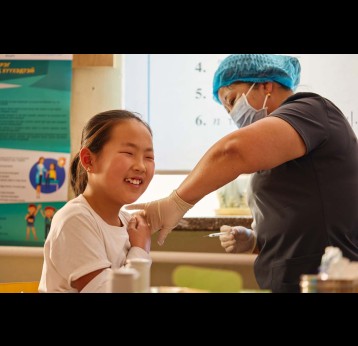
Gavi’s impact
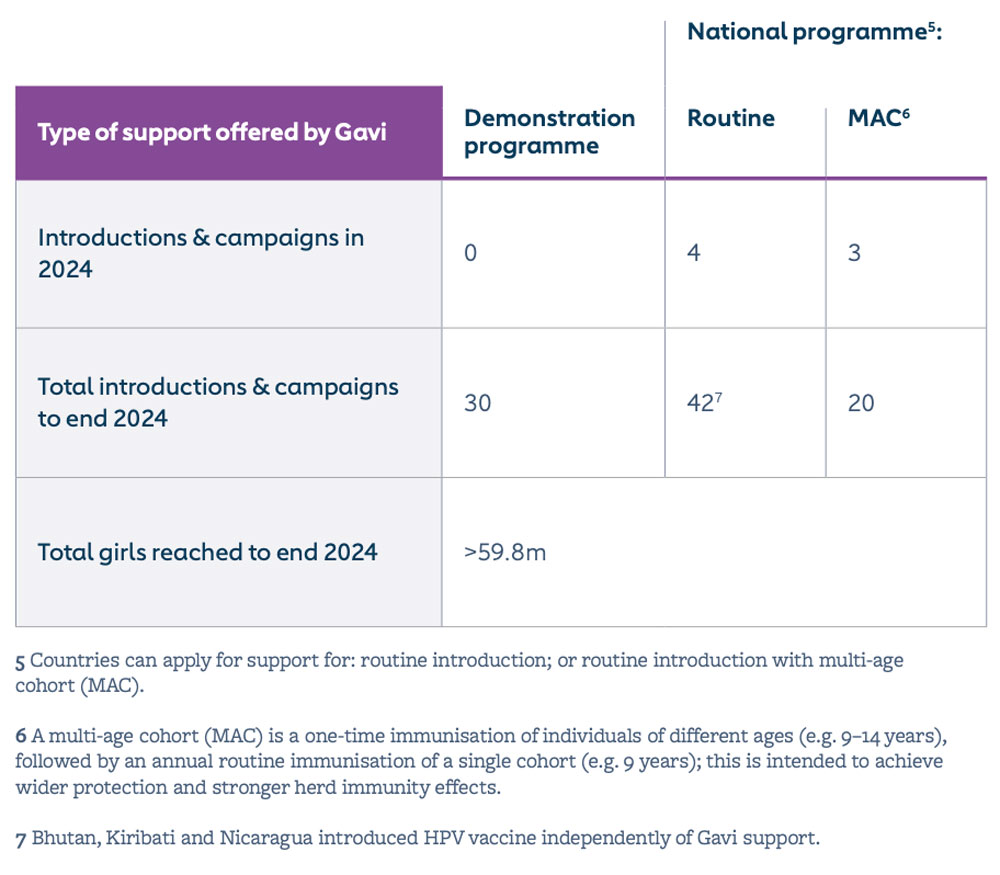
Human papillomavirus (HPV) vaccine coverage in the 57 lower-income countries supported by Gavi increased from 4% in 2019 to 8% in 2022, 16% in 2023 and to 25% in 2024. This was largely driven by switches to a one-dose schedule, as well as second phases of routine introductions in populous countries like Nigeria and Bangladesh. By end 2024, 42 countries had successfully launched their HPV vaccine national programme with Gavi support, fully immunising more than 59.8 million girls since 2014, which translates to over 1.2 million future cervical cancer deaths averted with Gavi support.
In a WHO position paper released in December 2022, the Strategic Advisory Group of Experts on Immunization (SAGE) recommended a one- or two-dose schedule for HPV vaccine. A single dose schedule greatly simplifies delivery of the vaccine, as you only need to reach a girl one time for full protection. In response to this potential gamechanger for Gavi’s HPV vaccine programme – and to overcome the challenges and impact of the COVID-19 pandemic on HPV vaccine coverage – in December 2022, the Gavi Board approved the revitalisation of Gavi’s HPV vaccine programme with a US$ 600+ million investment through 2025. Thanks in part to additional funding in place, the Alliance is on track to reach over 86 million girls with HPV vaccine by end of 2025, aiming to avert over 1.4 million future deaths from cervical cancer.
