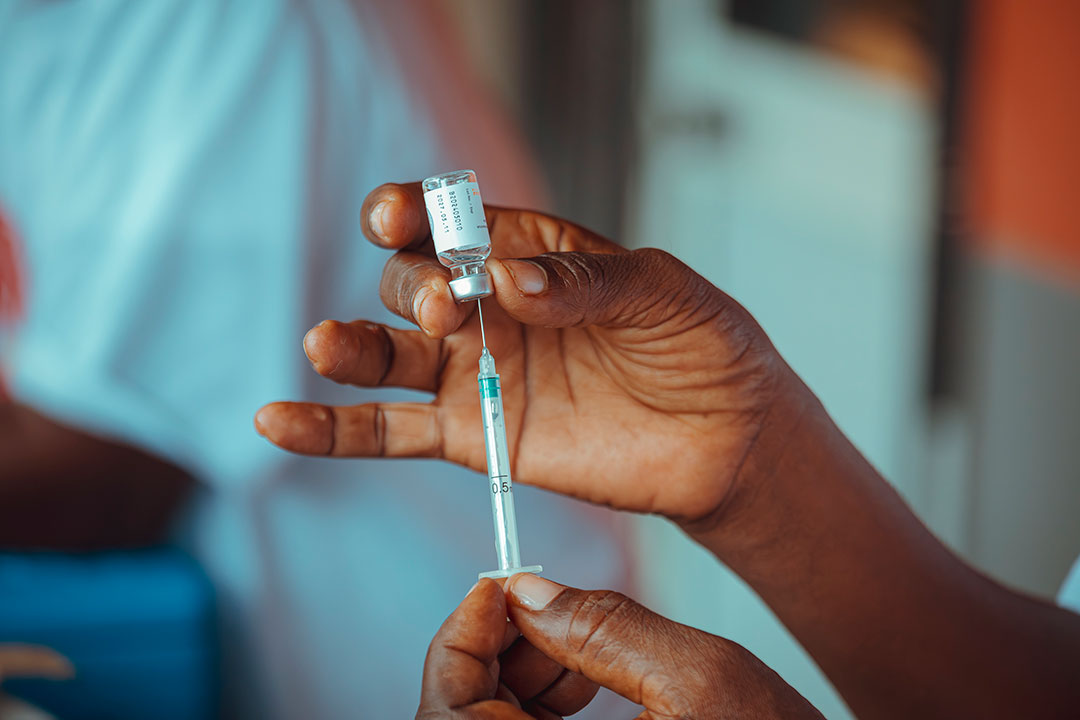
Vaccine information
Fact-based, accurate and accessible vaccine information from Gavi’s VaccinesWork platform and from our Vaccine Alliance partners.