The issue
Cervical cancer is the fourth most common cancer in women globally, causing more than 209,000 deaths in 2022 in lower-income countries. HPV is associated with over 90% of these cancers, and vaccination provides high protection against cervical cancer. HPV vaccine has among the highest impact of all Gavi-supported vaccines, with 17.4 deaths averted per 1,000 children vaccinated, and is one of the key interventions towards achieving the global strategy for cervical cancer elimination.
Gavi’s response
Historically, the high cost of HPV vaccine, limited supply and challenges of reaching adolescent girls to deliver immunisation have been barriers to introduction in lower-income countries. Gavi is working to bridge the equity gap by providing support for national HPV vaccine introductions and ensuring sustainable prices. Gavi supports routine HPV vaccine delivery to a single cohort of girls (e.g. aged 9 years); and a multi-age cohort (MAC) (e.g. aged 10–14) in the year of introduction.
By (1) accelerating quality introductions; (2) rapidly improving global and national coverage; and (3) generating long-term programmatic sustainability, the revitalisation will allow Gavi to dedicate additional funding to help countries and partners reach more girls than ever with this life-saving vaccine. Support available under the US$ 600+ million revitalisation initiative includes expanded funding for vaccine purchasing, introduction and campaign activity costs, and adoption of the single dose-schedule; and expanded technical assistance from partners at regional, national and local levels. Gavi-eligible countries can also utilise health system strengthening (HSS) funding to develop tailored approaches to improve and sustain HPV vaccine coverage.
Lastly, Gavi is investing in implementation research focused on: strengthening integration of services for adolescents; integration of cervical cancer elimination strategies; and strengthening measurement of HPV vaccine coverage.
Gavi currently procures three HPV vaccines that have been prequalified by WHO. After severe supply constraints starting in 2017, HPV vaccine supply outlook is improving – supported by rapid uptake of the single-dose schedule, ramped up production from suppliers and WHO prequalification of new HPV vaccine products.
Gender and HPV vaccine
Not only does HPV vaccine prevent a major cause of female mortality, HPV vaccine delivery is also a touchpoint between adolescent girls and health services which can act as a bridge to improving women’s and girls’ health across the life course. It is an opportunity to build adolescents’ knowledge and trust in the healthcare system; deliver other essential health and education services; and empower girls through involving them in programme design and social mobilisation activities.
Social and cultural norms, and the unequal status of women in many societies, can reduce the chances of children and adolescents being vaccinated, by preventing girls and their caregivers from accessing immunisation services. For example, school-based vaccination programmes may miss girls who are not able to attend school due to gender-related barriers. Therefore, Gavi is investing in innovative approaches to reach out-of-school girls, and to achieve high and equitable coverage.
FROM OTHER SITES
- WHO Cervical Cancer Elimination Initiative
- WHO HPV Vaccine Introduction Clearing House
- WHO HPV Dashboard
- UNICEF Supply Division article on HPV vaccination
- HPV Vaccine Schedule Optimization Guide
- WHO position paper (2022)
- WHO considerations for HPV vaccine product choice (2nd edition)
- Global HPV Communication Resource
- Technet: HPV Vaccine Introduction Technical Resources
- Girl Focus Toolkit HPV Campaign Resource
FROM GAVI'S 2024 ANNUAL PROGRESS REPORT:
Latest articles about HPV
View moreNew study: HPV and measles vaccines top vaccine impact list
Researchers compared 14 vaccine programmes across 117 countries to estimate how many deaths and illnesses they prevent per 1,000 vaccinations.
Researchers reviewed hundreds of HPV vaccine studies. Here’s what they found
Drawing on more than 20 years of data, an independent review found strong evidence that HPV vaccines safely prevent cervical cancer.
As Burundi prepares to roll out vaccines against a leading cancer killer, survivors take stock
For Irakoze Gratia, diagnosis with cervical cancer was the start of a long, painful, expensive journey back to health. But as a survivor, she’s one of the lucky ones. She hopes the next generation won’t have to roll those dice.